Objective: Developmental trauma disorder (DTD) is an integrative syndrome for assessing the biopsychosocial sequelae of early life traumatization and attachment disruption. The psychometrics of a DTD Semi-Structured Interview (DTD-SI) and the validity and structure of the DTD construct were tested.
Methods: The DTD-SI was administered by research clinicians at 5 sites between September 2011 and August 2013 to a convenience sample of 236 children ages 7-17 years (50% female, 47% black or Latino/Hispanic, 91% with trauma histories) and/or a parent, recruited in pediatric or mental health services. Validity data were obtained from structured interviews for traumatic stressor and attachment disruption history (Traumatic Events Screening Instrument), DSM-IV disorders (Kiddie Schedule for Affective Disorders and Schizophrenia, Present/Lifetime Version), and potential alternative DSM-5 disorders; parent ratings on the Child Behavior Checklist; and child self-report on measures of emotion dysregulation and quality of life.
Results: Statistical analyses confirmed (a) the DTD-SI’s item-level temporal and interrater reliability, informativeness, and absence (with 1 exception) of demographic bias and (b) DTD construct factor structure, unidimensionality, and convergent and discriminant validity.
Conclusions: The DTD-SI yielded reliable, structurally meaningful, and valid item- and criterion-level data for the proposed DTD syndrome. Further clinical and scientific investigation of the clinical utility of DTD as a childhood psychiatric syndrome and diagnosis is warranted.

Toward an Empirically Based Developmental Trauma Disorder Diagnosis for Children:
Factor Structure, Item Characteristics, Reliability, and Validity of the Developmental Trauma Disorder Semi-Structured Interview

ABSTRACT
Objective: Developmental trauma disorder (DTD) is an integrative syndrome for assessing the biopsychosocial sequelae of early life traumatization and attachment disruption. The psychometrics of a DTD Semi-Structured Interview (DTD-SI) and the validity and structure of the DTD construct were tested.
Methods: The DTD-SI was administered by research clinicians at 5 sites between September 2011 and August 2013 to a convenience sample of 236 children ages 7-17 years (50% female, 47% black or Latino/Hispanic, 91% with trauma histories) and/or a parent, recruited in pediatric or mental health services. Validity data were obtained from structured interviews for traumatic stressor and attachment disruption history (Traumatic Events Screening Instrument), DSM-IV disorders (Kiddie Schedule for Affective Disorders and Schizophrenia, Present/Lifetime Version), and potential alternative DSM-5 disorders; parent ratings on the Child Behavior Checklist; and child self-report on measures of emotion dysregulation and quality of life.
Results: Statistical analyses confirmed (a) the DTD-SI’s item-level temporal and interrater reliability, informativeness, and absence (with 1 exception) of demographic bias and (b) DTD construct factor structure, unidimensionality, and convergent and discriminant validity.
Conclusions: The DTD-SI yielded reliable, structurally meaningful, and valid item- and criterion-level data for the proposed DTD syndrome. Further clinical and scientific investigation of the clinical utility of DTD as a childhood psychiatric syndrome and diagnosis is warranted.
J Clin Psychiatry 2018;79(5):17m11675
To cite: Ford JD, Spinazzola J, van der Kolk B, et al. Toward an empirically based developmental trauma disorder diagnosis for children: factor structure, item characteristics, reliability, and validity of the Developmental Trauma Disorder Semi-Structured Interview. J Clin Psychiatry. 2018;79(5):17m11675.
To share: https://doi.org/10.4088/JCP.17m11675
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, University of Connecticut School of Medicine, Farmington, Connecticut
bThe Foundation Trust, Melrose, Massachusetts
cBoston University School of Medicine, Boston, Massachusetts
*Corresponding author: Julian D. Ford, PhD, UCHC Department of Psychiatry MC1410, 263 Farmington Ave, Farmington, CT 06030 ([email protected]).
Children who experience potentially traumatic victimization (eg, maltreatment, family or community violence) are at risk for developing biopsychosocial and developmental problems that include, but extend beyond, posttraumatic stress disorder (PTSD).1-4 These children tend to be polydiagnosed in childhood5,6 and adolescence7 and subsequently as adults.8 However, trauma-focused treatments designed to remediate developmental deficits in self-regulation and relational security have demonstrated benefit with victimized children.9
Therefore, a developmentally adapted complex traumatic stress syndrome for children, developmental trauma disorder (DTD), has been proposed to guide assessment and treatment with victimized children.1,10 DTD was designed to differ from PTSD in content but parallel PTSD in structure, with a gateway criterion A representing stressor exposure followed by 3 symptom domains (criteria B, C, and D). DTD criterion A requires exposure to both interpersonal trauma (eg, maltreatment, family or community violence) and disruptions in the child’s development of attachment bonds with primary caregivers—a combination that has been shown to interfere with children’s mastery of stage-salient developmental tasks, including emotion regulation, attentional focusing, behavioral self-control, autonomy, socialization, and learning.1 DTD’s proposed symptom criteria B (affective/physiological dysregulation), C (cognitive/behavioral dysregulation), and D (self/relational dysregulation) parallel but differ from those proposed for adult complex PTSD.11 The proposed DTD stressor criterion and symptom criteria are described in Table 1.
An international survey of child-serving mental health and pediatric professionals was conducted12 as a first test of DTD’s incremental clinical utility,13 with survey ratings paralleling those from prior clinical utility surveys.14-16 Respondents evaluated the proposed DTD stressor and symptom criteria as feasible, unique, and value-added17—more parsimonious and accurate than other psychiatric diagnoses for characterizing treatment-refractory problems. Based on these findings, the present study investigated the reliability and validity of a new semistructured DTD clinical research interview (the DTD-SI) with a sample of children representing a range of ages, ethnocultural backgrounds, trauma histories, and psychiatric morbidity.
METHODS
Sample and Procedure
A convenience sample of families of 236 children ages 7-18 years (mean = 12.1, SD = 3.0; 50% female) from varied ethnocultural backgrounds (51% white non-Hispanic, 30% black, 16% Latino/Hispanic, 3% Asian American) was recruited between September 2011 and August 2013 at sites in 3 geographical regions in the United States (Northeast, Mid-Atlantic, South, Midwest) that represented a mix of urban, suburban, and rural communities. Parent/guardian consent and child assent were obtained with a protocol approved by a (blinded) institutional review board. Interviews were conducted with the child alone if requested by youths 14 years or older (n = 18), with 93 parent-child dyads conjointly, and with 125 parents alone. Most children were in outpatient psychiatric (n = 189, 80%) or residential (n = 23, 10%) treatment; 10% were referred by a pediatrician (n = 24). Most participants (78%) were not living with both birth parents but were living in a stepfamily (30%), foster or adoptive family (19%), or residential facility (29%). Interviews were conducted with the parent and child together (n = 93; 39%; ages 7-12 years old, child mean age = 10.4, SD = 2.6), the parent alone (n = 125; 53%; child mean age = 12.9, SD = 2.6), or the child alone (n = 18; 8%; child mean age = 15.2, SD = 1.8).
Interviewers viewed simulated demonstration interviews conducted by expert assessors, then independently rated videotaped interviews until they achieved > 80% agreement with expert ratings, then conducted videotaped role-play interviews with > 90% agreement required by an independent expert’s review and had their first 2 study interview tapes reviewed by an independent expert, with > 90% agreement required to be considered calibrated. A randomly selected 15% of the remaining interviews that included a parent (N = 13; 5 with the parent alone, and 8 with the parent and child together) and half of all interviews with a child alone (n = 9) were independently reviewed by an interviewer supervisor in order to ensure interrater reliability across the full set of study interviews. In total, interviews by 15 interviewers were re-rated.
Measures
Developmental Trauma Disorder Semi-Structured Interview. DTD-SI items were initially designed by experts from the National Child Traumatic Stress Network. After iterative review/revisions, DTD-SI version 10.018 was used in this study, representing 3 DTD symptom criteria sets (B, C, D): emotion/somatic, attentional/behavioral, and interpersonal/self-dysregulation (Table 1). Each symptom was assessed with an overview descriptive statement followed by optional probe questions. DTD criterion A was assessed by the TESI (see below).
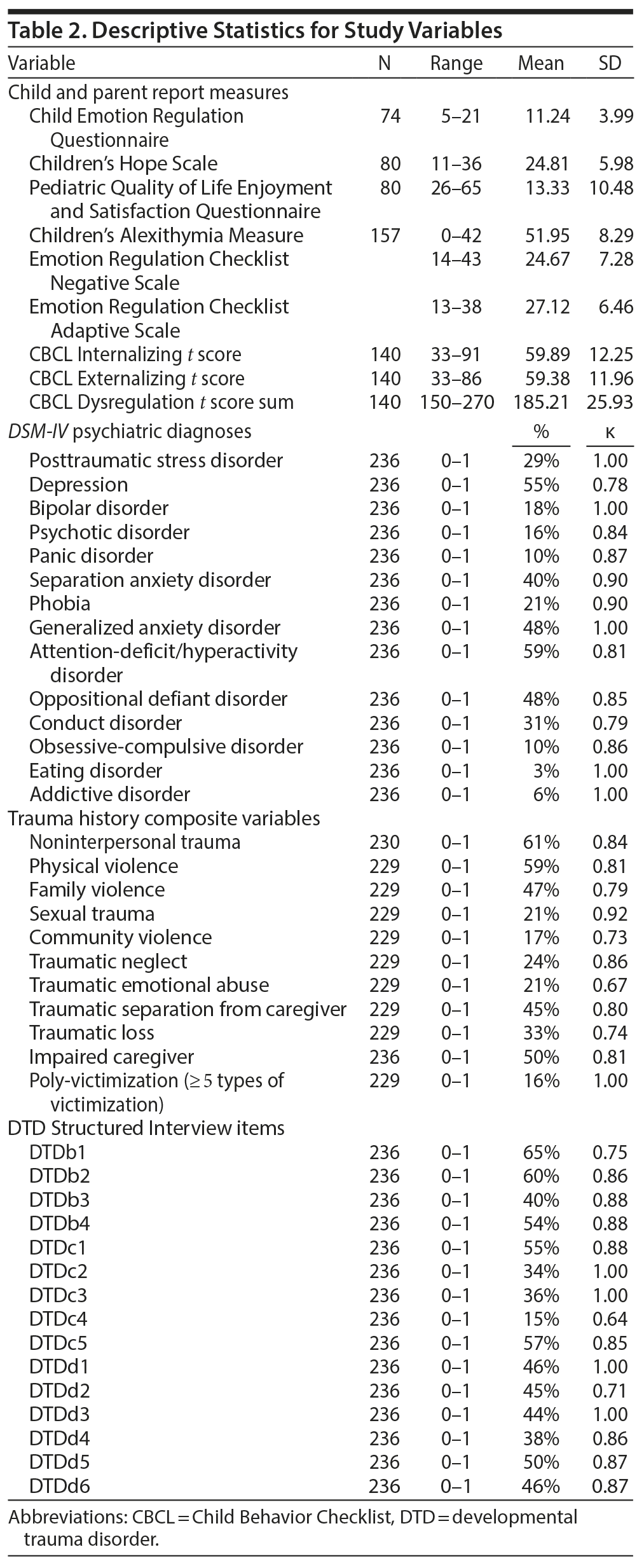
Traumatic Experiences Screening Instrument. This semistructured interview assesses 8 types of non-victimization adversity (accidents, illnesses, losses) and 13 types of interpersonal victimization. Traumatic Experiences Screening Instrument (TESI) items have shown evidence of retest reliability over a 2-4 month period (κ = 0.50-0.70) and criterion and predictive validity in psychiatric and pediatric samples.19,20 Interrater reliability for TESI composite scores in the current sample was κ = 0.67-1.00, median = 0.81 (see Table 2).

- Children who experience traumatic victimization and disrupted primary attachment relationships often receive multiple psychiatric diagnoses and are difficult to treat.
- Developmental trauma disorder provides a clinical framework for classification and treatment of complexly traumatized children.
- The Developmental Trauma Disorder Semi-Structured Interview is a psychometrically validated protocol for assessing the symptoms of complexly traumatized children.
Kiddie Schedule for Affective Disorders and Schizophrenia, Present/Lifetime Version. This semistructured interview assesses DSM-IV child psychiatric disorders with child and parent versions.21 PTSD symptoms and diagnoses were ascertained using the Kiddie Schedule for Affective Disorders and Schizophrenia, Present/Lifetime Version (K-SADS) module for PTSD. The child’s other internalizing and externalizing disorders were identified as probable vs absent using K-SADS screening questions for major depressive disorder, bipolar disorder, psychotic disorder, obsessive-compulsive disorder, panic disorder, social phobia, agoraphobia, generalized anxiety disorder, phobias, eating disorder, attention-deficit/hyperactivity disorder, oppositional defiant disorder, and conduct disorder. Interrater reliability was acceptable for PTSD diagnosis (κ = 1.00) and for K-SADS positive screens for each DSM-IV psychiatric disorder (κ = 0.78-1.00, median = 0.87). An internally consistent (α = .85) psychosocial impairment index was calculated with 8 K-SADS items for family, school, and peer functioning and emotional distress or behavioral avoidance.
Potential alternative DSM-5 disorders. Interviewers queried parent respondents using checklists with DSM-5 criteria to identify 4 disorders with core symptoms that closely parallel the proposed DTD symptoms. Potential DSM-5 diagnostic alternatives to DTD included 1 revised disorder (reactive attachment disorder; n = 8, 5% prevalence in the current sample), 2 new disorders (disinhibited social engagement disorder; n = 7, 4.5%; disruptive mood dysregulation disorder, n = 11, 7%), and 1 condition for further study (nonsuicidal self-injury, n = 9, 6%). Interrater reliability for the presence of these DSM-5 disorders was κ = 1.00.
Parent ratings. The Child Behavior Checklist (CBCL)22 is a 118-item parent/adult informant rating measure that assesses 8 factor analytically derived, internally consistent, and validated internalizing and externalizing dimensions (α = .84 and .87, respectively in this sample). A dysregulation score (α = .78) was calculated as a sum of the anxiety/depression, attention problems, and aggression CBCL subscale t scores.23 Parents also rated their child’s emotion-related capacities: (1) awareness/expression on the 14-item reliable (α = .94) and validated Children’s Alexithymia Measure24; and (2) dysregulation (10 items, α = .84) and (3) adaptive regulation (14 items, α = .87) on the reliable and validated Children’s Emotion Regulation Checklist.25,26 The CBCL could not be completed when only the child was interviewed (n = 18) and due to time limitations of the interview in 78 other cases.
Child self-report measures. Children self-rated their emotion regulation abilities using a 5-item abbreviated version of the reliable (α = .64) and cross-culturally validated Emotion Regulation Questionnaire.27 Child self-efficacy and optimism were assessed with the 6-item reliable (α = .78) and validated Children’s Hope Scale.28 Children rated their quality of life with the reliable (α = .86) and validated 13-item Pediatric Quality of Life Enjoyment and Satisfaction Questionnaire.29 Child self-ratings were not obtained when only the parent could be interviewed (n = 125) and due to time limitations on interviews that precluded administration of 1 or more of the questionnaires with 37 children.
Statistical Analyses
Confirmatory factor analysis was conducted to test the hypothesized 3-factor DTD symptom structure versus a 1-factor solution or a 4-factor hybrid solution modeled on the DSM-5 PTSD 4 symptom domains. For these analyses, a 10-point or greater difference in Bayesian information criterion (BIC) between non-nested models was used to indicate that the model with the smaller BIC was statistically superior with 150:1 odds.30 Multivariate linear regression analyses were used to identify the DTD symptom criteria that best predicted psychosocial impairment. DTD-SI convergent validity was tested with analyses of variance and child and parent ratings as dependent variables and a 3-level independent variable: (a) meets full criteria for DTD, (b) meets DTD exposure criterion A but not DTD symptom criteria, or (c) meets neither DTD exposure nor symptom criteria. Discriminant validity was tested with univariate and multivariate logistic regression analyses with the presence of any of the 4 alternative DSM-5 disorders as the independent variable. Item response theory (IRT) analysis was done to test DTD-SI item characteristics in relation to the underlying DTD dimension,31 considering 2 models (a 2-parameter logistic model and an unconstrained single-slope Rasch model32) and likelihood ratio tests. Differential item functioning (DIF) assessed whether items functioned differently between dichotomized demographic groups (age, race, and gender). Lord’s χ2 method was used to determine differential item function.33 IRT model fitting was carried out with the ltm package and DIF model fitting was carried out with the difR package34 in the statistical software R.35
RESULTS
Descriptive Statistics
One in 9 (n = 26; 11%) children had no psychiatric diagnosis, 14% (n = 33) screened positive for 1 psychiatric disorder, and 75% met criteria or screened positive for 2 or more (up to 10) psychiatric disorders (Table 2). Participants had a median of 3 psychiatric disorders. Almost all (91%) participants endorsed at least 1 traumatic event, with a median of 4.0 past types of traumatic events (mean [SD] = 4.8 [3.3]). A majority (58%) met the DTD exposure criterion.
DTD-SI Item and Diagnostic Reliability and Factor Structure
Interrater reliability was good (κ > 0.70) to excellent (κ = 0.88-1.00) for all DTD-SI items with 1 exception (Table 2), the rarely endorsed nonsuicidal self-injury item (κ = 0.64). Interrater reliability coefficients for the DTD syndrome and the presence of DTD symptom criteria B, C, and D were, respectively, κ = 1.00, 0.86, 0.71, and 0.71.
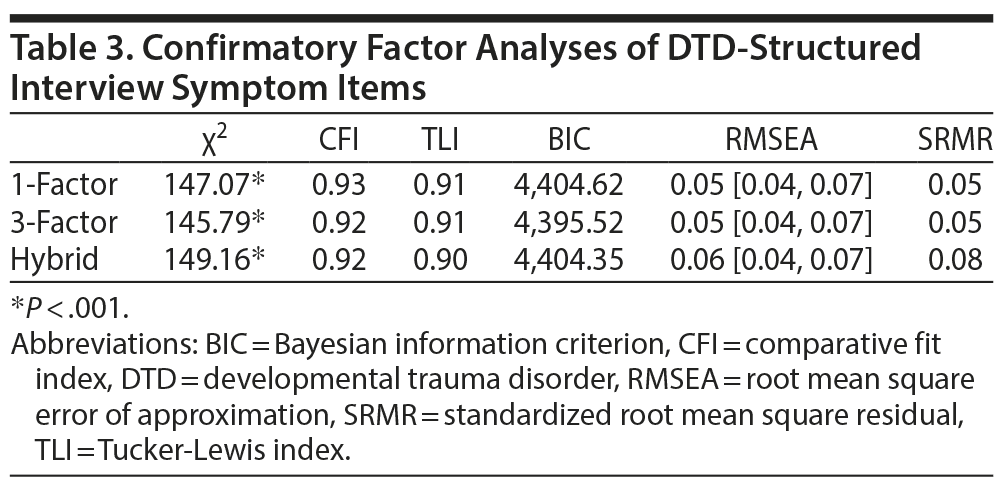
A 3-factor solution (versus 1-factor or a hybrid 4-factor modeled on the DSM-5 4-factor PTSD conceptualization) produced the best fit in the confirmatory factor analysis (Table 3). The 3-factor solution had a lower BIC than either alternative solution, a difference just below the conventional threshold of 10 points, and a higher Tucker-Lewis index (TLI), root mean square error of approximation (RMSEA), and standardized root mean square residual (SRMR) than the hybrid solution. Although the 1-factor solution had a higher comparative fit index than the 3-factor solution, they were equivalent on TLI, RMSEA, and SRMR, and the 3-factor solution had a lower χ2 than the 1-factor solution. Thus, while the 1-factor solution warrants further consideration (consistent with item analysis results indicating a unidimensional construct, see below), overall it appeared that the 3-factor solution best fit the data.
Each factor’s items, when scored as a simple count variable, comprised a scale that demonstrated moderate internal consistency (criterion B α = 67, criterion C α = 61, criterion D α = 72). Interitem correlations for each factor-based scale also were of moderate strength and statistically significant (criterion B: r = 0.24-0.42, P < .001; criterion C: r = 0.20-0.34, P < .01; criterion D: r = 0.23-0.39, P < .001) with 2 exceptions: the criterion C nonsuicidal self-injury symptom was uncorrelated with criterion C symptoms for insufficient self-protection and difficulty with completing goal-directed behavior (r = 0.07-0.08, P > .20)
DTD-SI Item Response Theory Analyses
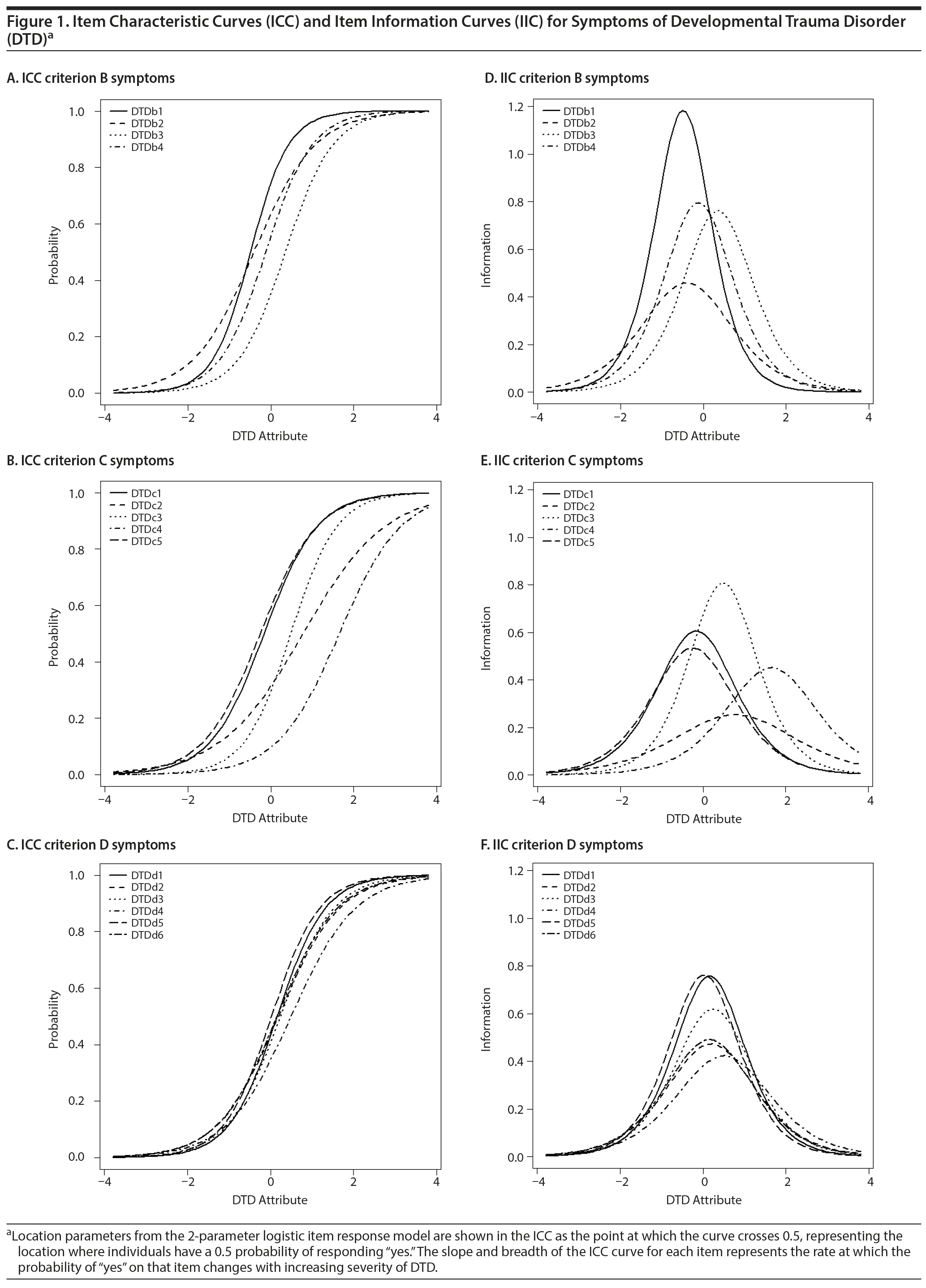
IRT item information function (IIF) analyses (Figure 1) using a 2-parameter logistic item response model (2-PL IRM) confirmed (1) the unidimensionality of the DTD construct with modified parallel analysis36 and scree plot analysis and (2) that all items were informative (maximum peak information > 20% of that of the maximally informative item) and (with 2 exceptions) unbiased in relation to demographics.37 Results from the 2-PL IRM, showing item characteristic curves and associated item information curves (IIC) (Figure 1), indicate that DTD-SI items discriminate individual differences across a spectrum of DTD severity. Criterion B item 1 was the most informative item for discriminating children scoring low on DTD severity (ie, maximal IIF height). All criteria B, C, and D items have maximum IIC information measure peaks no less than 20% of the IIC peak for the most informative item. DIF analyses on race (white vs nonwhite), gender, and age (pre-teen vs teenager) (Supplementary Figure 1) showed no differential functioning by DTD items by gender or race. Two items (DTDc5 and DTDd5) performed differently for children versus teens.
Empirical Evaluation of Alternative Algorithms for Classifying DTD Cases
Provisional DTD cases (N = 86, 36%) were identified using a conservative threshold for the hypothesized primary DTD component, criterion B emotion dysregulation symptoms (≥ 3 of 4 possible), and a less restrictive threshold for criterion C cognitive/behavioral and criterion D interpersonal/self-dysregulation (≥ 2 of 5 or 6 possible, respectively). These cut-points resulted in a minimum total DTD symptom count (ie, ≥ 7) that was above the sample median (median = 6.5).
Compared to children not meeting these DTD criteria, children classified as DTD cases had experienced 50% more types of potentially traumatic events (mean = 6.3 [3.5] vs mean = 4.0 [3.3], respectively; t228 = 5.00, P < .001) and twice as many types of interpersonal victimization (mean = 3.4 [2.4] vs mean = 1.9 [2.1], respectively; t228 = 4.88, P < .001).
Alternative classification algorithms were tested based on a more liberal B criterion (≥ 2 symptoms), or more conservative C/D criteria (≥ 3 symptoms). The DTD233 algorithm included both of these changes. Two other alternative algorithms retained the conservative B criterion (≥ 3 symptoms) but increased the threshold for either the C (DTD332) or D criteria (DTD323). The alternative algorithms reduced estimated DTD prevalence from N = 86 (36% of the sample) to N = 80 for DTD323 (34%), N = 68 for DTD233 (29%), and N = 63 for DTD 332 (27%).
All of the DTD classification algorithms were associated with DTD symptom burden in linear regression analyses controlling for DSM-IV diagnostic morbidity, DSM-5 alternative disorders, PTSD diagnosis, poly-victimization, and demographics (standardized B values = 0.54-0.60, P < .001). DTD233 and DTD332 were not included in further analyses due to not accounting for significant variance in psychosocial impairment in multivariate linear regression analyses.
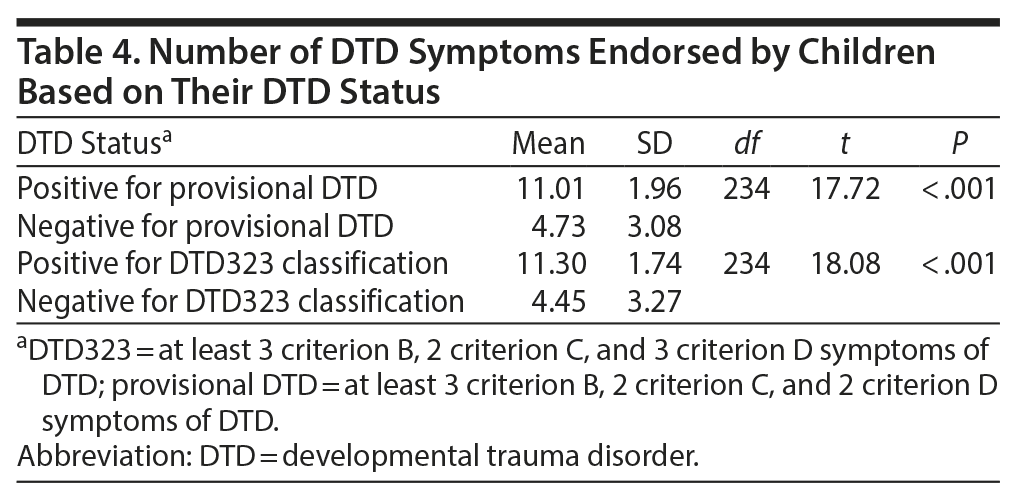
The provisional DTD and DTD323 algorithms accounted for significant variance in psychosocial impairment (R2 change = 0.19 for each) in multivariate regression analyses. All cases based on those algorithms had impairment in at least 1 psychosocial domain and met the DTD exposure criterion A. Cases identified based on either the provisional DTD or DTD323 algorithms also reported more than twice as many DTD symptoms as non-cases (Table 4).
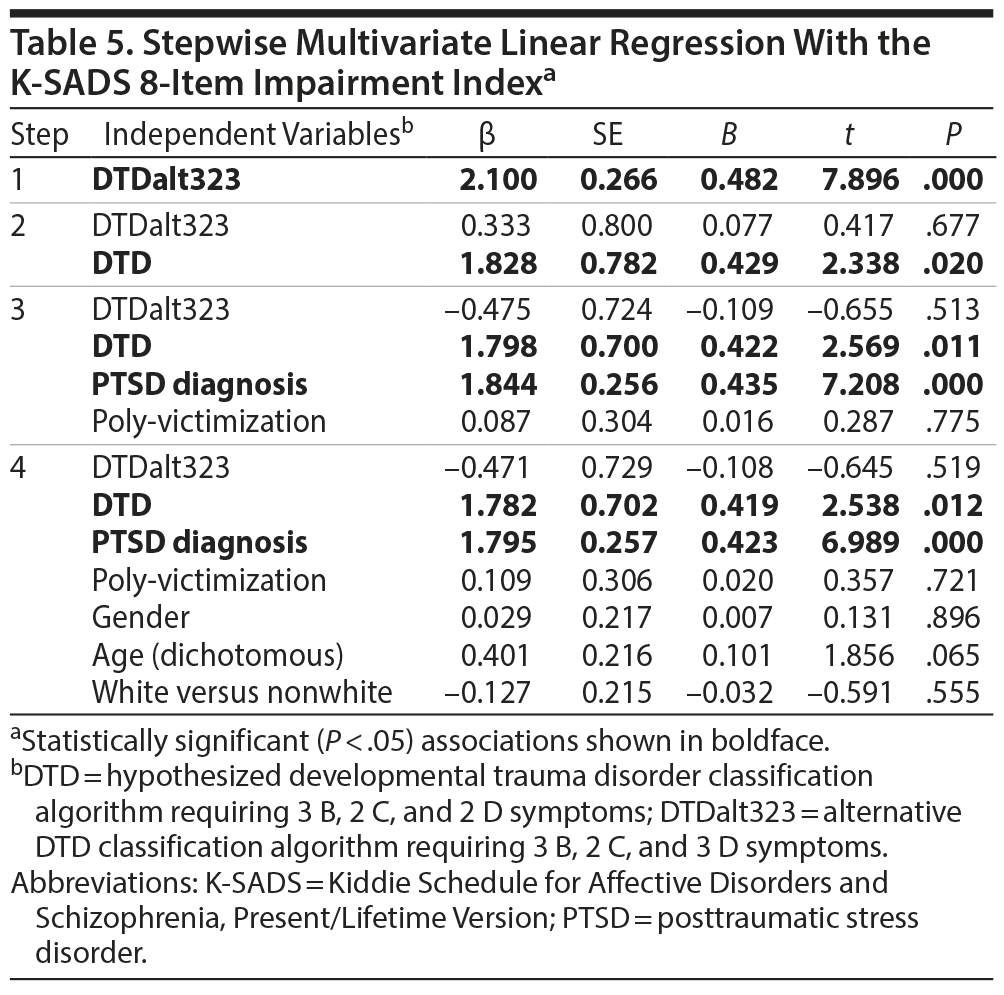
Finally, a stepwise multivariate regression was conducted with the K-SADS impairment index as the dependent variable and independent variables entered in the following steps: (1) DTD323 classification only; (2) DTD323 and provisional DTD; (3) DTD323, provisional DTD, and PTSD; and (4) DTD323, provisional DTD, PTSD, poly-victimization, and demographics (Table 5). Although DTD323 accounted for significant variance in the first step, in all subsequent steps in which the provisional DTD classification was entered DTD323 was nonsignificant and the provisional DTD classification was significant. In the final step, both the provisional DTD classification and the PTSD diagnosis were significantly associated with impairment (Table 4).
DTD Convergent Validity
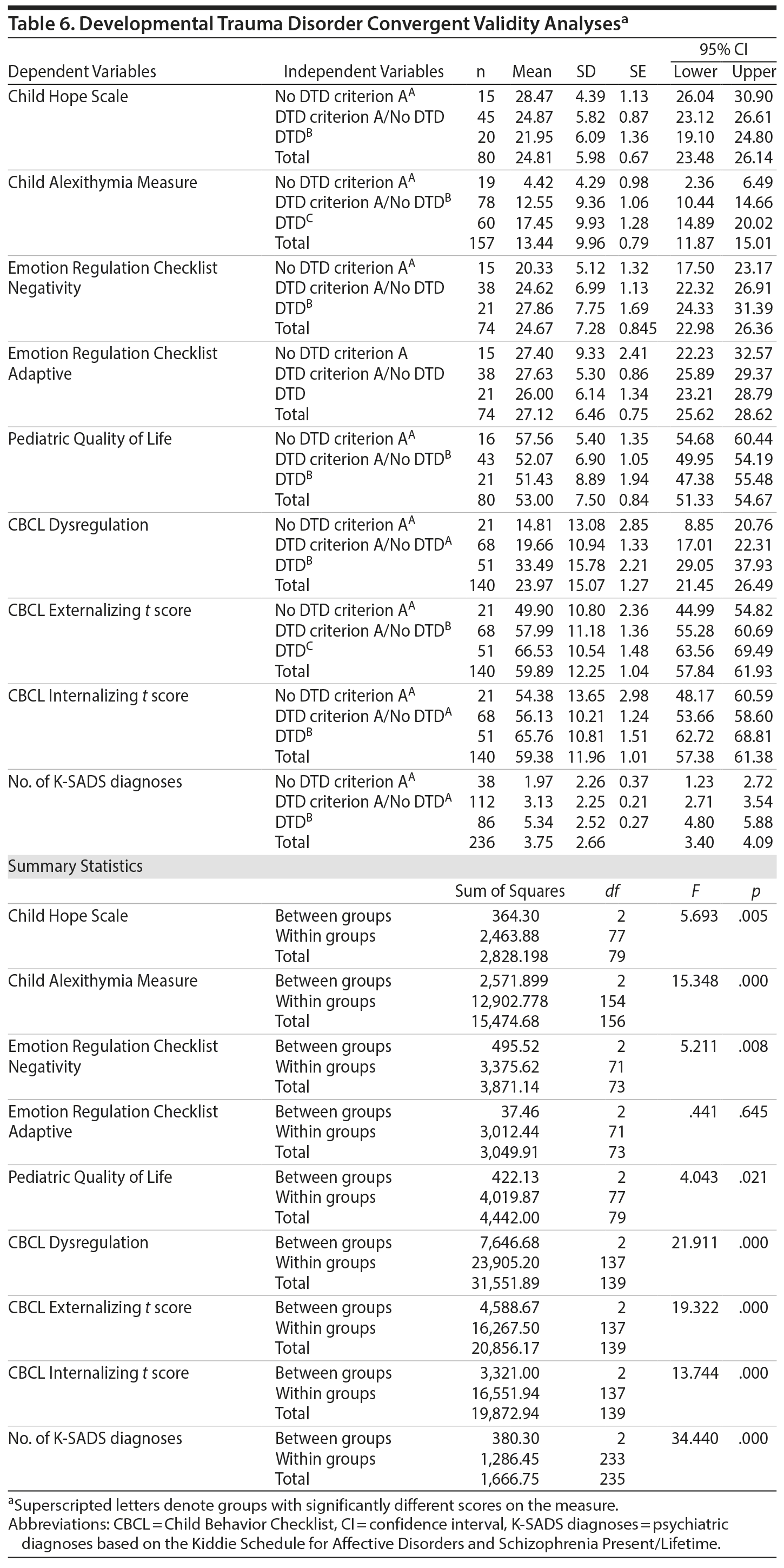
Convergent validity of the DTD algorithm was supported by analyses of variance showing significant differences between the subgroups defined by DTD status on all measures except child self-rated adaptive emotion regulation (Table 6). Compared to children who did not have lifetime adversities meeting DTD criterion A, DTD cases had lower levels of child self-reported hope and quality of life and higher levels of child self-reported negative emotion regulation, parent-reported dysregulation, internalizing symptoms, externalizing problems, and alexithymia, as well as more extensive psychiatric morbidity (ie, number of psychiatric diagnoses). On a more stringent test of convergent validity, compared to children who met DTD criterion A but not the DTD symptom criteria, DTD cases did not differ on child self-reported measures but had higher levels of parent-reported dysregulation, internalizing symptoms, externalizing problems, and alexithymia, as well as more extensive psychiatric morbidity.
DTD Discriminant Validity
DTD was unrelated to the presence of a DSM-5 alternative disorder on an unadjusted basis (OR = 1.74; 95% CI, 0.76-3.60). On the other hand, PTSD was associated with the presence of at least 1 DSM-5 alternative disorder on both an unadjusted (OR = 3.72; 95% CI, 1.60-8.62) and a multivariate (OR = 3.34; 95% CI, 1.36-8.20) basis. In the multivariate logistic regression, DTD was nonsignificant; age was the only significant covariate (OR = 2.80; 95% CI, 1.117-6.74). Thus, only PTSD, but not DTD, was strongly associated with the DSM-5 alternative disorders, suggesting that DTD is distinct from alternative DSM-5 disorders.
DISCUSSION
Study results support the DTD-SI’s reliability, construct (ie, factor analytic) validity, informativeness on an item-level basis, and convergent and discriminant validity. DTD was associated with psychosocial impairment independent of the effects of PTSD, poly-victimization, and demographics. DTD also was discriminable from alternative DSM-5 diagnoses that include some symptoms that closely parallel some DTD symptoms, whereas PTSD actually showed evidence of co-occurrence with those alternative DSM-5 diagnoses. Although the adult complex PTSD construct has been criticized as duplicative,38 study findings replicate and extend results of an international survey of child/family-serving clinicians who viewed DTD as related to but distinct from PTSD and both Axis I and Axis II DSM-IV psychiatric disorders.12 DTD therefore warrants further consideration as a distinct diagnostic syndrome that could enhance the assessment and treatment of victimized children.1,39
Consistent with the survey’s findings,12 all children who met DTD symptom criteria had histories of interpersonal victimization and attachment disruption. Children who met the DTD symptom criteria also had experienced twice as many types of interpersonal victimization as other children, consistent with an association of DTD with poly-victimization. In addition, independent of the effects of both PTSD and poly-victimization, meeting both the DTD exposure and symptom criteria was associated with psychosocial impairment. Thus, the proposed trauma antecedents of DTD are supported, and the symptoms of DTD account for psychosocial impairment over and above the effects of both poly-victimization and PTSD. Although both poly-victimization2,3,40 and PTSD41,42 are important to assess clinically with dysregulated children and adolescents, the study findings suggest that attachment disruption43-45 and DTD symptoms also should be considered clinically in assessing the full range of childhood adversities and their sequelae symptoms. Further research is needed to establish whether DTD is related to types of childhood adversities that are distinct from the antecedents of PTSD.1
Study results also supported the hypothesized symptom structure of DTD, with 3 interrelated but phenomenologically and empirically distinct domains of dysregulation: emotion/physiological, cognitive/behavioral, and interpersonal/self-identity.1 Additionally, each item in the DTD-SI was psychometrically informative in relation to overall DTD symptomatology. While requiring replication with both clinical and community/school or pediatric health care populations of children and adolescents, the findings support the conceptual and clinical integrity of DTD and its constituent symptoms. Interestingly, PTSD symptoms in the DSM-5 now include several symptoms similar to DTD symptoms (eg, pervasive negative emotions; preoccupation with blame; self-harm; reckless or aggressive behavior). However, DTD did not co-occur with DSM-5 diagnoses that included those symptoms, while the DSM-IV PTSD syndrome did show evidence of co-occurrence with those DSM-5 diagnoses. This suggests that DTD as an integrated syndrome may enable clinicians to identify features of biopsychosocial dysregulation that are not tapped by PTSD or by alternative DSM-5 diagnoses.12 Although the evidence of DTD’s discriminant validity in relation to both PTSD and alternative DSM-5 diagnoses is encouraging, whether DTD is sufficiently distinguishable from, and has incremental clinical utility beyond that of, those disorders to warrant a separate diagnosis requires further research.
Study limitations should be considered when interpreting the results. The sample was of convenience, primarily including children in psychiatric treatment with histories of exposure to traumatic stressors (ie, approximately 90%, in contrast to community prevalence estimates of 25%-70%41,46,47). Although several areas of the United States and both urban/suburban and rural areas were represented, the sample was not geographically dispersed across the United States.
The perspective of both the child and parent was included in a subset of cases, but most of the data were collected from either the child or parent but not both. Parent-child concordance on structured interviews of psychiatric symptoms tends to be weak, with each individual having unique information and perspectives such that combining data from both respondents tends to be optimal.48-50 Convergent validity was supported in relation to questionnaires completed by parents, but only partially for child self-report; the latter finding may be an artifact of reporter bias but also suggests a need for further testing of the DTD-SI with youths alone, which was possible in only a small number of cases (7.5% of the sample) in this study. Discriminant validity was tested with data from unvalidated checklists because validated structured interviews for DSM-5 dysregulation disorders were not available at the time of the study. Replication with these methodological concerns addressed is needed to further test the clinical utility of DTD.
Submitted: May 3, 2017; accepted March 13, 2018.
Published online: September 11, 2018.
Potential conflicts of interest: Dr Ford is co-owner of Advanced Trauma Solutions, Inc, the sole licensed distributor of the TARGET model copyrighted by the University of Connecticut. Other authors (Drs Spinazzola, van der Kolk, and Grasso), and named contributors (Drs Lynch and Pynoos), report no conflicts of interest.
Funding/support: The study was funded by contributions to the Justice Resource Institute by organizations and individuals (see www.jri.org); Julian Ford, PhD, and Bessel van der Kolk, MD, principal investigators.
Role of the sponsor: No organizational or individual funder had any role in the conduct or publication of this study.
Acknowledgments: The authors gratefully acknowledge the contributions of Miranda Lynch, PhD (University of Connecticut Health Center, Center for Biostatistics, Farmington, Connecticut), who conducted the item response theory analyses; the National Child Traumatic Stress Network Developmental Trauma Disorder Work Group, co-led by Robert Pynoos, MD (UCLA Department of Psychiatry, Los Angeles, California) and Dr van der Kolk to the conceptual framework and initial item development of the Developmental Trauma Disorder Semi-Structured Interview; and the field site coordinators and interviewers in Boston, Hartford, Houston, Kalamazoo, and Philadelphia who accomplished the data collection for this study.
Supplementary material: Available at PSYCHIATRIST.COM.
REFERENCES
1. D’ Andrea W, Ford J, Stolbach B, et al. Understanding interpersonal trauma in children: why we need a developmentally appropriate trauma diagnosis. Am J Orthopsychiatry. 2012;82(2):187-200. PubMed CrossRef
2. Turner HA, Finkelhor D, Ormrod R. Poly-victimization in a national sample of children and youth. Am J Prev Med. 2010;38(3):323-330. PubMed CrossRef
3. Ford JD, Elhai JD, Connor DF, et al. Poly-victimization and risk of posttraumatic, depressive, and substance use disorders and involvement in delinquency in a national sample of adolescents. J Adolesc Health. 2010;46(6):545-552. PubMed CrossRef
4. Finkelhor D, Turner H, Ormrod R, et al. Trends in childhood violence and abuse exposure: evidence from 2 national surveys. Arch Pediatr Adolesc Med. 2010;164(3):238-242. PubMed CrossRef
5. Cook A, Spinazzola J, Ford JD, et al. Complex trauma in children and adolescents. Psychiatr Ann. 2005;35(5):390-398. CrossRef
6. Ford JD, Connor DF, Hawke J. Complex trauma among psychiatrically impaired children: a cross-sectional, chart-review study. J Clin Psychiatry. 2009;70(8):1155-1163. PubMed CrossRef
7. Mueser KT, Taub J. Trauma and PTSD among adolescents with severe emotional disorders involved in multiple service systems. Psychiatr Serv. 2008;59(6):627-634. PubMed CrossRef
8. Sansone RA, Songer DA, Miller KA. Childhood abuse, mental healthcare utilization, self-harm behavior, and multiple psychiatric diagnoses among inpatients with and without a borderline diagnosis. Compr Psychiatry. 2005;46(2):117-120. PubMed CrossRef
9. Ford JD, Courtois CA, eds. Treating Complex Traumatic Stress Disorders in Children and Adolescents: Scientific Foundations and Therapeutic Models. New York, NY: Guilford; 2013.
10. van der Kolk BA. Developmental trauma disorder: toward a rational diagnosis for children with complex trauma histories. Psychiatr Ann. 2005;35(5):401-408. CrossRef
11. Ford JD. Complex PTSD: research directions for nosology/assessment, treatment, and public health. Eur J Psychotraumatol. 2015;6(1):27584. PubMed CrossRef
12. Ford JD, Grasso D, Greene C, et al. Clinical significance of a proposed developmental trauma disorder diagnosis: results of an international survey of clinicians. J Clin Psychiatry. 2013;74(8):841-849. PubMed CrossRef
13. First MB. Clinical utility: a prerequisite for the adoption of a dimensional approach in DSM. J Abnorm Psychol. 2005;114(4):560-564. PubMed CrossRef
14. Weinberger AH, Reutenauer EL, Vessicchio JC, et al. Survey of clinician attitudes toward smoking cessation for psychiatric and substance abusing clients. J Addict Dis. 2008;27(1):55-63. PubMed CrossRef
15. Mairs H, Lovell K, Keeley P. Clinician views of referring people with negative symptoms to outcome research: a questionnaire survey. Int J Ment Health Nurs. 2012;21(2):138-144. PubMed CrossRef
16. Cloitre M, Courtois CA, Charuvastra A, et al. Treatment of complex PTSD: results of the ISTSS expert clinician survey on best practices. J Trauma Stress. 2011;24(6):615-627. PubMed CrossRef
17. Regier DA, Narrow WE, Kuhl EA, et al. The conceptual development of DSM-V. Am J Psychiatry. 2009;166(6):645-650. PubMed CrossRef
18. Ford JD; Developmental Trauma Disorder Work Group. Developmental Trauma Disorder Semi-Structured Interview (DTD-SI). Farmington, CT: University of Connecticut Health Center, Center for the Treatment of Developmental Trauma Disorders; 2011.
19. Daviss WB, Racusin R, Fleischer A, et al. Acute stress disorder symptomatology during hospitalization for pediatric injury. J Am Acad Child Adolesc Psychiatry. 2000;39(5):569-575. PubMed CrossRef
20. Daviss WB, Mooney D, Racusin R, et al. Predicting posttraumatic stress after hospitalization for pediatric injury. J Am Acad Child Adolesc Psychiatry. 2000;39(5):576-583. PubMed CrossRef
21. Kaufman J, Birmaher B, Brent D, et al. Schedule for affective disorders and schizophrenia for school-age children-present and lifetime version (K-SADS-PL): initial reliability and validity data. J Am Acad Child Adolesc Psychiatry. 1997;36(7):980-988. PubMed CrossRef
22. Achenbach TM, Ruffle TM. The Child Behavior Checklist and related forms for assessing behavioral/emotional problems and competencies. Pediatr Rev. 2000;21(8):265-271. PubMed CrossRef
23. Masi G, Pisano S, Milone A, et al. Child behavior checklist dysregulation profile in children with disruptive behavior disorders: a longitudinal study. J Affect Disord. 2015;186:249-253. PubMed CrossRef
24. Way I, Black-Pond C, Applegate B, et al. Children’s Alexithymia Measure (CAM): a new instrument for screening difficulties with emotional expression. J Child Adolesc Trauma. 2010;3(4):303-318. CrossRef
25. Shields A, Cicchetti D. Emotion regulation among school-age children: the development and validation of a new criterion Q-sort scale. Dev Psychol. 1997;33(6):906-916. PubMed CrossRef
26. Suveg C, Zeman J. Emotion regulation in children with anxiety disorders. J Clin Child Adolesc Psychol. 2004;33(4):750-759. PubMed CrossRef
27. Spaapen DL, Waters F, Brummer L, et al. The Emotion Regulation Questionnaire: validation of the ERQ-9 in two community samples. Psychol Assess. 2014;26(1):46-54. PubMed CrossRef
28. Snyder CR, Hoza B, Pelham WE, et al. The development and validation of the Children’s Hope Scale. J Pediatr Psychol. 1997;22(3):399-421. PubMed CrossRef
29. Endicott J, Nee J, Yang R, et al. Pediatric Quality of Life Enjoyment and Satisfaction Questionnaire (PQ-LES-Q): reliability and validity. J Am Acad Child Adolesc Psychiatry. 2006;45(4):401-407. PubMed CrossRef
30. Volinsky CT, Raftery AE. Bayesian information criterion for censored survival models. Biometrics. 2000;56(1):256-262. PubMed CrossRef
31. Cappelleri JC, Jason Lundy J, Hays RD. Overview of classical test theory and item response theory for the quantitative assessment of items in developing patient-reported outcomes measures. Clin Ther. 2014;36(5):648-662. PubMed CrossRef
32. Petrillo J, Cano SJ, McLeod LD, et al. Using classical test theory, item response theory, and Rasch measurement theory to evaluate patient-reported outcome measures: a comparison of worked examples. Value Health. 2015;18(1):25-34. PubMed CrossRef
33. Lord F. Applications of Item Response Theory to Practical Testing Problems. Hillsdale, NJ: Lawrence Erlbaum Associates; 1980.
34. Magis D, Béland S, Tuerlinckx F, et al. A general framework and an R package for the detection of dichotomous differential item functioning. Behav Res Methods. 2010;42(3):847-862. PubMed CrossRef
35. Rizopoulos D. ltm: An R package for latent variable modelling and item response theory analyses. J Stat Softw. 2006;17(5):1-25. CrossRef
36. Medina-Mirapeix F, Navarro-Pujalte E, Escolar-Reina P, et al. Mobility activities measurement for outpatient rehabilitation settings. Arch Phys Med Rehabil. 2011;92(4):632-639. PubMed CrossRef
37. Prigerson HG, Horowitz MJ, Jacobs SC, et al. Prolonged grief disorder: Psychometric validation of criteria proposed for DSM-V and ICD-11. PLoS Med. 2009;6(8):e1000121. PubMed CrossRef
38. Resick PA, Bovin MJ, Calloway AL, et al. A critical evaluation of the complex PTSD literature: implications for DSM-5. J Trauma Stress. 2012;25(3):241-251. PubMed CrossRef
39. Ford JD, Blaustein M, Habib M, et al. Developmental trauma-focused treatment models. In: Ford JD, Courtois CA, eds. Treating Complex Traumatic Stress Disorders in Children and Adolescents: Scientific Foundations and Therapeutic Models. New York, NY: Guilford; 2013:261-276.
40. Gustafsson PE, Nilsson D, Svedin CG. Polytraumatization and psychological symptoms in children and adolescents. Eur Child Adolesc Psychiatry. 2009;18(5):274-283. PubMed CrossRef
41. McLaughlin KA, Koenen KC, Hill ED, et al. Trauma exposure and posttraumatic stress disorder in a national sample of adolescents. J Am Acad Child Adolesc Psychiatry. 2013;52(8):815-830.e14, e14. PubMed CrossRef
42. Copeland WE, Keeler G, Angold A, et al. Traumatic events and posttraumatic stress in childhood. Arch Gen Psychiatry. 2007;64(5):577-584. PubMed CrossRef
43. van Dijke A, Ford JD, Frank LE, et al. Association of childhood complex trauma and dissociation with complex posttraumatic stress disorder symptoms in adulthood. J Trauma Dissociation. 2015;16(4):428-441. PubMed CrossRef
44. Van Dijke A, Ford JD, Frank L, et al. Association of childhood trauma-by-primary-caregiver and affect dysregulation with borderline personality disorder symptoms in adulthood. Psychol Trauma. 2013;5(3):217-224. CrossRef
45. Spinazzola J, Hodgdon H, Liang L, et al. Unseen wounds: The contribution of psychological maltreatment to child and adolescent mental health and risk outcomes. Psychol Trauma. 2014;6(suppl 1):518-528. CrossRef
46. Costello EJ, Erkanli A, Fairbank JA, et al. The prevalence of potentially traumatic events in childhood and adolescence. J Trauma Stress. 2002;15(2):99-112. PubMed CrossRef
47. Saunders BE, Adams ZW. Epidemiology of traumatic experiences in childhood. Child Adolesc Psychiatr Clin N Am. 2014;23(2):167-184, vii. PubMed CrossRef
48. Safford SM, Kendall PC, Flannery-Schroeder E, et al. A longitudinal look at parent-child diagnostic agreement in youth treated for anxiety disorders. J Clin Child Adolesc Psychol. 2005;34(4):747-757. PubMed CrossRef
49. Edelbrock C, Costello AJ, Dulcan MK, et al. Parent-child agreement on child psychiatric symptoms assessed via structured interview. J Child Psychol Psychiatry. 1986;27(2):181-190. PubMed CrossRef
50. Braet C, Soetens B, Moens E, et al. Are two informants better than one? Parent-child agreement on the eating styles of children who are overweight. Eur Eat Disord Rev. 2007;15(6):410-417. PubMed CrossRef
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Childhood and Adolescent Mental Health section. Please contact Karen D. Wagner, MD, PhD, at [email protected].
This PDF is free for all visitors!
Save
Cite