Objective: To evaluate the relationships between benzodiazepine use and (1) health care utilization and (2) suicide risk in veterans diagnosed with posttraumatic stress disorder (PTSD).
Methods: This propensity-matched retrospective cohort study included veterans diagnosed with 1 ICD-9 code for PTSD who were active users of the Veterans Affairs health care system between January 1, 2001, and December 31, 2014. Exposure included at least 1 thirty-day prescription of a benzodiazepine within 1 year following PTSD diagnosis among patients with no recent history of benzodiazepine use. The primary outcomes were health care utilization and suicidal behavior.
Results: A total of 242,493 of 1,134,201 eligible veterans were included in the propensity-matched cohort, 80,831 (7.13%) of whom were prescribed benzodiazepines. Veterans with PTSD who received benzodiazepines had significantly more hospitalizations (incident rate ratio [IRR] = 1.27; 95% CI, 1.10-1.47) and emergency department (IRR = 1.16; 95% CI, 1.13-1.20), general outpatient (IRR = 1.19; 95% CI, 1.16-1.21), outpatient mental health (IRR = 1.49; 95% CI, 1.41-1.57), and total mental health (IRR = 1.37; 95% CI, 1.34-1.40) visits. Benzodiazepine users had a significantly greater risk of death due to suicide (hazard ratio [HR] = 2.74; 95% CI, 2.40-3.13) and were significantly more likely to have medically documented suicide attempts (HR = 1.85; 95% CI, 1.65-2.08) and suicidal ideation (HR = 1.57; 95% CI, 1.48-1.67).
Conclusions: Benzodiazepine users had higher rates of health care utilization and were more likely to attempt and complete suicide than patients without benzodiazepine exposure. This study strengthens the empirical evidence against the use of benzodiazepines in veterans with PTSD. Prescribers should weigh the benefits and risks—especially the almost 3-fold increase in suicide risk—when prescribing benzodiazepines in these patients.

Benzodiazepines, Health Care Utilization, and Suicidal Behavior in Veterans With Posttraumatic Stress Disorder

ABSTRACT
Objective: To evaluate the relationships between benzodiazepine use and (1) health care utilization and (2) suicide risk in veterans diagnosed with posttraumatic stress disorder (PTSD).
Methods: This propensity-matched retrospective cohort study included veterans diagnosed with 1 ICD-9 code for PTSD who were active users of the Veterans Affairs health care system between January 1, 2001, and December 31, 2014. Exposure included at least 1 thirty-day prescription of a benzodiazepine within 1 year following PTSD diagnosis among patients with no recent history of benzodiazepine use. The primary outcomes were health care utilization and suicidal behavior.
Results: A total of 242,493 of 1,134,201 eligible veterans were included in the propensity-matched cohort, 80,831 (7.13%) of whom were prescribed benzodiazepines. Veterans with PTSD who received benzodiazepines had significantly more hospitalizations (incident rate ratio [IRR] = 1.27; 95% CI, 1.10-1.47) and emergency department (IRR = 1.16; 95% CI, 1.13-1.20), general outpatient (IRR = 1.19; 95% CI, 1.16-1.21), outpatient mental health (IRR = 1.49; 95% CI, 1.41-1.57), and total mental health (IRR = 1.37; 95% CI, 1.34-1.40) visits. Benzodiazepine users had a significantly greater risk of death due to suicide (hazard ratio [HR] = 2.74; 95% CI, 2.40-3.13) and were significantly more likely to have medically documented suicide attempts (HR = 1.85; 95% CI, 1.65-2.08) and suicidal ideation (HR = 1.57; 95% CI, 1.48-1.67).
Conclusions: Benzodiazepine users had higher rates of health care utilization and were more likely to attempt and complete suicide than patients without benzodiazepine exposure. This study strengthens the empirical evidence against the use of benzodiazepines in veterans with PTSD. Prescribers should weigh the benefits and risks—especially the almost 3-fold increase in suicide risk—when prescribing benzodiazepines in these patients.
J Clin Psychiatry 2018;79(6):17m12038
To cite: Deka R, Bryan CJ, LaFleur J, et al. Benzodiazepines, health care utilization, and suicidal behavior in veterans with posttraumatic stress disorder. J Clin Psychiatry. 2018;79(6):17m12038.
To share: https://doi.org/10.4088/JCP.17m12038
© Copyright 2018 Physicians Postgraduate Press, Inc.
aVA San Diego Health Care System, La Jolla, California
bVA Salt Lake City Health Care System, Salt Lake City, Utah
cDepartment of Radiation Medicine and Applied Sciences, University of California San Diego School of Medicine, La Jolla, California
dDepartment of Pharmacotherapy, Pharmacotherapy Outcomes Research Center, University of Utah College of Pharmacy, Salt Lake City, Utah
eNational Center for Veterans Studies, University of Utah, Salt Lake City, Utah
fDepartment of Psychology, University of Utah, Salt Lake City, Utah
gDivision of Epidemiology, University of Utah School of Medicine, Salt Lake City, Utah
*Corresponding author: Rishi Deka, PhD, Department of Radiation Medicine and Applied Sciences, University of California San Diego School of Medicine, 9500 Gilman Drive, La Jolla, CA 92093 ([email protected]).
PTSD is a debilitating and prevalent psychiatric disorder among military personnel and veterans.1 As compared to the general population, veterans have a 2 to 3 times greater risk of developing PTSD.1-3 According to the US Department of Veterans Affairs (VA), a veteran is diagnosed with PTSD if he or she experiences a cluster of symptoms that have persisted for more than 1 month after a traumatic event and caused significant impairment in social, occupational, or other important areas of functioning.1 This cluster includes 1 intrusion symptom (recurrent memories, recurrent dreams, dissociative reactions, or psychological distress), 1 avoidance symptom (avoidance of distressing memories or external reminders), 2 or more negative alterations in cognition/mood (negative beliefs, negative emotional state, detachment from others, diminished interest in activities, or inability to experience positive emotions), and 2 or more alterations in arousal/reactivity (irritable behavior, hypervigilance, problems with concentration, or sleep disturbance).1 Estimates on the cost of PTSD among military personnel due to medical care, lost productivity, and suicide range from $2 to $3 billion per year.4 Veterans suffering from PTSD have increased health care utilization and are 3 times as likely to experience suicidal behavior compared to veterans without PTSD.5-8 Data further indicate that veterans are significantly more likely to die by suicide than the US general population.6 Thus, understanding modifiable risk factors for suicidal behavior among these patients is a major focus for the VA and its mental health providers.
According to the 2010 VA Clinical Practice Guidelines,9 trauma-focused psychotherapy is the recommended first-line treatment for PTSD; this includes cognitive processing therapy (CPT) and prolonged exposure (PE). While psychotherapy is the recommended first-line treatment for PTSD, pharmacotherapy is also an important treatment option.9. First-line recommended pharmacotherapies include the selective serotonin reuptake inhibitors (SSRIs) sertraline, paroxetine, fluoxetine, citalopram, and fluvoxamine and the serotonin-norepinephrine reuptake inhibitor (SNRI) venlafaxine.9 If none of these first-line agents are effective, a second-line agent is the next step of treatment.9 Prazosin is recommended for nightmares not relieved by first-line medications; other second-line agents include mirtazapine, nefazodone, and tricyclic antidepressants (eg, imipramine, amitriptyline).9 Benzodiazepines, conventional antipsychotics, and atypical antipsychotics are not recommended for the treatment of PTSD.9,10 Furthermore, opioids should be used cautiously, and only for a short duration, due to impairment of cognitive performance.9
Despite the abundance of psychotherapy and pharmacologic options available, delivering effective treatment to patients in need remains a significant challenge. In cases in which first- and second-line agents inadequately manage symptoms, providers may reach for alternative treatment options such as benzodiazepines in the search for short-term symptomatic relief. Although benzodiazepines can provide short-term relief for anxiety, they are not recommended for the treatment of PTSD, in part because they are not effective in treating the 4 core symptom clusters of PTSD.9,10 Furthermore, benzodiazepines are associated with worse overall symptom severity, anxiety, aggression, substance abuse, and social functioning.9-15 Benzodiazepines have also been known to cause or worsen depression, dissatisfaction with life, and suicidal thoughts and behaviors, all of which can increase the risk for suicide.9,10,15 This is especially problematic because veterans are already at an elevated risk for suicide, and depression is comorbid in 30%-50% of patients with PTSD.9,10,15 Despite these concerns, benzodiazepines are still prescribed to some veterans with PTSD.9,10,15 Thus, the purpose of this study is to evaluate the potential consequences of benzodiazepine use, including increased health care utilization and suicide risk, in veterans diagnosed with PTSD.
METHODS
Study Design and Participants
This study was a retrospective analysis of veterans diagnosed with PTSD between January 1, 2001, and December 31, 2014. The study population consisted of veterans with PTSD who were active VA utilizers. A veteran was considered to be an active VA utilizer if he or she had at least 6 months of VA care at any point in time during the study time period in any inpatient or outpatient setting and had at least 1 visit 12 months prior to his or her first PTSD diagnosis. The International Classification of Diseases, Ninth Revision Clinical Modification (ICD-9-CM) code for PTSD (309.81) was used to identify veterans with PTSD. Research indicates that 75% of Veterans Health Administration (VHA) users with an ICD-9 code for PTSD also meet diagnostic criteria for PTSD on other validated measures.16
This study was reviewed and approved by the University of Utah Institutional Review Board and the Research and Development Committee of the VA Salt Lake City Health Care System. Waivers of consent and authorization were granted by the University of Utah Institutional Review Board and the Research and Development Committee of the VA Salt Lake City Health Care System. Study data were not deidentified.

- Understanding modifiable risk factors for suicidal behavior, such as benzodiazepine use, in patients with posttraumatic stress disorder (PTSD) is a major focus for the US Department of Veterans Affairs and its mental health providers.
- Prescribers should carefully weigh the benefits and risks of prescribing a benzodiazepine, particularly the increased risk of suicide, among veterans diagnosed with PTSD.
Study Data
All study data were extracted from the VA’s Corporate Data Warehouse (CDW) and the VA/Department of Defense (DOD) Suicide Data Repository (SDR) and accessed through the VA Informatics and Computing Infrastructure (VINCI), which provides database management and statistical analysis tools within a central, secure location inside the VA firewall.17 The CDW contains electronic health records of over 20 million veterans from the years 2000-2015; these veterans have sought health care at the 1,400 VA outpatient facilities and 152 medical centers throughout the United States.18 The VA/DOD SDR includes the National Death Index Plus, which contains all-cause mortality for all service members who separated from military service between the years 1979 and 2014. It also contains a current mortality archive on all users of VHA services from 2000 to 2014.19
The exposed group included new users of benzodiazepines. Exposure was assessed in the year following PTSD diagnosis. Patients who received at least one 30-day prescription for benzodiazepines during this window were considered benzodiazepine users, whereas patients without at least one 30-day prescription during this time were considered nonusers. The index date was defined as the date of benzodiazepine prescription. The index date for the benzodiazepine nonusers corresponded to the matched benzodiazepine user’s first prescription date. The comparator group included VA utilizers with PTSD who did not receive a benzodiazepine prescription during the study time period. Patients were followed from index until the end of study or death.
The primary outcomes of interest were suicide death and measures of health care utilization (HCU). Outcomes were assessed starting at the benzodiazepine initiation date (or the corresponding index date for nonusers) and followed through a veteran’s last health care encounter or until the end of the study period, whichever came first. Suicide death was established using records contained within the VA/DOD SDR.19 HCU, measured over a 6-year follow-up time period, included hospitalizations, emergency department visits, general non-mental health outpatient visits, mental health outpatient visits, substance abuse outpatient visits, and total mental health outpatient visits. VA clinic codes were used to identify the different types of visits in the CDW.
Statistical Analysis
In observational data, treatment assignment is not random.20 If not accounted for, nonrandom assignment can lead to confounding bias if measured and unmeasured characteristics of individuals are associated with the outcome and with the probability of receiving treatment. Thus, statistical methods must be employed to reduce confounding bias in observational studies.21 Propensity scores mimic a randomized controlled trial by balancing measured covariates across treatment and comparison groups, thereby making the 2 groups similar to each other, conditional on a set of variables that systematically differ between these groups.21-23 In the propensity score model, the recommended variable selection strategy is to include all variables associated with the outcomes of interest—health care utilization and suicide—regardless of their association with exposure.21-23 Thus, the variables chosen in the propensity score for this study included demographics, comorbidities, and other therapies. These covariates were captured in the 12-month period prior to PTSD diagnosis. Traumatic brain injury, anxiety disorder, bipolar disorder, depression, alcohol abuse, opioid abuse, chronic pain, homelessness, smoking, and illicit drug use were identified using ICD-9 codes. SSRI, SNRI, prazosin, opioid, atypical antipsychotic, and conventional antipsychotic use were ascertained from medication prescription fills in the VA CDW. Age, sex, socioeconomic status, service percentage disabilities, race, and military sexual trauma (sexual assault) were directly identified using standard fields in the VA CDW. Socioeconomic status was assigned to each zip code based on census variables from the American Community Survey.24 Service disabilities were categorized according to the proportion of the disability that is estimated to be due to military service; disabilities included physical health conditions that were incurred or aggravated during active duty service. Disability ratings were categorized to low percentage (0-29), medium percentage (30-59), and high percentage (60-100).
The impact of benzodiazepine use in veterans with PTSD was assessed in a 1:2 propensity score-matched cohort using regression models. Health care visits and suicide death were modeled as a function of benzodiazepine use, traumatic brain injury, anxiety disorder, bipolar disorder, depression, alcohol abuse, opioid abuse, chronic pain, SSRI use, SNRI use, prazosin use, atypical antipsychotic use, conventional antipsychotic use, opioids use, sex, marital status, race, service percentage disabilities, age, socioeconomic status, smoking status, homelessness, illicit drug use, and military sexual trauma. Incidence rate ratios and hazard ratios were used to estimate the effect of benzodiazepine use on the outcomes of interest.
The appropriate distribution for each HCU outcome was chosen using modified Park tests and analyzed using generalized linear models; incidence rate ratios (IRRs) were reported for these different types of visits.25,26 The IRR can be interpreted as the ratio of the number of health care visits per population at risk among patients prescribed benzodiazepines to the number of health care visits per population at risk among patients not prescribed benzodiazepines over the study period.25,26 Because suicide death constitutes a time-to-event outcome, these were estimated through hazard ratios from a Cox proportional hazards regression model.25,26 The hazard ratio (HR) is the ratio of the instantaneous rates of suicide among benzodiazepine users compared to nonusers at any point in time during the study.25,26 Numbers needed to harm (NNHs) for all-cause and suicide mortality were calculated using risk differences estimated from fully adjusted log binomial regression models.25,26
Sensitivity Analyses
To account for potential variability in methods of documentation of suicide-related outcomes, sensitivity analyses were conducted using a variety of methods to identify suicidal behavior. The VA employs a number of standard clinical note templates to describe and report on suicidal ideation and behavior. We used a combination of clinical note titles suggestive of suicidal behavior and ICD-9 codes to identify suicide attempts and suicidal ideation. First, we searched for electronic medical record (EMR) note titles with the combination of terms (suicide) and (consult, event, attempt, flag, alert, warning, or report).18,19 Second, we searched for ICD-9 codes that designate suicidal behavior (E950-E959 for suicide attempts and v62.84 for suicidal ideation). Additional statistical models were constructed for each outcome using the alternative identification methods to determine the impact of outcome assessment method on the results.
All statistical analyses were performed using SAS V9.3 (Cary, North Carolina) and Stata 13 (College Station, Texas), assuming a 2-sided α of .05. Approval for this study was obtained from the Institutional Review Board at the University of Utah and the Research & Development committee at the Salt Lake City VA. Approval for the use of the VA/DOD suicide data repository was obtained from the US Department of Defense Suicide Prevention Office.
RESULTS
Patients
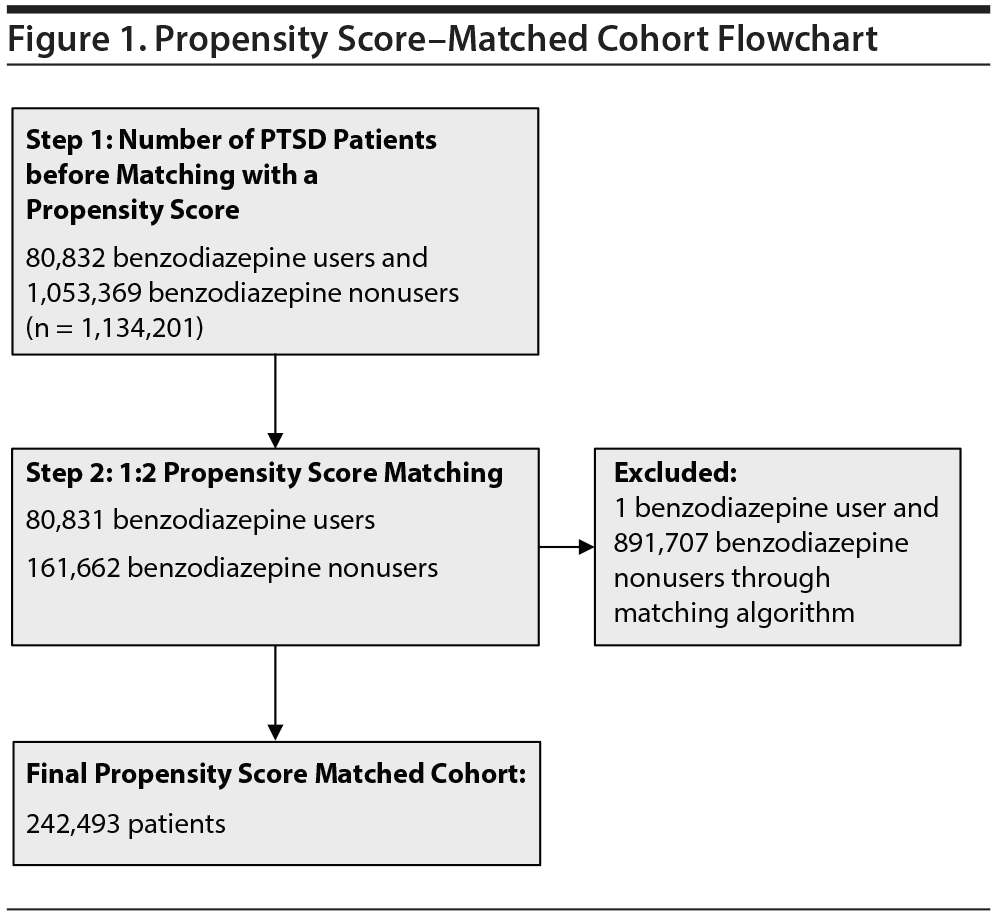
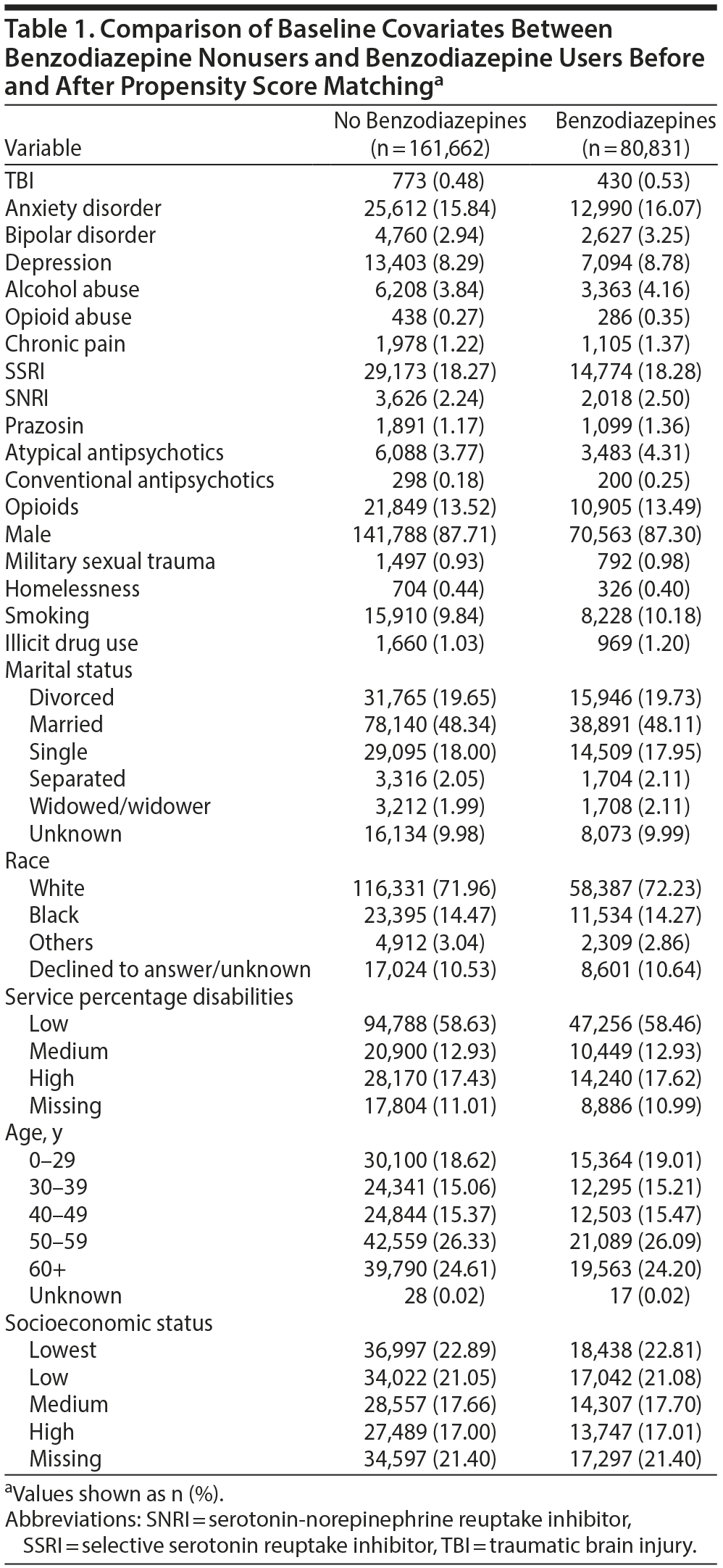
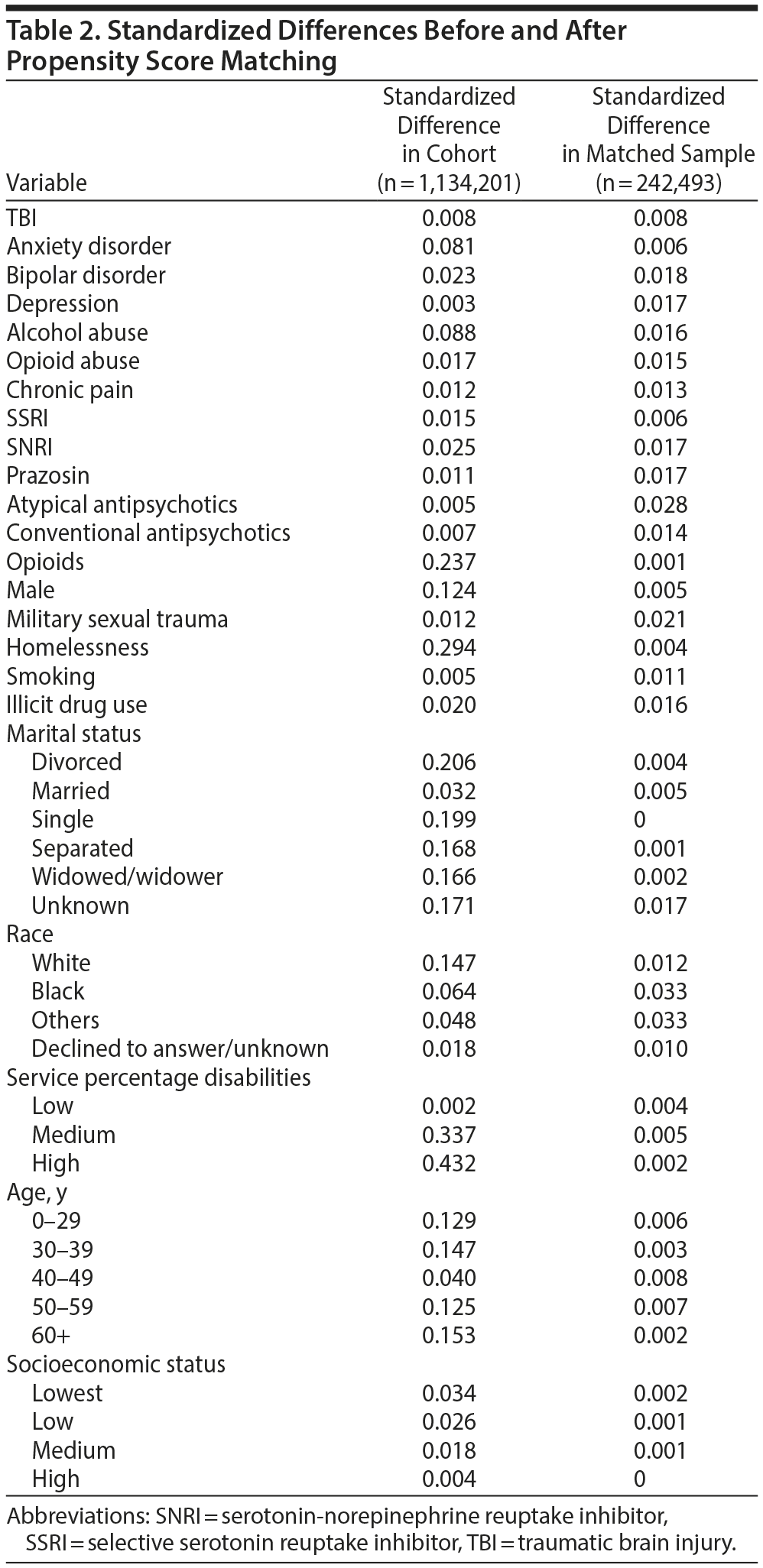
Before propensity score matching, there were 80,832 benzodiazepine users and 1,053,369 benzodiazepine nonusers with PTSD (a total of 1,134,201 veterans). After 1:2 matching, 891,708 patients were excluded (1 benzodiazepine user and 891,707 benzodiazepine nonusers); the final propensity-matched cohort consisted of 242,493 veterans with PTSD, of whom there were 80,831 benzodiazepine users and 161,662 benzodiazepine nonusers (Figure 1). After propensity score matching, there were no large or clinically meaningful differences in baseline covariates (Table 1). All standardized differences in the matched cohort were close to zero, which indicated covariate balance between benzodiazepine users and nonusers (Table 2).
Health Care Utilization
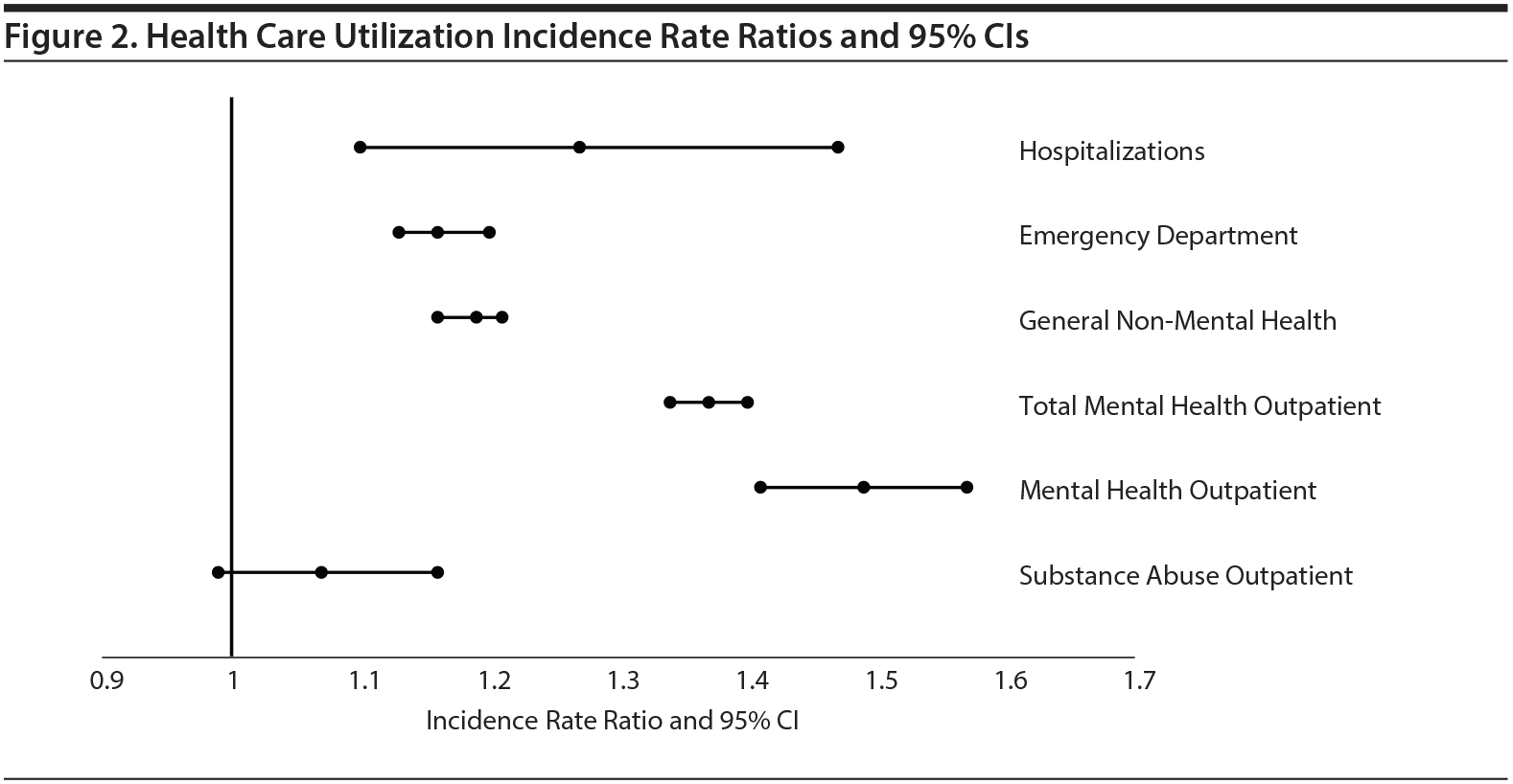
Rates of health care utilization were higher among benzodiazepine users than nonusers, with the exception of substance abuse outpatient visits (Figure 2). On average, over the 6-year follow-up period, patients with benzodiazepines had 27% more hospitalizations (adjusted IRR 95% CI, 1.10-1.47), 16% more emergency department visits (adjusted IRR 95% CI, 1.13-1.20), 19% more general non-mental health outpatient visits (adjusted IRR 95% CI, 1.16-1.21), 49% more mental health outpatient visits (adjusted IRR 95% CI, 1.41-1.57), and 37% more total mental health outpatient visits (adjusted IRR 95% CI, 1.34-1.40) relative to patients without benzodiazepines. Finally, patients with benzodiazepines had 7% more substance abuse outpatient visits, although this was found to be statistically insignificant (adjusted IRR 95% CI, 0.99-1.16).
Suicide Death
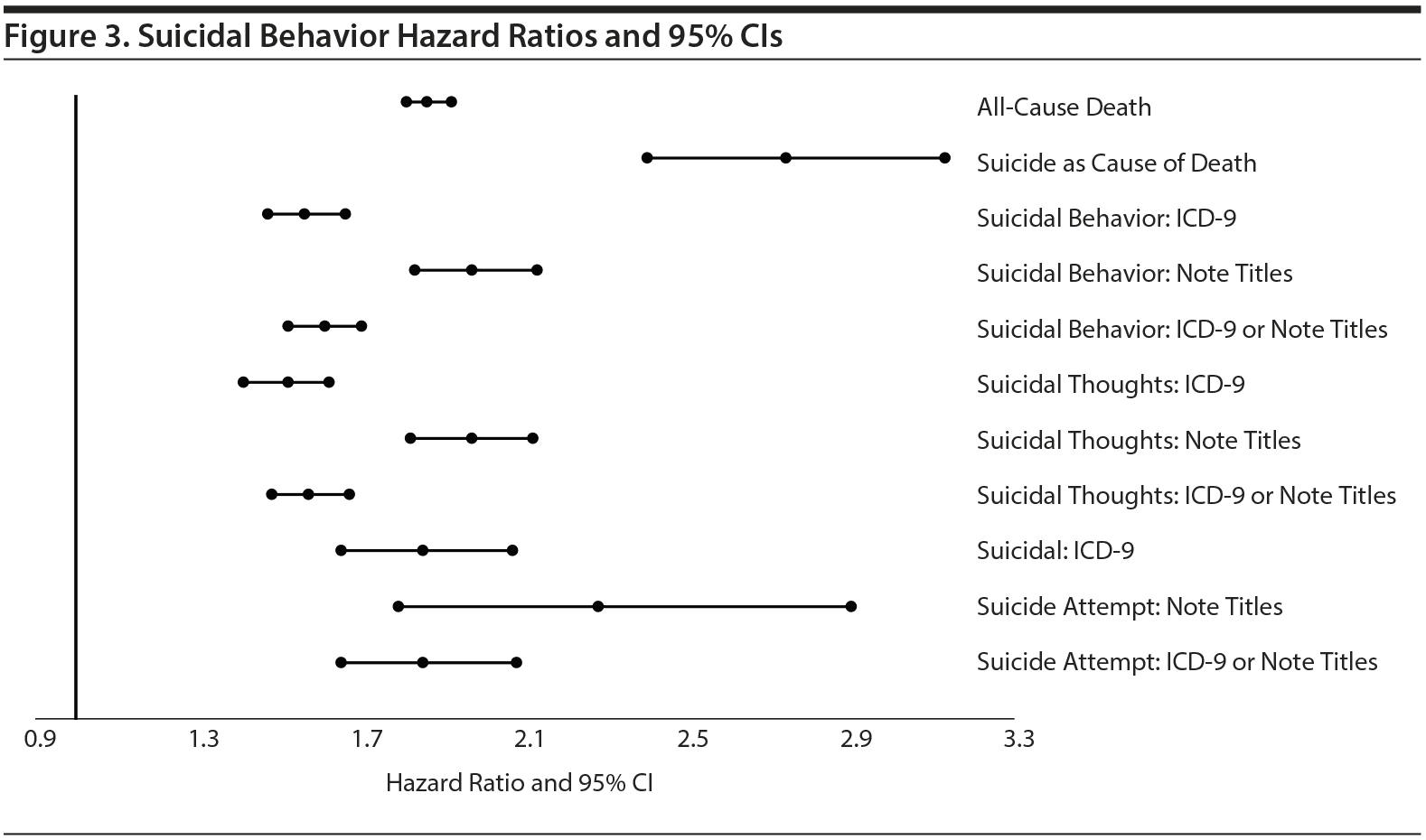
Using data from the SDR, 26,841 (11.06%) of 242,493 patients in the propensity-matched cohort died during the study period. Patients who received benzodiazepines were 1.86 times more likely to die of any cause than patients who did not (adjusted HR 95% CI, 1.81-1.92; Figure 3). The number of veterans who completed suicide was 456 (3.68%) of 12,391 benzodiazepine users and 349 (2.41%) of 14,481 benzodiazepine nonusers. As compared to the nonuser group, patients who received benzodiazepines were 2.74 times more likely to die by suicide (adjusted HR 95% CI, 2.40-3.13; Figure 3). The NNH for all-cause mortality, 15.6, means that for approximately every 16 patients with PTSD who receive benzodiazepines, 1 will die. The NNH for suicide death, 333.3, means that for approximately every 333 patients with PTSD who receive benzodiazepines, 1 will complete suicide. Thus, in this cohort, the number of preventable veteran suicides is approximately 243.
Sensitivity Analyses
Patterns of association were similar regardless of the outcome assessment method. Using ICD-9 codes, benzodiazepine users were 1.56 times more likely than benzodiazepine nonusers to exhibit suicidal behavior (adjusted HR 95% CI, 1.47-1.66), 1.52 times more likely to have suicidal thoughts (adjusted HR 95% CI, 1.41-1.62), and 1.85 times more likely to attempt suicide (adjusted HR 95% CI, 1.64-2.07). Using EMR note titles, veterans who received benzodiazepines were 1.97 times more likely to exhibit suicidal behavior (adjusted HR 95% CI, 1.83-2.13), 1.97 times more likely to have suicidal thoughts (adjusted HR 95% CI, 1.82-2.12), and 2.28 times more likely to attempt suicide (adjusted HR 95% CI, 1.79-2.90). Finally, using a combined outcome (ICD-9 codes or EMR note titles), veterans who received benzodiazepines were 1.61 times more likely to exhibit suicidal behavior (adjusted HR 95% CI, 1.52-1.70), 1.57 times more likely to have suicidal thoughts (adjusted HR 95% CI, 1.48-1.67), and 1.85 times more likely to attempt suicide (adjusted HR 95% CI, 1.65-2.08).
DISCUSSION
Veterans diagnosed with PTSD who received a benzodiazepine prescription had significantly more hospitalizations, emergency department visits, general non-mental health outpatient visits, mental health outpatient visits, and total mental health outpatient visits. Benzodiazepine users were also more likely than the comparator group to have medically documented suicidal thoughts and behaviors, as indicated by ICD-9 codes and electronic record note titles. Benzodiazepine users were 1.9 times likely to die of any cause. Most importantly, benzodiazepine users were 2.7 times more likely to die by suicide than patients who did not receive benzodiazepines.
In June 2017, the VA released updated Clinical Practice Guidelines for the treatment of PTSD. The new guidelines indicate similar first-line recommended treatments for PTSD and an expanded list of second-line agents following failure of all first-line medication options.27 Benzodiazepines and atypical antipsychotics remain on the list of drugs that should not be used.27 Our study supports these recommendations and provides further evidence for the potential harms in using benzodiazepines in patients with PTSD.
To our knowledge, this study is the first to evaluate the relationship between benzodiazepine use with suicide risk and health care utilization among veterans diagnosed with PTSD. While benzodiazepines can provide some treatment-resistant patients with short-term symptomatic relief, their use is associated with worse overall PTSD symptom severity, and depression, all of which potentially increase risk for suicidal behavior.5-8 Veterans suffering from PTSD have increased health care utilization and are 3 times as likely to experience suicidal behavior compared to veterans without PTSD.5-8 However, prior to this study, little was known about the relationship between benzodiazepines and the outcomes of health care utilization and completed suicide. An association of benzodiazepines with health care utilization and suicide is consistent with existing biological and medical knowledge. Potential biological explanations for benzodiazepines’ worsening long-term outcomes include discontinuation symptoms that stem from decreased inhibition from the γ-aminobutyric acid system and hyperactive excitation from glutamate, disruption of normal stress responses, avoidance of cognitive and emotional processing of trauma, and worsening of underlying PTSD pathophysiology.10
Our study has several important strengths. The population consisted of a large number of veterans who were diagnosed with PTSD and exposed to benzodiazepines, which ensures adequate power. The VA treats the largest population of PTSD sufferers in the United States. Since the VA is a nationwide, integrated health system, we were able to follow patients across inpatient and outpatient settings of care, allowing for more complete follow-up. Robust data collected by the SDR and the use of multiple definitions of suicidal behavior allowed us to assess the risk of these outcomes with relative confidence. While comparability between exposed and nonexposed is difficult to achieve in a retrospective cohort, the existence of observable systematic differences between the 2 treatment groups was eliminated through propensity scores. In addition, this method preserved the exposed group, separated the analysis phase from the design phase, and reduced the likelihood of bias from iterative model building.
This study also has some notable limitations. An important limitation of propensity score matching is that it accounts for measured confounders only, and only to the extent that they are accurately measured. If a potential confounder is not measured or available, adjustments cannot be made. As a result, some unmeasured confounding may be present in this study. However, a great many proximal risk factors were used based on an exhaustive search of the literature and were included in the propensity score model. Of note, PTSD symptom severity was not adjusted for in the propensity score model. There were 2 reasons for this: First, there is no structured data field in the VHA that captures symptom severity; scales such as the Posttraumatic Diagnostic Scale that measure symptom severity are not consistently implemented. Second, severity was indirectly adjusted for through the inclusion of comorbidities such as bipolar disorder, anxiety disorder, and depression. The present study’s population may also limit generalizability to other cohorts of veterans, such as veterans who were diagnosed with and sought care for PTSD outside the VHA. Thus, the study results are not generalizable to all veterans with PTSD. However, veterans who did seek some care outside (and inside) the VA were included if they did meet the cohort eligibility criteria. Relatedly, patients who take benzodiazepines may have received this medication outside of the VA but not within the VA, although this limitation is very likely mitigated by the strong incentive for veterans to fill prescriptions at the VA due to the smaller copays that exist within the VHA than outside the VHA for most medications, including benzodiazepines.28 Veterans are therefore more likely to fill prescriptions within the VHA. While there could be unreliability in coding and documentation of various suicide risk indicators, the results of sensitivity analyses revealed a consistent pattern of higher rates of suicide risk indicators (ie, note titles, ICD-9 codes, and suicide death).
Despite these limitations, the present study provides critical information about the potential risks associated with benzodiazepine use among veterans diagnosed with PTSD. From a clinical perspective, these results suggest that prescribers should carefully weigh the benefits and risks of prescribing a benzodiazepine, particularly the increased risk of suicide, among veterans diagnosed with PTSD.
Submitted: November 22, 2017; accepted April 19, 2018.
Published online: October 23, 2018.
Author contributions: Dr Deka had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Drs Deka, Stevens, Bryan, LaFleur, and Oderda. Acquisition, analysis, or interpretation of data: Drs Deka, Stevens, Bryan, LaFleur, and Oderda. Drafting of the manuscript: Drs Deka, Stevens, Bryan, LaFleur, and Oderda. Critical revision of the manuscript for important intellectual content: all authors. Statistical analysis: Drs Deka and Stevens. Obtained funding: Dr Stevens. Administrative, technical, or material support: Drs Deka and Stevens. Study supervision: Dr Stevens.
Potential conflicts of interest: None.
Funding/support: This material is based on work supported in part by Center of Innovation grant 13-414 (to Dr Stevens; Principal Investigator: Matthew Samore, MD) from the US Department of Veterans Affairs, Veterans Health Administration, Office of Research and Development, Health Services Research and Development service.
Role of the sponsor: The funding source had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and the decision to submit the manuscript for publication.
Disclaimer: The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the United States government.
REFERENCES
1. Friedman MJ, Keane TM. Handbook of PTSD. 2nd ed. New York, NY: The Guilford Press; 2014.
2. Cohen BE, Gima K, Bertenthal D, et al. Mental health diagnoses and utilization of VA non-mental health medical services among returning Iraq and Afghanistan veterans. J Gen Intern Med. 2010;25(1):18-24. PubMed CrossRef
3. Kang HK, Bullman TA, Smolenski DJ, et al. Suicide risk among 1.3 million veterans who were on active duty during the Iraq and Afghanistan wars. Ann Epidemiol. 2015;25(2):96-100. PubMed CrossRef
4. The Veterans Health Administration’s Treatment of PTSD and Traumatic Brain Injury among Recent Combat Veterans. Congressional Budget Office website. https://www.cbo.gov/sites/default/files/112th-congress-2011-2012/reports/02-09-PTSD_0.pdf
5. Jakupcak M, Hoerster KD, Varra A, et al. Hopelessness and suicidal ideation in Iraq and Afghanistan War Veterans reporting subthreshold and threshold posttraumatic stress disorder. J Nerv Ment Dis. 2011;199(4):272-275. PubMed CrossRef
6. Suicide Among Veterans and Other Americans. US Department of Veterans Affairs website. https://www.mentalhealth.va.gov/docs/2016suicidedatareport.pdf
7. Calhoun PS, Bosworth HB, Grambow SC, et al. Medical service utilization by veterans seeking help for posttraumatic stress disorder. Am J Psychiatry. 2002;159(12):2081-2086. PubMed CrossRef
8. Kartha A, Brower V, Saitz R, et al. The impact of trauma exposure and post-traumatic stress disorder on healthcare utilization among primary care patients. Med Care. 2008;46(4):388-393. PubMed
9. Jeffreys M, Capehart B, Friedman MJ. Pharmacotherapy for Post-Traumatic Stress Disorder: Review with Clinical Applications. Washington, DC: VA Health Care; 2010.
10. Guina J, Rossetter SR, DeRhodes BJ, et al. Benzodiazepines for PTSD: a systematic review and meta-analysis. J Psychiatr Pract. 2015;21(4):281-303. PubMed CrossRef
11. Amos T, Stein DJ, Ipser JC. Pharmacological interventions for preventing post-traumatic stress disorder (PTSD). Cochrane Database Syst Rev. 2014;(7):CD006239. PubMed
12. Hermos JA, Young MM, Lawler EV, et al. Characterizations of long-term anxiolytic benzodiazepine prescriptions in veteran patients. J Clin Psychopharmacol. 2005;25(6):600-604. PubMed
13. Hermos JA, Young MM, Lawler EV, et al. Long-term, high-dose benzodiazepine prescriptions in veteran patients with PTSD: influence of preexisting alcoholism and drug-abuse diagnoses. J Trauma Stress. 2007;20(5):909-914. PubMed CrossRef
14. Institute of Medicine. Returning Home from Iraq and Afghanistan: Assessment of Readjustment Needs of Veterans, Service Members, and their Families. Washington, DC: The National Academies Press; 2013.
15. Ader R. Psychoneuroimmunology. Burlington, MA: Elsevier Academic Press; 2006.
16. Gravely AA, Cutting A, Nugent S, et al. Validity of PTSD diagnoses in VA administrative data: comparison of VA administrative PTSD diagnoses to self-reported PTSD Checklist scores. J Rehabil Res Dev. 2011;48(1):21-30. PubMed CrossRef
17. Duvall S. What is VINCI? US Department of Veterans Affairs website. https://www.hsrd.research.va.gov/for_researchers/cyber_seminars/archives/video_archive.cfm?SessionID=1143
18. Noel PH. Using VA Corporate Data Warehouse for Health Services Research. VA Information Resource Center; 2012.
19. Bossarte R, Schneiderman A. An Overview of VA/DoD Joint Military Data Repository and Data From Studies Conducted by the Epidemiology Program in the VA’s Office of Public Health. US Department of Veterans Affairs website https://www.hsrd.research.va.gov/for_researchers/cyber_seminars/archives/video_archive.cfm?SessionID=931
20. Kurth T, Walker AM, Glynn RJ, et al. Results of multivariable logistic regression, propensity matching, propensity adjustment, and propensity-based weighting under conditions of nonuniform effect. Am J Epidemiol. 2006;163(3):262-270. PubMed CrossRef
21. Garrido MM, Kelley AS, Paris J, et al. Methods for constructing and assessing propensity scores. Health Serv Res. 2014;49(5):1701-1720. PubMed CrossRef
22. Faries D, Leon AC, Haro JM, et al. Analysis of Observational Health Care Data Using SAS. Cary, NC: SAS Institute Inc.; 2010.
23. Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70(1):41-55. CrossRef
24. Coogan PF, Castro-Webb N, Yu J, et al. Neighborhood and individual socioeconomic status and asthma incidence in African American women. Ethn Dis. 2016;26(1):113-122. PubMed CrossRef
25. Rothman KJ, Greeland S, Lash TL. Modern Epidemiology. Philadelphia, PA: Lippincott Williams & Wilkins; 2012.
26. Fox J. Applied Regression Analysis and Generalized Linear Models. Thousand Oaks, CA: SAGE Publications, Inc; 2015.
27. VA/DOD Clinical Practice Guideline for the Management of Posttraumatic Stress Disorder and Acute Stress Disorder. US Department of Veterans Affairs website. https://www.healthquality.va.gov/guidelines/MH/ptsd/cpg_PTSD-full-201011612.PDF. June 2017.
28. Medication Copayments. US Department of Veterans Affairs website. https://www.va.gov/healthbenefits/resources/publications/IB10-971_medication_copayment_brochure.pdf. Revised August 2016.
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Suicide section. Please contact Philippe Courtet, MD, PhD, at [email protected].
Enjoy free PDF downloads as part of your membership!
Save
Cite
Advertisement
GAM ID: sidebar-top