J Clin Psychiatry 2022;83(5):22ac14590
To cite: Singh B, Sundaresh V. Thyroid hormone use in mood disorders: revisiting the evidence. J Clin Psychiatry. 2022;83(5):22ac14590.
To share: https://doi.org/10.4088/JCP.22ac14590
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Psychology, Mayo Clinic, Rochester, Minnesota
bDivision of Endocrinology, University of Utah School of Medicine, Salt Lake City, Utah
*Corresponding author: Balwinder Singh, MD, MS, Department of Psychiatry and Psychology, Mayo Clinic, 200 First St SW, Rochester, MN 55905 ([email protected]).
Alterations in thyroid functioning have been of long-standing interest in the research and treatment of depressive disorders. Thyroid hormones may play a role in mood regulation by modulating serotonin and norepinephrine neurotransmission. As such, thyroid hormone therapy (THT) has been investigated as a treatment option for depression and has been used clinically to treat mood disorders in patients with and without hypothyroidism.1–3 What follows is an overview of the available literature discussing the potential benefits and harms of THT in the management of unipolar and bipolar depression.
Major Depressive Disorder
Several randomized controlled trials (RCTs) and non-randomized studies report positive findings for the use of triiodothyronine (T3) in the acceleration of antidepressant response in major depressive disorder (MDD).2,4 The data reporting T3 use as an accelerating agent with a tricyclic antidepressant (TCA) are more favorable in older studies than in newer studies when THT is added to a selective serotonin reuptake inhibitor (SSRI) (and there are no published serotonin norepinephrine reuptake inhibitor acceleration trials), making it hard to know if this is a true drug difference or an artifact of older versus newer study designs or their populations. A meta-analysis of 4 RCTs (n = 444) comparing T3 and SSRI coinitiation therapy with SSRI monotherapy for MDD showed no added benefits of combining T3 with an SSRI in either response or remission rates.5
Thyroid hormone augmentation is widely used as a treatment option in MDD when first-line treatment approaches have been unsuccessful.6–8 A meta-analysis of controlled clinical trials suggested a positive effect of T3 addition to TCA in partial responders.3 However, the authors concluded a need for replication of these findings in large RCTs. Sequenced Treatment Alternatives to Relieve Depression (STAR*D), a large study that examined several different antidepressant switching and antidepressant augmentation strategies, evaluated the augmentation of antidepressant action by addition of T3. Subjects with MDD in whom other treatment strategies had already failed were randomly assigned to receive augmentation with either T3 or lithium. Each study arm showed only modest improvement, and there was no statistical difference in outcomes between the two augmentation strategies.9 A few studies have used levothyroxine (L-T4) as an augmentation agent as well, with some encouraging results.10,11 In a recent network meta-analysis of 65 studies evaluating the efficacy of 19 augmentation agents in patients with failure of at least one antidepressant, thyroid hormones (both T3 and L-T4) were effective augmentation agents.12 Supraphysiologic doses of up to 500 µg/d (with the goal to achieve suppression of thyroidstimulating
hormone [TSH] and to increase free T4 [fT4] levels by ≥ 50% compared with the pretreatment level) of L-T4 have been used in highly treatment-refractory patients and were overall well tolerated.13
Thyroid hormone therapy is often used among depressed patients with subclinical hypothyroidism (SCH) and high-normal TSH levels.7 There is debate about what TSH cutoff level should constitute euthyroid status with respect to predicting depression outcomes and whether high-normal TSH levels signal a role for considering optimization of thyroid function. Some authors note that monoaminergic antidepressants may be less effective when TSH levels are higher than 2.5 mIU/L.7,14 However, the use of THT for SCH remains controversial, and elements to consider include level of TSH, presence of thyroid antibodies, and comorbid medical conditions.15 An ancillary study of a large RCT investigated the efficacy of L-T4 on the development of depressive symptoms at 12 months in older adults (age ≥ 65 years, n = 427) with SCH.16 This study showed no significant difference in the depression scores (measured using Geriatric Depression Scale at 12 months) between the L-T4 (n = 211) and placebo (n = 216) groups.16 This study was limited by the fact that most patients had low depression scores at baseline, and the effect of L-T4 among severely depressed patients is to be considered still an area of active investigation.
Bipolar Disorder
Adjunctive THT has been studied in RCTs for bipolar depression, but it is a lower-tiered recommendation in most practice guidelines, such as the 2018 Canadian Network for Mood and Anxiety Treatments (CANMAT) guidelines.17 Overall, the evidence base for THT use in bipolar depression is sparse and based on small sample size studies with significant heterogeneity.18
A prospective study of 30 patients reported a possible intrinsic association with rapid cycling and grade I hypothyroidism (defined as decreased serum T4 level) and suggested that hypothyroidism is a risk factor for rapid cycling.19 This finding was not unequivocally replicated.20,21 A large multicenter study reported high prevalence of thyroid autoimmunity in patients with bipolar disorder, which was associated with thyroid failure but not with rapid cycling or lithium exposure.22
A recently published double-blind, placebo (n = 9) controlled RCT compared L-T4 (n = 13) and T3 (n = 10) as adjunctive treatments in rapid-cycling bipolar disorder.23 L-T4 reduced the time spent in depressed or mixed states and increased the time spent in euthymia.23 However, T3 was not superior compared to placebo. A pilot study showed some evidence of supraphysiologic L-T4 doses (400 µg/d), leading to hyperthyroxinemic states, alleviating mood symptoms (depression and mania) in patients with rapid-cycling bipolar disorder.24 Nonetheless, some patients relapsed despite being on supraphysiologic doses. One explanation provided by the authors was that “supranormal circulating levels of free thyroxine were necessary to induce clinical response.” Another RCT investigating the efficacy of supraphysiologic L-T4 (300 µg/d) as an adjunctive treatment in patients with bipolar depression did not find an overall effect versus placebo at study end, except in a post hoc analysis that identified female sex as a possible moderator of response.25 Use of supraphysiologic L-T4 dose is uncommon in clinical settings but worth investigating further, especially due to limited options for treatment-refractory bipolar disorder.
Clinical Practice
Effective communication with a patient’s primary care physician (PCP) is important for the prevention and timely diagnosis of short- and long-term complications of THT. This is especially important when THT is started in euthyroid patients or if one is considering a high/supraphysiologic dose of L-T4. All patients diagnosed with mood disorders should undergo a baseline thyroid hormone evaluation measuring serum TSH. If the TSH level is low, patients should be further evaluated by their PCP and/or endocrinologist, as it is contraindicated to initiate THT in hyperthyroid patients. If TSH is high, fT4 and thyroid peroxidase antibody levels are indicated to evaluate the extent and etiology of hypothyroidism, respectively. While TSH levels above 20 mIU/L indicate hypothyroidism, TSH elevations less than 20 mIU/L may be due to hypothyroidism or recovery from euthyroid sick syndrome (ESS). Since it takes several weeks for the TSH to normalize in ESS, it is best to discuss with the PCP and/or endocrinologist before initiating THT.
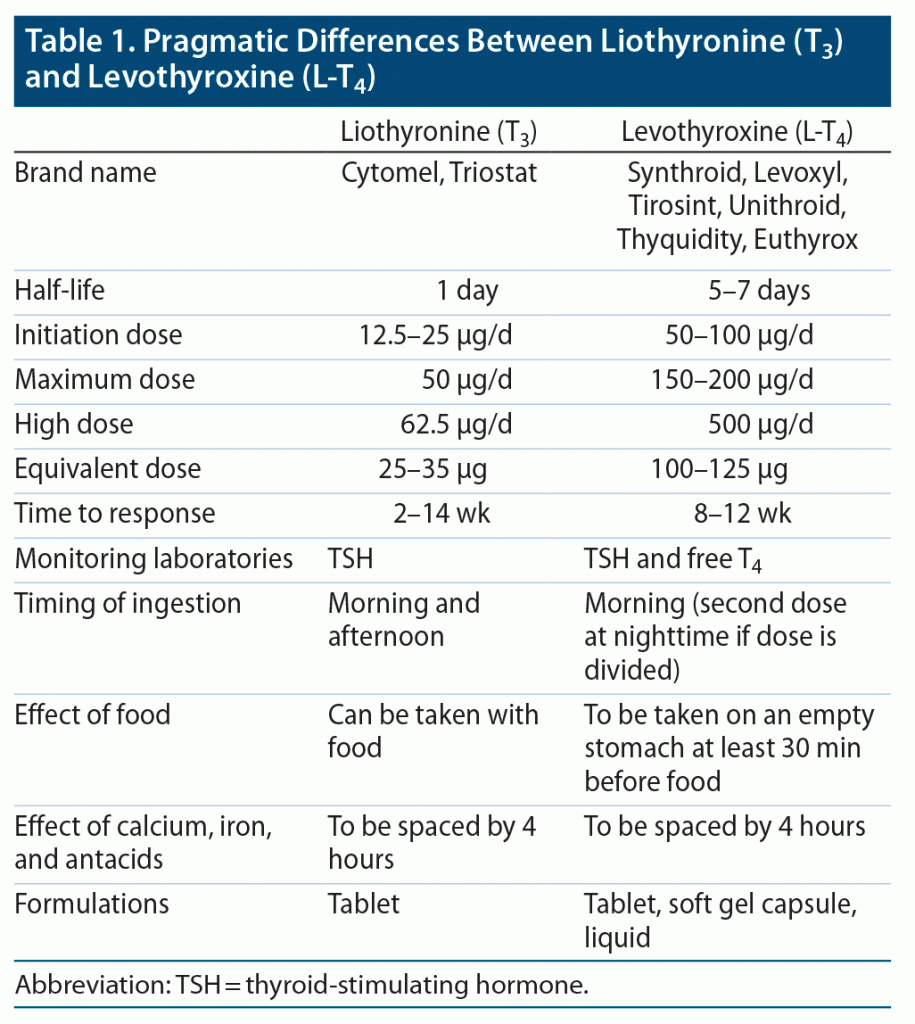
Although both T3 and L-T4 can be used to augment antidepressant treatment, T3 (the active hormone) has been favored by clinicians based on the older literature.10 Short- and long-term adverse effects of L-T4 are the same as for T3. Table 1 describes some pragmatic differences between T3 and L-T4. The benefit and possible adverse effects of THT should be discussed with patients. Those with known or suspected cardiac conditions should be evaluated and cleared by their PCP prior to initiating THT. Since THT increases the metabolic rate, it is not safe to be used in patients with compromised cardiovascular function (eg, cardiac arrhythmias, recent myocardial infarction, unstable angina) and untreated adrenal insufficiency. Caution should be exercised in patients who are 65 years and older because they are more susceptible to adverse cardiac events. While studies evaluating short-term use of T3 at 25–50 µg/d report good tolerability for most patients, hyperthyroid symptoms may still occur (palpitations, dyspnea, diaphoresis, hand tremors, anxiety, insomnia, unintentional weight loss, and hyperdefecation). Hence, patients should be advised to immediately hold the THT in case they experience any of these symptoms and report this to their prescribing physician. In patients who have been on long-term THT therapy, accelerated bone loss resulting in osteoporosis and fragility fractures is a concern, especially in postmenopausal women. Hence, appropriate communication with the PCP to manage bone health with (a) adequate calcium and vitamin D intake, (b) regular weight-bearing and balance exercises, (c) fall prevention efforts, and (d) a monitoring plan using a bone density scan is prudent.
The standard practice is to start T3 at 12.5–25 µg/d, and, based on tolerability and response over 1–2 weeks, the dose can be titrated to a maximum of 50 µg/d.26 In patients 65 years and older, T3 is started at a lower dose. When successful, augmentation with T3 can lead to remission anywhere between 2–14 weeks.9 The maximum tolerated dose of T3 should be used for 4–6 weeks before a decision is made regarding its efficacy. While minimal data are available to guide physicians regarding long-term use of T3, duration of therapy likely varies from patient to patient depending on magnitude of clinical response and adverse effects. Some authors advise tapering off T3 after 60 days, by 12.5 µg every 3 days; T3 can be reinitiated if there is a relapse of depression symptoms.27 Some open-label studies have reported safety data on long-term (≥ 1 year) maintenance treatment with THT.13,28,29 In such scenarios, TSH can be measured every 3–6 months or as needed to monitor thyroid status. If TSH is below the lower limit of reference range, the dose of T3 should be reduced and TSH rechecked after 7–10 days, as T3 has a shorter half-life (1 day) compared to L-T4 (half-life of 5–7 days), for which TSH should be rechecked after 5–6 weeks.
L-T4 is often started at 50 µg/d and is optimized to 100–150 µg/d. High L-T4 doses such as 400–500 µg/d, although reported in the literature,6,24 are rarely used in clinical settings due to concerns regarding short- and long-term adverse events and limited evidence base.
Conclusion
Thyroid functioning can play a pivotal role in mood disorders, with even minor perturbations leading to unstable mood states. Careful use of T3 and L-T4 can be critical mood-stabilizing options, especially for depressive illness that has not responded to first-line therapies, and can provide an alternative to other augmentation strategies such as atypical antipsychotics, lithium, or esketamine/ketamine.
Published online: August 15, 2022.
Relevant financial relationships: Dr Singh reports no potential conflicts of interest. Dr Sundaresh is the recipient of a patient education research grant from Radius Health Inc., unrelated to this manuscript.
Funding/support: None.
ORCID: Balwinder Singh: https://orcid.org/000-0001-7062-8192
The ASCP Corner, edited by Leslie L. Citrome, MD, MPH, is a collection of brief peer-reviewed, evidence-based articles, authored by American Society of Clinical Psychopharmacology members, that examine the practice of psychopharmacology through the lens of clinical experience. The information contained herein only represents the opinion of the author(s).

References (29)

- Feldmesser-Reiss EE. The application of triiodothyronine in the treatment of mental disorders. J Nerv Ment Dis. 1958;127(6):540–545. PubMed CrossRef
- Prange AJ Jr, Wilson IC, Rabon AM, et al. Enhancement of imipramine antidepressant activity by thyroid hormone. Am J Psychiatry. 1969;126(4):457–469. PubMed CrossRef
- Aronson R, Offman HJ, Joffe RT, et al. Triiodothyronine augmentation in the treatment of refractory depression: a meta-analysis. Arch Gen Psychiatry. 1996;53(9):842–848. PubMed CrossRef
- Altshuler LL, Bauer M, Frye MA, et al. Does thyroid supplementation accelerate tricyclic antidepressant response? a review and meta-analysis of the literature. Am J Psychiatry. 2001;158(10):1617–1622. PubMed CrossRef
- Papakostas GI, Cooper-Kazaz R, Appelhof BC, et al. Simultaneous initiation (coinitiation) of pharmacotherapy with triiodothyronine and a selective serotonin reuptake inhibitor for major depressive disorder: a quantitative synthesis of double-blind studies. Int Clin Psychopharmacol. 2009;24(1):19–25. PubMed CrossRef
- Bauer M, Hellweg R, Gräf KJ, et al. Treatment of refractory depression with high-dose thyroxine. Neuropsychopharmacology. 1998;18(6):444–455. PubMed CrossRef
- Cohen BM, Sommer BR, Vuckovic A. Antidepressant-resistant depression in patients with comorbid subclinical hypothyroidism or high-normal TSH levels. Am J Psychiatry. 2018;175(7):598–604. PubMed CrossRef
- Rosenthal LJ, Goldner WS, O’Reardon JP. T3 augmentation in major depressive disorder: safety considerations. Am J Psychiatry. 2011;168(10):1035–1040. PubMed CrossRef
- Nierenberg AA, Fava M, Trivedi MH, et al. A comparison of lithium and T(3) augmentation following two failed medication treatments for depression: a STAR*D report. Am J Psychiatry. 2006;163(9):1519–1530. PubMed CrossRef
- Joffe RT, Singer W. A comparison of triiodothyronine and thyroxine in the potentiation of tricyclic antidepressants. Psychiatry Res. 1990;32(3):241–251. PubMed CrossRef
- Spoov J, Lahdelma L. Should thyroid augmentation precede lithium augmentation: a pilot study. J Affect Disord. 1998;49(3):235–239. PubMed CrossRef
- Nuñez NA, Joseph B, Pahwa M, et al. Augmentation strategies for treatment resistant major depression: a systematic review and network meta-analysis. J Affect Disord. 2022;302:385–400. PubMed CrossRef
- Bauer M, Berghöfer A, Bschor T, et al. Supraphysiological doses of L-thyroxine in the maintenance treatment of prophylaxis-resistant affective disorders. Neuropsychopharmacology. 2002;27(4):620–628. PubMed CrossRef
- Talaei A, Rafee N, Rafei F, et al. TSH cut off point based on depression in hypothyroid patients. BMC Psychiatry. 2017;17(1):327. PubMed CrossRef
- Biondi B, Cappola AR, Cooper DS. Subclinical hypothyroidism: a review. JAMA. 2019;322(2):153–160. PubMed CrossRef
- Wildisen L, Feller M, Del Giovane C, et al. Effect of levothyroxine therapy on the development of depressive symptoms in older adults with subclinical hypothyroidism: an ancillary study of a randomized clinical trial. JAMA Netw Open. 2021;4(2):e2036645. PubMed CrossRef
- Yatham LN, Kennedy SH, Parikh SV, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) 2018 guidelines for the management of patients with bipolar disorder. Bipolar Disord. 2018;20(2):97–170. PubMed CrossRef
- Parmentier T, Sienaert P. The use of triiodothyronine (T3) in the treatment of bipolar depression: a review of the literature. J Affect Disord. 2018;229:410–414. PubMed CrossRef
- Bauer MS, Whybrow PC, Winokur A. Rapid cycling bipolar affective disorder, I: association with grade I hypothyroidism. Arch Gen Psychiatry. 1990;47(5):427–432. PubMed CrossRef
- Post RM, Kramlinger KG, Joffe RT, et al. Rapid cycling bipolar affective disorder: lack of relation to hypothyroidism. Psychiatry Res. 1997;72(1):1–7. PubMed CrossRef
- Joffe RT, Kutcher S, MacDonald C. Thyroid function and bipolar affective disorder. Psychiatry Res. 1988;25(2):117–121. PubMed CrossRef
- Kupka RW, Nolen WA, Post RM, et al. High rate of autoimmune thyroiditis in bipolar disorder: lack of association with lithium exposure. Biol Psychiatry. 2002;51(4):305–311. PubMed CrossRef
- Walshaw PD, Gyulai L, Bauer M, et al. Adjunctive thyroid hormone treatment in rapid cycling bipolar disorder: a double-blind placebo-controlled trial of levothyroxine (L-T4) and triiodothyronine (T3). Bipolar Disord. 2018;20(7):594–603. PubMed CrossRef
- Bauer MS, Whybrow PC. Rapid cycling bipolar affective disorder, II: treatment of refractory rapid cycling with high-dose levothyroxine: a preliminary study. Arch Gen Psychiatry. 1990;47(5):435–440. PubMed CrossRef
- Stamm TJ, Lewitzka U, Sauer C, et al. Supraphysiologic doses of levothyroxine as adjunctive therapy in bipolar depression: a randomized, double-blind, placebo-controlled study. J Clin Psychiatry. 2014;75(2):162–168. PubMed CrossRef
- Kennedy SH, Lam RW, McIntyre RS, et al; CANMAT Depression Work Group. Canadian Network for Mood and Anxiety Treatments (CANMAT) 2016 clinical guidelines for the management of adults with major depressive disorder: section 3. pharmacological treatments. Can J Psychiatry. 2016;61(9):540–560. PubMed CrossRef
- Schatzberg AF, DeBattista C. Augmentation strategies for treatment-resistant disorders. In: Schatzberg’s Manual of Clinical Psychopharmacology. 9th ed. American Psychiatric Association Publishing; 2019:544–546.
- Kelly TF, Lieberman DZ. Long term augmentation with T3 in refractory major depression. J Affect Disord. 2009;115(1-2):230–233. PubMed CrossRef
- Gyulai L, Bauer M, Garcia-Espana F, et al. Bone mineral density in pre-and post-menopausal women with affective disorder treated with long-term L-thyroxine augmentation. J Affect Disord. 2001;66(2-3):185–191. PubMed CrossRef
This PDF is free for all visitors!
Save
Cite