Prim Care Companion CNS Disord 2023;25(2):22cr03346
To cite: Sayles BD, Royer EG, Meyer Karre VM, et al. Malignant catatonia induced by concurrent opioid and benzodiazepine withdrawal. Prim Care Companion CNS Disord. 2023;25(2):22cr03346.
To share: https://doi.org/10.4088/PCC.22cr03346
© 2023 Physicians Postgraduate Press, Inc.
aCollege of Medicine, University of Nebraska Medical Center, Omaha, Nebraska
bDepartment of Psychiatry, University of Nebraska Medical Center, Omaha, Nebraska
*Corresponding author: Alëna A. Balasanova, MD, Department of Psychiatry, Poynter Hall 5th Floor, University of Nebraska Medical Center, 985578 Nebraska Medical Center, Omaha, NE 68198-5578 ([email protected]).
Catatonia is a psychomotor syndrome characterized by abnormal behaviors and movements, either stuporous or agitated, that is specified as malignant if hyperthermia and autonomic dysfunction are present.1,2 Previously considered a subtype of schizophrenia,3 catatonia is now recognized to arise in numerous psychiatric and physical medical conditions, including withdrawal from some sedative-hypnotic and antipsychotic medication.4,5 Malignant catatonia, formerly designated “lethal” catatonia, is a severe state of motor excitement that may progress to cardiovascular collapse and death if not treated quickly.6 We present the case of a young man who developed malignant catatonia induced by concurrent opioid and benzodiazepine withdrawal.
Case Report
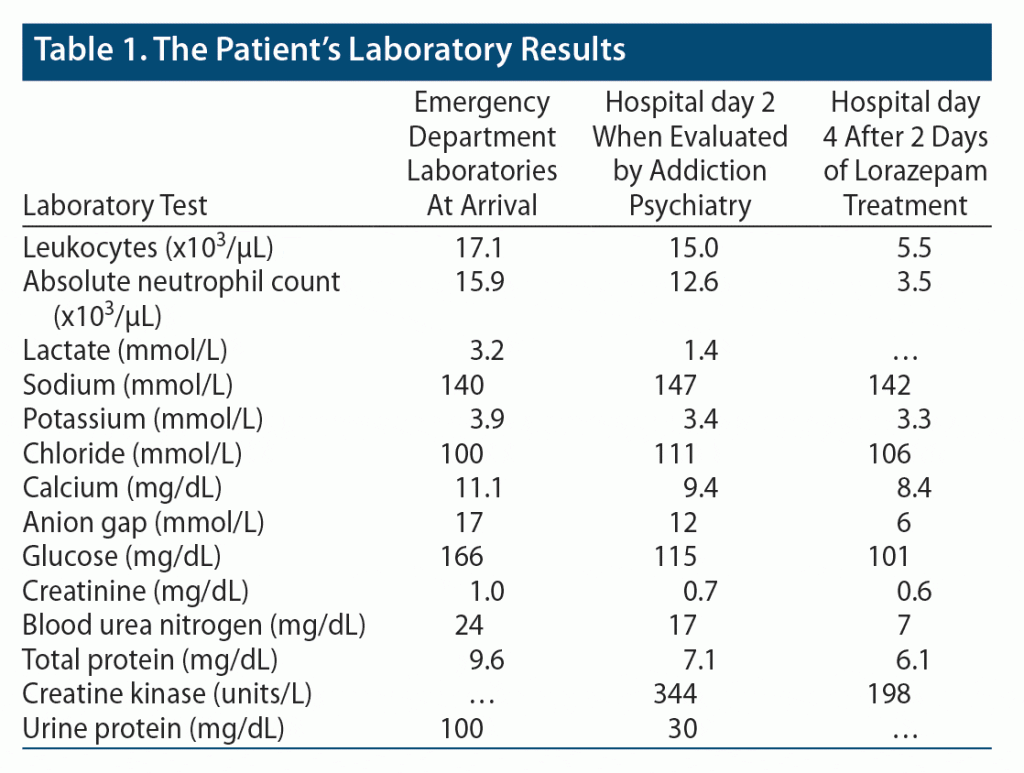
A 30-year-old man with self-reported history of unspecified anxiety, unspecified depression, and chronic pain secondary to Legg-Calves-Perthes disease on chronic opioid therapy was brought to the hospital due to decreased verbal responsiveness and recurrent emesis. He had reported an unspecified medication problem to his family 3 days earlier, which was later clarified to be an abrupt discontinuation of his anxiolytic and analgesic medications. Family reported that in the 3 days preceding admission, he became increasingly withdrawn and uncommunicative. In the emergency department, he responded to questions with slow, 1-word responses and was noted to follow commands. Laboratory analysis performed in the emergency department was remarkable for leukocytosis, an elevated anion gap with elevated lactate, and proteinuria (Table 1). His medical record showed current prescriptions for alprazolam 1 mg every 4 hours as needed for anxiety, fentanyl 50 µg/hour patch every 72 hours, oxycodone 30 mg 5 times/d, and gabapentin 900 mg 3 times/d.
At admission, the patient’s home medications were initially held. His fentanyl patch was restarted in the evening on the day of admission but was discontinued several hours later at the recommendation of another consulting team. The following day, he became less verbally responsive with new episodic rigidity in his upper extremities. A routine electroencephalogram was performed and was unremarkable. In the afternoon, the addiction psychiatry team was consulted, and on evaluation the patient exhibited stupor, mutism, sustained posturing, and grimacing with eyes tightly closed. He was febrile to 102°F, hypertensive to 164/110 mm Hg, tachycardic to 126 beats/minute, and tachypneic to 38 breaths/minute with a new oxygen requirement of 5 L/minute by nasal cannula. His leukocytosis persisted with normal creatine kinase (Table 1). Due to suspected catatonia, he was given one dose of intravenous lorazepam 2 mg, after which he began speaking nonsensically with eyes closed but maintained rigid posturing. After a second dose 30 minutes later, he relaxed his posturing, opened his eyes, and became more coherent in his verbal responses.
Thereafter, intravenous lorazepam 2 mg was scheduled every 4 hours as the equivalent to his home dose of alprazolam. The addiction psychiatry team also recommended restarting his home fentanyl patch, which was applied to the patient that evening. His autonomic symptoms resolved within hours, and his white blood cell counts normalized within a day. His creatine kinase peaked at 387 units/L 1 day after initiation of lorazepam but remained within normal limits. His thought process became more logical, and his motor control progressively improved. He reached his baseline level of functioning after 4 days of treatment with lorazepam, fentanyl, and electrolyte repletion as needed. His home oxycodone and gabapentin were not restarted during the admission.
Discussion
Catatonia has varied presentations. DSM-5 criteria for catatonia include stupor, catalepsy, waxy flexibility, mutism, negativism, posturing, mannerism, stereotypy, agitation, grimacing, echolalia, and echopraxia.1 A trial of lorazepam is indicated in clinically suspected cases meeting more than 3 of the 12 DSM-5 criteria, even in the absence of classic signs like waxy flexibility and echolalia. Our patient met 4 criteria. A clinical improvement of over 50% after starting lorazepam confirms the diagnosis, as was the case with our patient. His catatonia was further specified as malignant due to the presence of hyperthermia, rigidity, and autonomic instability.2,6 Withdrawal from his abruptly discontinued home regimen of alprazolam, fentanyl, and oxycodone was thought to be the most likely etiology based on the absence of other potentially causative psychiatric conditions and the symptom timeframe after discontinuation. Further, his condition worsened when his fentanyl patch was removed and improved after lorazepam and fentanyl were restarted together.
Malignant catatonia is most often observed as a sequela of a psychiatric disorder, with schizophrenia, major depressive disorder, and unspecified psychotic disorders being the most common precipitants.2 Several case reports have documented catatonia induced by benzodiazepine withdrawal, which tends to develop in older patients (over age 60 years) on chronic, high-dose benzodiazepines that are rapidly tapered.5 Malignant catatonia has been reported in benzodiazepine withdrawal very rarely, however, with one review identifying only 2 cases, both older than age 59 years and presenting with fever and autonomic symptoms, out of 24 cases of catatonia induced by benzodiazepine withdrawal.5
This is the only case report, to our knowledge, of malignant catatonia presenting in combined benzodiazepine and opioid withdrawal in a young patient. Limited reports of improvement in catatonic symptoms with naloxone administration7,8 and of opioid-induced catatonic symptoms such as muscular rigidity and akinesia9 suggest a potential role of the endogenous opioid system in catatonic syndromes. Given the rarity of malignant catatonia in benzodiazepine withdrawal, our case illustrates that concurrent opioid withdrawal may predispose to a malignant presentation of catatonia. Our case is also unusual in that it arose in a relatively young patient and resolved with medical therapy alone, a less frequently successful treatment modality than electroconvulsive therapy in malignant catatonia.10
Conclusion
Our case illustrates that malignant catatonia can occur in simultaneous benzodiazepine and opioid withdrawal. In this case, initiating scheduled benzodiazepines and fentanyl led to complete resolution of catatonic symptoms, suggesting malignant catatonia in this setting may be particularly amenable to medical therapy.
Published online: March 16, 2023.
Relevant financial relationships: The authors report no conflicts of interest related to the subject of this report.
Funding/support: None.
Patient consent: The patient provided consent to publish the case report, and information has been de-identified to protect anonymity.
References (10)

- Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. American Psychiatric Association; 2013.
- Mann SC, Caroff SN, Campbell EC, et al. Malignant catatonia. In: Frucht SI, Fahn S, eds. Movement Disorder Emergencies: Diagnosis and Treatment. Totowa, NJ: Humana Press; 2013.
- Fink M, Shorter E, Taylor MA. Catatonia is not schizophrenia: Kraepelin’s error and the need to recognize catatonia as an independent syndrome in medical nomenclature. Schizophr Bull. 2010;36(2):314–320. PubMed CrossRef
- Edinoff AN, Kaufman SE, Hollier JW, et al. Catatonia: clinical overview of the diagnosis, treatment, and clinical challenges. Neurol Int. 2021;13(4):570–586. PubMed CrossRef
- Lander M, Bastiampillai T, Sareen J. Review of withdrawal catatonia: what does this reveal about clozapine? Transl Psychiatry. 2018;8(1):139. PubMed CrossRef
- Rasmussen SA, Mazurek MF, Rosebush PI. Catatonia: our current understanding of its diagnosis, treatment and pathophysiology. World J Psychiatry. 2016;6(4):391–398. PubMed CrossRef
- Sandyk R. Endogenous opioid system in catatonia. Psychiatry Res. 1985;15(2):159. PubMed CrossRef
- Davis GC, Buchsbaum MS, Bunney WE Jr. Opiates, opioid peptides and psychiatry. Ann N Y Acad Sci. 1981;362(1):67–75. PubMed CrossRef
- Havemann U, Kuschinsky K. Neurochemical aspects of the opioid-induced “catatonia.” Neurochem Int. 1982;4(4):199–215. PubMed CrossRef
- Hawkins JM, Archer KJ, Strakowski SM, et al. Somatic treatment of catatonia. Int J Psychiatry Med. 1995;25(4):345–369. PubMed CrossRef
Please sign in or purchase this PDF for $40.
Save
Cite