ABSTRACT
Objective: Adolescents diagnosed with brain or central nervous system tumors face elevated levels of depression and anxiety compared to the general pediatric population. The objective of this review was to explore factors associated with elevated depression and anxiety symptoms in these patients, as well as various currently recommended interventions.
Data Sources: Articles were searched in PubMed and filtered to select for the following MeSH keywords: brain neoplasm, mental health, behavioral symptom, mental disorder AND (child* OR adolescen* OR teen* OR youth OR pediatr*). Articles were limited to those published in English between 2000 and 2020.
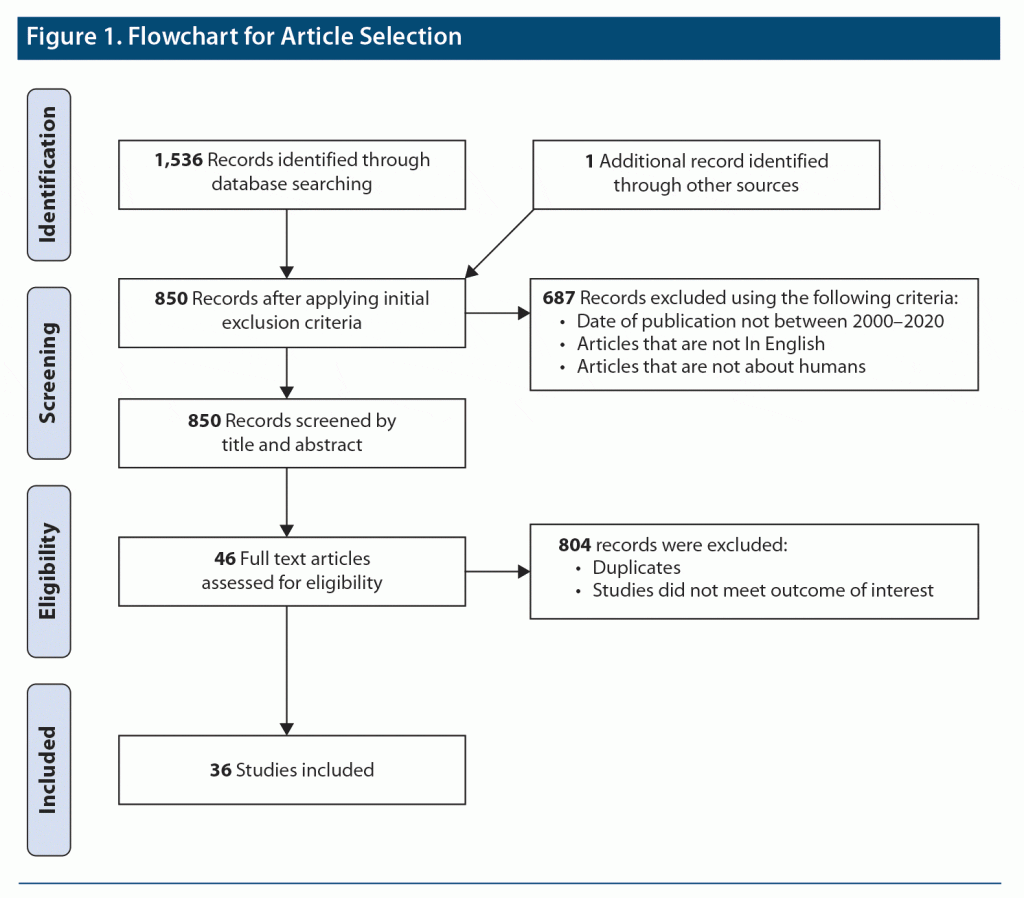
Study Selection: A total of 1,537 articles were retrieved, and 36 studies were reviewed. Articles were selected if they pertained to human subjects, specifically adolescents aged ≤ 18 years. Additionally, only articles about depression and anxiety were included. Symptoms of depression and anxiety before a brain tumor diagnosis or as symptoms of a possible brain tumor were excluded.
Data Extraction: Articles were screened by title and abstract as they pertained to depression and anxiety in patients diagnosed with brain tumors in adolescence. Data extracted included information about risk factors associated with depression and anxiety, interventions, and pharmacologic considerations.
Results: Factors associated with increased depressive and anxiety symptoms include intensity of cancer treatment, female sex, and brain tumor diagnosis. Pediatric brain tumor patients also experience elevated antidepressant prescription rates. When treating depression and anxiety in these patients, it is also important to focus on multifaceted interventions like behavioral and communication therapies, as the nature of brain tumors can affect psychological, social, and cognitive abilities.
Conclusions: Depression and anxiety can have long-lasting effects on pediatric brain tumor patients and put them at risk for developing other psychosocial problems. Therefore, it is important to recognize factors contributing to depression and anxiety as well as potential interventions.
Prim Care Companion CNS Disord 2022;24(6):21r03228
To cite: Benson J, Sarangi A. Psychiatric considerations in pediatric patients with brain tumors. Prim Care Companion CNS Disord. 2022;24(6):21r03228.
To share: https://doi.org/10.4088/PCC.21r03228
© 2022 Physicians Postgraduate Press, Inc.
aTexas Tech University Health Sciences Center School of Medicine, Lubbock, Texas
bBaylor College of Medicine, Houston, Texas
*Corresponding author: Ashish Sarangi, MD, Baylor College of Medicine, Geriatric Psychiatry, 1 Baylor Plaza, Houston, TX 77004 ([email protected]).
Brain and central nervous system (CNS) tumors are the most common solid tumors and the second most common form of cancer in the pediatric population.1 Between 2013 and 2017, the incidence rate of brain and CNS tumors in those aged ≤ 19 years in the United States was 6.14 per 100,000 persons.2 While cancer survival rates have increased among adolescents, it is important to recognize that survivors of pediatric brain tumors still experience many long-term complications. Pediatric brain tumor survivors face not only risk of neurologic/cognitive deficits, endocrine dysfunctions, and growth disturbances, but also psychological problems.3 While pediatric cancer patients in general have relatively similar rates of depression to the general pediatric population, this is not the case for those diagnosed with brain/CNS tumors. Of the long-term psychosocial effects experienced by pediatric brain tumor survivors, depression and anxiety are the most common, with incidences of 19% and 20%, respectively.4 This incidence is elevated in comparison to the general US pediatric population, for which rates of depression and anxiety are 3% and 7%, respectively.5
Many pediatric brain tumor patients appear to be more affected by social, behavioral, and emotional difficulties rather than neurocognitive or physical dysfunction. These difficulties experienced by pediatric brain tumor survivors can extend into young adult and adulthood and severely impact familial and interpersonal relationships, academic success, and mood.6 Neurocognitive or physical impairments like decreased attention span and memory issues experienced by these patients can also in turn lead to elevated levels of depression and anxiety.7,8 Given the psychological consequences of brain tumors, the objective of this clinical review is to examine depression and anxiety among pediatric brain tumor survivors and explore the management and current recommendations for treatment.
METHOD
Data were searched in PubMed using MeSH keywords for articles via the following search:
((brain neoplasm[MeSH Terms]) AND (((mental health[MeSH Terms]) OR (behavioral symptom[MeSH Terms])) OR (mental disorder[MeSH Terms]))) AND (child* OR adolescen* OR teen* OR youth OR pediatr*).
Articles were limited to publications between the years 2000 and 2020 and those pertaining to adolescents aged ≤ 18 years of age. Articles were excluded if they were not in English, not about human subjects, or had no abstract available. Articles that were not systematic, traditional reviews, meta-analyses, or clinical trials were also excluded. Articles that included diagnoses of depression or anxiety before cancer diagnoses or as symptoms of a possible brain tumor were excluded.
RESULTS
A total of 36 articles fit the selection criteria (Figure 1).
Risk Factors
Adolescence is a critical time for the development of children’s social, cognitive, and psychological health, making pediatric cancer survivors especially vulnerable to psychosocial hardships. Some studies have reported that children diagnosed with cancer do not experience more psychological difficulties in comparison to their siblings or age- and sex-matched counterparts. The overall exception, however, has been children diagnosed with brain or CNS tumors.9 While there are still a few studies that report no difference in depression outcomes between adolescent brain tumor survivors and the general healthy population,10,11 most studies do show that pediatric brain tumor survivors experience elevated levels of depression and anxiety. A study9 looking at adolescent survivors of acute lymphoblastic leukemia (ALL) or brain tumors, the 2 most common forms of childhood cancer, suggests that the psychological needs of ALL and brain tumor survivors are not being met. The 2 most significant risk factors associated with worse psychological outcomes, a brain tumor diagnosis and history of cranial radiation therapy, were found in 83% and 67% of survivors, respectively.9 In particular, diagnosis of pediatric astrocytomas or glial tumors, followed by medulloblastomas and primitive neuroectodermal tumors, were commonly associated with depression.4 However, in a single-center study12 looking at children and young adults who had been treated for astrocytoma, levels of depression and anxiety were low at an average follow-up time of 12 years later. Although the extent of tumor location impact on depression and anxiety symptoms is unclear, children diagnosed with right cortical or left cerebellar tumors have increased anxiety symptoms compared to those with tumors in other locations of the brain.13 Compared to supratentorial tumors, children with infratentorial tumors have increased depression symptoms.14 Even compared to other brain complications like traumatic brain injury and vascular/infectious brain lesions, brain tumor survivors still experience elevated levels of anxiety and depression.15
While preoperatively children with brain tumors already have increased anxiety symptoms,16 the intensity of brain tumor treatments has also been shown to associate with elevated levels of depression and anxiety. Many studies describe an increase in depression and anxiety with radiotherapy compared to chemotherapy.17 The Childhood Cancer Survivor Study18 showed that patients who received cranial radiation therapy and/or methotrexate had higher depression/anxiety scores than those who did not receive either form of treatment. Specifically, radiation to the temporal lobes has also been associated with differences in depression scores.19 Another study20 showed that patients who are categorized as receiving high-risk craniospinal irradiation treatments experience higher levels of parent-reported withdrawn/depressed behavior over time than those who receive average risk craniospinal irradiation treatments. Additionally, patients with posterior fossa syndrome have higher levels of withdrawn/depressed behavior at the time of brain tumor diagnosis but exhibit reduced levels of this behavior over time.20 When looking at patients that underwent surgery-only treatment, 35% experienced symptoms consistent with major depressive disorder, and 9% experienced anxiety symptoms. Further breakdown of these symptoms showed that 46% of patients experienced depression symptoms within 2 weeks to 1 year after treatment. As time from treatment increased (1–5 years after treatment), prevalence of depression decreased to 29%.21 Surgery can also be a source of anxiety for children with brain tumors. This anxiety does not persist after surgery, but in 1 patient, postoperative symptoms of depression were described. In this case, depression was related to fear of relapse.22
Studies have also reported an association between sex and depressive symptoms in pediatric brain tumor patients. A study by Brinkman and colleagues20 found that females were more likely to exhibit parent-reported withdrawn/depressed behaviors compared to their male counterparts. This is consistent with findings from Barrera and colleagues23 that females are at greater risk of depression than males, as decreased social skills and self-worth has also been shown to be associated with depressive symptoms. In a separate study, Barrera and colleagues24 designed an intervention program focused on social skills like establishing friendships, conflict resolution, cooperation, bullying management, building self-confidence, and empathy. While the intervention improved quality of life, self-control, and social skills, it had no significant impact on levels of depression in adolescent survivors of childhood brain tumors.24
The psychological effects of a brain tumor diagnosis in adolescence can persist into adulthood. In a report from the Childhood Cancer Survivor Study,18 levels of clinically significant psychological distress at young adulthood in pediatric brain tumor survivors were similar to those of the general population. However, after adjusting for socioeconomic status, physical health status, and sex (risk factors for psychological distress), brain tumor survivors were more likely to experience depressive symptoms than their siblings. Additionally, females and those from lower socioeconomic backgrounds were at greater risk of experiencing depression. On the contrary, Gunn et al25 found that the majority of survivors did not experience increased risk of depression but did have impaired quality of life. Elevated psychological distress was found to be associated with reduced social functioning as a result of cancer, rather than cancer treatment directly.26 Memmesheimer et al27 found that among young adults who had been diagnosed with a craniopharyngioma in adolescence, greater than 20% and 10% had elevated Hospital Anxiety and Depression Scale scores indicative of clinical depression and anxiety, respectively. This increase in depression and anxiety was not affected by the number of lifetime surgeries, but rather experience of a negative life event in the prior year. Additionally, among childhood cancer survivors, those with a history of brain tumor in particular face increased risk of hospitalization for psychiatric disease. However, there was no clear trend in risk as related to time since diagnosis or age at diagnosis.11
Depression and anxiety are often risk factors for other psychological conditions, emphasizing an even greater necessity to screen for and address symptoms of depression and anxiety. In a study28 looking at suicidal ideation in adult and adolescent survivors of childhood brain tumors, 40.8% and 27.6% experienced depression and anxiety, respectively. Furthermore, depression specifically was associated with increased risk of suicidal ideation.28 A study29 looking at cognitive fatigue in adolescent ALL and brain tumor patients found that while a brain tumor diagnosis was the main predictor of cognitive fatigue, depression was the second predictor. Depression has also been shown to correlate with self-rated apathy30 and decreased quality of life.25,31 On the contrary, depression and anxiety symptoms were not found to be predictive of reduced adaptive functioning.32
Interventions
Antidepressants are prescribed at higher rates in the pediatric oncology population than in the general pediatric population. A study by the National Institutes of Health (NIH)33 found that, on average, psychotropic medications were prescribed twice as often in pediatric oncology patients than in the general pediatric population. However, when looking at those diagnosed with brain cancer specifically, 7% of patients received medications, which was similar to the rate in the general population (6%). This similarity could be due in part to the small sample size of the study. Johannsdottir and colleagues,34 however, did find that among children and young adult cancer survivors, those diagnosed with CNS tumors had a significantly increased risk of receiving antidepressant medication. The NIH study33 also found that the most commonly prescribed medications were anticonvulsants and antidepressants, specifically sertraline, a selective serotonin reuptake inhibitor (SSRI). A study35 across 9 medical centers looked specifically at SSRI prescribing practices among pediatric oncologists, with 71% of physicians reporting prescribing SSRIs to their patients. Sertraline was most prescribed, followed by fluoxetine. Physicians often prescribed antidepressants in accordance with observance of depressive symptoms, although none indicated that symptoms met the DSM diagnostic criteria for major depressive disorder.35 The study35 also emphasized the need for resources, with 40% of physicians citing desire for improved access to psychiatrists and psychologists and 19% of physicians recommending increased mental health literature and formal training for both physicians and families. The study35 suggested that antidepressants were unnecessarily overprescribed to pediatric cancer patients and increased monitoring of patients on antidepressants is necessary. It was also suggested that for mild depressive symptoms, behavioral therapies should be utilized prior to initiating psychotropic medications, as these should be reserved for cases of severe depression.35
There have been no studies, to our knowledge, assessing the risk and efficacy of antidepressant usage in pediatric brain tumor patients specifically. This is an important area of research due to the association between depression and the brain. Brain tumors and associated treatments have potential impacts on neural circuits related to emotion, which may affect the efficacy of antidepressants. Additionally, both antidepressants and brain tumors are associated with fatigue, epilepsy, and cognitive dysfunction, yet the relationships between the 2 have not been fully studied.36 Due to the lack of research on antidepressants in this population, it may be prudent to first utilize cognitive and behavioral interventions to treat depression and anxiety before prescribing medication. On the other hand, there has been research suggesting that antidepressant medications may potentially contain anticancer mechanisms useful in fighting glioblastomas and therefore may be beneficial for patients.37
Currently the Children’s Oncology Group suggests annual psychosocial evaluations for pediatric cancer survivors. However, research suggests that for adolescent brain tumor survivors, further recommendations are necessary. Early detection of their psychological needs must be made. Long-term psychological monitoring through parent/teacher reports and formal psychological evaluations every 1 to 2 years would also be beneficial.9 Poggi et al38 suggest that due to the age-related differences in psychological disorders it is necessary to alter recommendations in accordance with the patient’s age. Children in the age range of 7–13 years in particular present with higher levels of depression and anxiety and should therefore be seen regularly. Assisting children with re-entry into the school environment and development of social skills may also help improve psychological outcomes.38
Physical activity has been shown to improve psychological outcomes in survivors of childhood cancers. However, due to the nature of brain tumors, children may often present with functional deficits including loss of motor, social, or daily skills that can limit their ability to engage in activities that can improve their psychological health. A study by Cheung and colleagues39 showed that musical training is an effective alternative intervention to reduce depressive symptoms in pediatric brain tumor survivors and may even have a long-term effect. Studies have also suggested that functional deficits may not be the sole factor associated with anxiety or depression. Ehrstedt et al40 looked at seizure activity in postoperative adolescent glioneuronal tumor patients and found that all clinically elevated levels of depression and anxiety were in patients who were seizure free, with one exception. A study by Adduci and colleagues41 also found that anxiety and depression were not associated with functional deficits but rather were associated with avoidance of communication or ineffective communication about the brain tumor diagnosis between parent and child. The study41 highlights the role of effective communication, which is characterized by truthfulness, continuity, completeness, consistency, comprehensibility, and personalization in improving psychological outcomes. When parents engage with their children using effective communication regardless of their age, children are better able to comprehend and cope with their diagnosis, thereby reducing negative psychological impact.13
Because of the relationship of depression and anxiety with many other social and emotional difficulties, multifaceted interventions are important. In a study42 looking at social adjustment and psychological distress in pediatric brain tumor patients 8 months posttreatment, baseline levels of social withdrawal predicated elevated depression and anxiety symptoms. The loss of executive functioning, which can impede emotional expression and control, was also a predictor of increased depressive symptoms. In turn, baseline levels of depression and social skills predicated social withdrawal.42 The study42 suggested that successful interventions to lower levels of depression and anxiety in pediatric brain tumor patients should focus not only on psychological domains, but also on development of social skills in these patients.
Children diagnosed with brain tumors also experience anxiety during their treatments. In Taiwan, a study43 showed that therapeutic play can reduce anxiety associated with external beam radiotherapy, a common form of brain tumor management. Children exposed to therapeutic play interventions, like painting, watching cartoons and playing video games, before external beam radiotherapy procedures had decreased salivary cortisol levels and lower fear, anxiety, and stress and Beck Youth Anxiety Inventory scores.43
Pharmacologic Considerations
Overall, antidepressants are an effective form of depression treatment in cancer patients. However, increased antidepressant use in cancer patients also warrants recognition of the potential drug interactions associated with antidepressants, as many cancer patients are often on a multidrug treatment regimen (Table 1). A study44 done at The University of Texas MD Anderson Cancer Center examined this association in cancer patients in general and found that 49% of patients were taking drugs that could have major drug interactions with antidepressants. Potential major drug interactions involved anticoagulants like heparin and serotonin syndrome–inducing drugs like tramadol and oxycodone. The presence of these drug interactions was also associated with increased risk of hospital and emergency department visits.44 Additionally, it is important to recognize the potential for drug interactions between antidepressants and chemotherapeutic drugs. The inhibition of cytochrome P450 is often linked to negative drug interactions, which is significant as many antidepressants utilize this enzyme system for metabolism. Drug interactions and potential inhibition of chemotherapeutic agents can result in reduced efficacy or even increased treatment toxicity. When prescribing antidepressants, it is of note to consider using newer antidepressants like SSRIs, which have lower drug interaction risk compared to tricyclic antidepressants (TCAs) or monoamine oxidase inhibitors.45 Specifically, imipramine and tranylcypromine (TCAs) have been shown to reduce the efficacy of temozolomide, the drug of choice for treating glioblastomas. However, fluoxetine was not shown to have this effect, demonstrating the specificity of these drug interactions to various classes of antidepressants.46 It is also important to note the potential effect of brain tumor treatments on the development of depression and anxiety symptoms. In a study47 looking at the use of trametinib in children with low-grade gliomas, 5 of 8 patients reported increased depressive symptoms, while 3 of 8 reported increased anxiety symptoms. While this was a limited case series, it highlights the need to be cognizant of possible psychiatric effects associated with treatments.47
DISCUSSION
The primary limitation of this study is exclusion of other psychiatric disorders, which may be comorbid in patients with pediatric brain tumors. These disorders can include posttraumatic stress disorder, adjustment disorder, and psychotic disorders. Discussion of these associated illnesses would be beyond the scope of this article. Classifying various tumors according to grade and stage and linking mental health issues would have added further depth to this review. Further research is needed to identify specific chemotherapeutic agents utilized in treating brain tumors and associated psychiatric side effects.
CONCLUSION
Depression and anxiety are the 2 most common psychological issues faced by survivors of pediatric brain tumors. Given the potential lasting psychological impact of a brain tumor diagnosis and vulnerability of brain tumor patients to psychological deficits, it is important to recognize ways in which depression and anxiety can be addressed in these children.
Submitted: December 23, 2021; accepted April 27, 2022.
Published online: December 20, 2022.
Relevant financial relationships: None.
Funding/support: None.
Clinical Points
- Children diagnosed with brain tumors experience increased risk of depression throughout their disease course.
- There is a lack of support and treatment of depression and anxiety in children diagnosed with brain tumors despite the high prevalence of both disorders in this population.
References (47)

- Udaka YT, Packer RJ. Pediatric brain tumors. Neurol Clin. 2018;36(3):533–556. PubMed CrossRef
- Ostrom QT, Patil N, Cioffi G, et al. CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2013–2017. Neuro-oncol. 2020;22(suppl 1):iv1–iv96. PubMed CrossRef
- Gerber NU, Zehnder D, Zuzak TJ, et al. Outcome in children with brain tumors diagnosed in the first year of life: long-term complications and quality of life. Arch Dis Child. 2008;93(7):582–589. PubMed CrossRef
- Shah SS, Dellarole A, Peterson EC, et al. Long-term psychiatric outcomes in pediatric brain tumor survivors. Childs Nerv Syst. 2015;31(5):653–663. PubMed CrossRef
- Ghandour RM, Sherman LJ, Vladutiu CJ, et al. Prevalence and treatment of depression, anxiety, and conduct problems in US children. J Pediatr. 2019;206:256–267.e3. PubMed CrossRef
- Zada G, Kintz N, Pulido M, et al. Prevalence of neurobehavioral, social, and emotional dysfunction in patients treated for childhood craniopharyngioma: a systematic literature review. PLoS One. 2013;8(11):e76562. PubMed CrossRef
- Oh Y, Seo H, Sung KW, et al. The effects of attention problems on psychosocial functioning in childhood brain tumor survivors: a 2-year postcraniospinal irradiation follow-up. J Pediatr Hematol Oncol. 2017;39(2):e46–e53. PubMed CrossRef
- Waber DP, Pomeroy SL, Chiverton AM, et al. Everyday cognitive function after craniopharyngioma in childhood. Pediatr Neurol. 2006;34(1):13–19. PubMed CrossRef
- Kahalley LS, Wilson SJ, Tyc VL, et al. Are the psychological needs of adolescent survivors of pediatric cancer adequately identified and treated? Psychooncology. 2013;22(2):447–458. PubMed CrossRef
- Alibas H, Uluc K, Kahraman Koytak P, et al. Evaluation of depressive mood and cognitive functions in patients with acromegaly under somatostatin analogue therapy. J Endocrinol Invest. 2017;40(12):1365–1372. PubMed CrossRef
- Ross L, Johansen C, Dalton SO, et al. Psychiatric hospitalizations among survivors of cancer in childhood or adolescence. N Engl J Med. 2003;349(7):650–657. PubMed CrossRef
- Kristiansen I, Strinnholm M, Strömberg B, et al. Clinical characteristics, long-term complications and health-related quality of life (HRQoL) in children and young adults treated for low-grade astrocytoma in the posterior fossa in childhood. J Neurooncol. 2019;142(1):203–210. PubMed CrossRef
- Moitra E, Armstrong CL. Neural substrates for heightened anxiety in children with brain tumors. Dev Neuropsychol. 2013;38(5):337–351. PubMed CrossRef
- Patel SK, Mullins WA, O’Neil SH, et al. Neuropsychological differences between survivors of supratentorial and infratentorial brain tumors. J Intellect Disabil Res. 2011;55(1):30–40. PubMed CrossRef
- Pastore V, Colombo K, Villa F, et al. Psychological and adjustment problems due to acquired brain lesions in pre-school-aged patients. Brain Inj. 2013;27(6):677–684. PubMed CrossRef
- Varela M, Liakopoulou M, Alexiou GA, et al. Presurgical neuropsychological and behavioral evaluation of children with posterior fossa tumors. J Neurosurg Pediatr. 2011;8(6):548–553. PubMed CrossRef
- Mabbott DJ, Spiegler BJ, Greenberg ML, et al. Serial evaluation of academic and behavioral outcome after treatment with cranial radiation in childhood. J Clin Oncol. 2005;23(10):2256–2263. PubMed CrossRef
- Schultz KAP, Ness KK, Whitton J, et al. Behavioral and social outcomes in adolescent survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. J Clin Oncol. 2007;25(24):3649–3656. PubMed CrossRef
- Brackett J, Krull KR, Scheurer ME, et al. Antioxidant enzyme polymorphisms and neuropsychological outcomes in medulloblastoma survivors: a report from the Childhood Cancer Survivor Study. Neuro-oncol. 2012;14(8):1018–1025. PubMed CrossRef
- Brinkman TM, Palmer SL, Chen S, et al. Parent-reported social outcomes after treatment for pediatric embryonal tumors: a prospective longitudinal study. J Clin Oncol. 2012;30(33):4134–4140. PubMed CrossRef
- Meyer EA, Kieran MW. Psychological adjustment of ‘surgery-only’ pediatric neuro-oncology patients: a retrospective analysis. Psychooncology. 2002;11(1):74–79. PubMed CrossRef
- Riquin E, Dinomais M, Malka J, et al. Psychiatric and psychologic impact of surgery while awake in children for resection of brain tumors. World Neurosurg. 2017;102:400–405. PubMed CrossRef
- Barrera M, Schulte F, Spiegler B. Factors influencing depressive symptoms of children treated for a brain tumor. J Psychosoc Oncol. 2008;26(1):1–16. PubMed CrossRef
- Barrera M, Schulte F. A group social skills intervention program for survivors of childhood brain tumors. J Pediatr Psychol. 2009;34(10):1108–1118. PubMed CrossRef
- Gunn ME, Mört S, Arola M, et al. Quality of life and late-effects among childhood brain tumor survivors: a mixed method analysis. Psychooncology. 2016;25(6):677–683. PubMed CrossRef
- Zebrack BJ, Gurney JG, Oeffinger K, et al. Psychological outcomes in long-term survivors of childhood brain cancer: a report from the childhood cancer survivor study. J Clin Oncol. 2004;22(6):999–1006. PubMed CrossRef
- Memmesheimer RM, Lange K, Dölle M, et al. Psychological well-being and independent living of young adults with childhood-onset craniopharyngioma. Dev Med Child Neurol. 2017;59(8):829–836. PubMed CrossRef
- Brinkman TM, Liptak CC, Delaney BL, et al. Suicide ideation in pediatric and adult survivors of childhood brain tumors. J Neurooncol. 2013;113(3):425–432. PubMed CrossRef
- Irestorm E, Tonning Olsson I, Johansson B, et al. Cognitive fatigue in relation to depressive symptoms after treatment for childhood cancer. BMC Psychol. 2020;8(1):31. PubMed CrossRef
- Mehren A, Özyurt J, Zu Klampen P, et al. Self- and informant-rated apathy in patients with childhood-onset craniopharyngioma. J Neurooncol. 2018;140(1):27–35. PubMed CrossRef
- Laffond C, Dellatolas G, Alapetite C, et al. Quality-of-life, mood and executive functioning after childhood craniopharyngioma treated with surgery and proton beam therapy. Brain Inj. 2012;26(3):270–281. PubMed CrossRef
- Papazoglou A, King TZ, Morris RD, et al. Parent report of attention problems predicts later adaptive functioning in children with brain tumors. Child Neuropsychol. 2009;15(1):40–52. PubMed CrossRef
- Pao M, Ballard ED, Rosenstein DL, et al. Psychotropic medication use in pediatric patients with cancer. Arch Pediatr Adolesc Med. 2006;160(8):818–822. PubMed CrossRef
- Johannsdottir IM, Karlstad Ø, Loge JH, et al. Prescriptions of antidepressants to survivors of cancer in childhood, adolescence, and young adulthood: a population-based study. J Adolesc Young Adult Oncol. 2017;6(1):120–126. PubMed CrossRef
- Phipps S, Buckholdt KE, Fernandez L, et al. Pediatric oncologists’ practices of prescribing selective serotonin reuptake inhibitors (SSRIs) for children and adolescents with cancer: a multi-site study. Pediatr Blood Cancer. 2012;58(2):210–215. PubMed CrossRef
- Rooney A, Grant R. Pharmacological treatment of depression in patients with a primary brain tumor. Cochrane Database Syst Rev. 2013;2013(5):CD006932. PubMed CrossRef
- Zhuo C, Xun Z, Hou W, et al. Surprising anticancer activities of psychiatric medications: old drugs offer new hope for patients with brain cancer. Front Pharmacol. 2019;10:1262. PubMed CrossRef
- Poggi G, Liscio M, Galbiati S, et al. Brain tumors in children and adolescents: cognitive and psychological disorders at different ages. Psychooncology. 2005;14(5):386–395. PubMed CrossRef
- Cheung AT, Li WHC, Ho KY, et al. Efficacy of musical training on psychological outcomes and quality of life in Chinese pediatric brain tumor survivors. Psychooncology. 2019;28(1):174–180. PubMed CrossRef
- Ehrstedt C, Rydell AM, Gabert Hallsten M, et al. Cognition, health-related quality of life, and mood in children and young adults diagnosed with a glioneuronal tumor in childhood. Epilepsy Behav. 2018;83:59–66. PubMed CrossRef
- Adduci A, Jankovic M, Strazzer S, et al. Parent-child communication and psychological adjustment in children with a brain tumor. Pediatr Blood Cancer. 2012;59(2):290–294. PubMed CrossRef
- Desjardins L, Barrera M, Schulte F, et al. Predicting social withdrawal, anxiety and depression symptoms in pediatric brain tumor survivors. J Psychosoc Oncol. 2019;37(1):22–36. PubMed CrossRef
- Tsai YL, Tsai SC, Yen SH, et al. Efficacy of therapeutic play for pediatric brain tumor patients during external beam radiotherapy. Childs Nerv Syst. 2013;29(7):1123–1129. PubMed CrossRef
- Barton MK. Drug interactions in cancer patients receiving antidepressants are common, researchers report. CA Cancer J Clin. 2011;61(5):283–284. PubMed CrossRef
- Grassi L, Nanni MG, Rodin G, et al. The use of antidepressants in oncology: a review and practical tips for oncologists. Ann Oncol. 2018;29(1):101–111. PubMed CrossRef
- Bielecka AM, Obuchowicz E. Antidepressant drugs can modify cytotoxic action of temozolomide. Eur J Cancer Care (Engl). 2017;26(5):e12551. PubMed CrossRef
- Peterson RK, McKeown T, Tabori U, et al. Neuropsychological impact of trametinib in pediatric low-grade glioma: a case series. Pediatr Blood Cancer. 2020;67(12):e28690. PubMed CrossRef
Please sign in or purchase this PDF for $40.
Save
Cite