LESSONS LEARNED AT THE INTERFACE OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Prim Care Companion CNS Disord 2023;25(3):22f03320
To cite: Donovan AL, Petriceks AH, Paudel S, et al. Use of physical restraints in the emergency department: rationale, risks, and benefits. Prim Care Companion CNS Disord. 2023;25(3):22f03320.
To share: https://doi.org/10.4088/PCC.22f03320
© 2023 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Massachusetts General Hospital, Boston, Massachusetts
bHarvard Medical School, Boston, Massachusetts
cColumbia University Mailman School of Public Health, New York, New York
‡All authors contributed equally to the work.
*Corresponding author: Aldis H. Petriceks, BA, Columbia University Mailman School of Public Health, 722 W 168th St, New York, NY 10032 ([email protected]).
Have you ever wondered whether use of physical restraints in the emergency department (ED) is safe, effective, and ethical? Have you been uncertain about which types of physical restraints can be employed and what complications can arise from their use? Have you been unsure about how often patients in physical restraints must be evaluated, what must be documented, and how long a patient can be restrained? If you have, the following case vignette and discussion should prove useful.
CASE VIGNETTE
Mr A, a 35-year-old Marine veteran, was brought to the ED by 6 police officers after he was seen making threatening martial arts gestures to people who were walking leisurely through a public park. He failed to respond verbally to questions by police officers in the park and to stop his threatening behavior when requested to do so. Upon his arrival to the ED, Mr A was wearing combat fatigues. He had an intense stare and was mute; he offered no personal or historical information. When the attending physician stepped toward him to perform the physical examination, Mr A suddenly kicked out his foot, clad in a steel-toed boot. As the attending physician retreated, Mr A lunged toward him. Hospital security quickly intervened and placed Mr A in 4-point locked leather restraints. Mr A was given intramuscular haloperidol and lorazepam.
After several hours, Mr A became calmer, and a physical examination was conducted. The physical examination revealed no acute findings. Laboratory testing (including electrolytes, a complete blood count, and liver function tests) was within normal limits. Urine toxicology testing was notable for the presence of delta-9-tetrahydrocannabinol and cocaine metabolites.
Initially, Mr A was quite guarded when he was interviewed by the consulting psychiatrist. He explained that he had recently been honorably discharged from the Marines after 10 years of military service, which included 3 combat tours. While in Afghanistan, he witnessed many of his friends being injured or killed. He began to have nightmares and flashbacks. After returning home from combat, he felt on edge and was prone to irritability and explosive anger. He used increasing amounts of illicit drugs, including cannabis and cocaine, to cope with his symptoms. On the day of his ED presentation, he had used both cannabis and intravenous cocaine, which triggered paranoia. When he was being brought to the ED, he believed that the police and doctors were attempting to orchestrate his kidnapping, and he sought to defend himself.
DISCUSSION
When Are Physical Restraints Indicated in the ED?
Physical restraints are the emergency intervention of last resort to manage agitated or aggressive behavior in the ED. Agitation is noted in up to 2.6% of all ED visits.1 While the goal is to prevent agitation and management with the least restrictive measures possible (eg, verbal de-escalation, use of medications, a calming environment) if it does develop, some patients do not respond to these measures. When least-restrictive measures fail and a patient poses an immediate danger to themselves or others,2 physical restraints can be used to protect the safety of the patient and those around them.
Physical and pharmacologic restraints have been compared in the medical literature. For instance, Sloane et al3 determined several patient risk factors that disposed individuals to receive pharmacologic restraints, including physically abusive behavior, severe mental status impairment, and frequent family visitation. The authors3 concluded that physical and pharmacologic restraints do represent distinct interventions with distinct indications and patient risk factors. Therefore, for the remainder of this discussion, we will focus specifically on “physical” or “mechanical” restraints as opposed to “chemical” or “pharmacologic” restraints. We will not address pharmacologic restraints and their specific indications, adverse effects, and ethical or legal considerations, nor will we discuss selection between physical or pharmacologic restraints, how the 2 forms might be combined, or how to transition between one form of restraint and another. The term restraints will be used to refer specifically to physical restraints.
What Are Alternatives to Use of Restraints?
For most patients, being in the ED is a stressful and overwhelming experience. Stress, physical pain, hunger, and discomfort can each contribute to emotional dysregulation and increase the potential for agitation. Addressing these vulnerabilities (through treating pain, offering food, increasing comfort [such as with a warm blanket]) can preemptively decrease the risk of agitation and therefore the use of restraints.
If a patient’s behavior begins to escalate, it is critical for staff to recognize this and intervene rapidly. Initial interventions include use of verbal de-escalation techniques, offers of oral medication, and involvement of the patient in decisions about which medications to take.4 Verbal de-escalation techniques (such as respecting personal space, establishing verbal contact, offering reassurance, identifying the patient’s wants and feelings, finding areas of agreement, setting clear limits, and offering choices)5 can be effective. Concurrently, and particularly if verbal de-escalation is unsuccessful, medications should be offered to the patient. These medications typically include benzodiazepines and first- or second-generation antipsychotics. Medication choice should be tailored to the patient’s diagnosis and when possible should take into account patient preference regarding which medication is provided and by what route it will be administered.6
Changing the physical environment is another possible intervention. If a patient is situated in a crowded or noisy area of the ED, simply moving them to a quieter space with greater privacy can reduce sensory stimulation and facilitate de-escalation.5
How Often Are Restraints Used in the ED?
Restraints are frequently used in EDs to manage (and prevent) aggressive or harmful behavior, to prevent falls, and to protect property and equipment. The rates, duration, and methods of restraint vary widely around the globe, as do their outcomes (eg, complications). For example, physical restraints (eg, use of elevated bed rails, wrist restraints, and belts) are the most frequently used care techniques in many countries, with a prevalence that ranges from 6% to 85%.7 Potential factors associated with variation in the prevalence of restraint use include the type of health care facility (eg, psychogeriatric unit), the location of the health care setting, the patient population (eg, geriatric, gender [men > women], people of color, the undomiciled, beneficiaries of Medicare and Medicaid, a diagnosis of a substance-related disorder or another major psychiatric disorder, a history of violence, presence of sensory impairments or cognitive decline/dementia), regulations, and policies for restraint use.7–10 The variation in the frequency of restraint use can also be influenced by organizational factors, such as the nurse-to-patient ratio, staff experience and training, health care facility characteristics (eg, availability of psychiatric beds, availability of safety measures), and proximity to practice audits.11,12 Notably, the ED environment is typically characterized by being highly stressful, having long wait times, and experiencing frequent disruptions or transitions in patient-provider communication that can provoke violence in some individuals and precipitate the application of restraints.
In the US, use of restraints decreased precipitously for Medicare and Medicaid beneficiaries who were treated in inpatient psychiatric facilities or long-term care facilities since more rigorous regulations and policies were implemented by the Department of Health and Human Services in 2007.13–15 However, disparities in the use of restraints in the US among racial and ethnically diverse populations are concerning.8–10,16 A recent multicenter study16 (N = 32,054) found that people of color, especially Black and Hispanic adults, being evaluated for psychiatric emergencies are restrained at much higher rates in the ED. Such a disparity in restraint use may reflect racism and other sources of bias at multiple levels within and beyond the emergency care continuum.
What Devices or Techniques Qualify as Restraints?
Restraints are defined by the Centers for Medicare and Medicaid Services (CMS) and the Joint Commission as “any manual method, physical or mechanical device, material, or equipment that immobilizes or reduces the ability of a patient to move his or her arms, legs, body, or head freely or a drug or medication when it is used to restrict or manage the patient’s behavior or restrict the patient’s freedom of movement and it is not a standard treatment or dosage for the patient’s condition.”2 Restraints can be further subdivided into nonviolent or non–self-destructive restraints (used to promote medical healing, such as preventing self-extubation) or violent or self-destructive restraints (used for the management of self-destructive behavior that jeopardizes the immediate physical safety of the patient, staff, or others).17 Restraints include soft restraints, hard (often leather) restraints, Posey vests, and veils or net beds. Seclusion is a type of restraint and is defined as “the involuntary confinement of a patient alone in a room or area from which the patient is physically prevented from leaving.”2 Seclusion may only be used for the management of violent or self-destructive behavior.17 Seclusion is most typically achieved by use of a locked room. Orthopedic devices, protective helmets, or methods used to prevent the patient from falling out of bed are not considered restraints.2
How Can Restraints Be Applied to Reduce the Risk of Physical Injuries?
Use of restraints is not a benign intervention; it is associated with morbidity and mortality. Restraints should only be applied by hospital staff who are well trained regarding their use. Soft restraints (with padding) may increase patient comfort, although very agitated patients may require hard, double-locked restraints to ensure safety. Patients should not be restrained in the prone position, as this position is associated with a higher risk of mortality.18,19 Rather, patients should be restrained in the supine position. If there is a concern for aspiration, the head of the bed can be elevated to 30 degrees. Patients with significant agitation, especially those at risk for sliding off or tipping over the stretcher, can be restrained in the “swimmer’s position,” with one arm raised and the other placed alongside the body.
After placement of restraints, the Joint Commission requires regular monitoring at intervals determined by the individual hospital policy. Those with significant cardiac or respiratory illness, as well as those who are severely intoxicated may benefit from more frequent monitoring. Patients should also be moved at regular intervals to prevent untoward sequelae of immobility, such as pressure ulcers, rhabdomyolysis, and paresthesias.20
If a patient is in 2-point restraints, the restraints should be rotated from one limb to another. The rule of thumb is to use the least restrictive form of restraints for the shortest time possible to decrease the risk of patient injury.
How Are Restraints Ordered and by Whom?
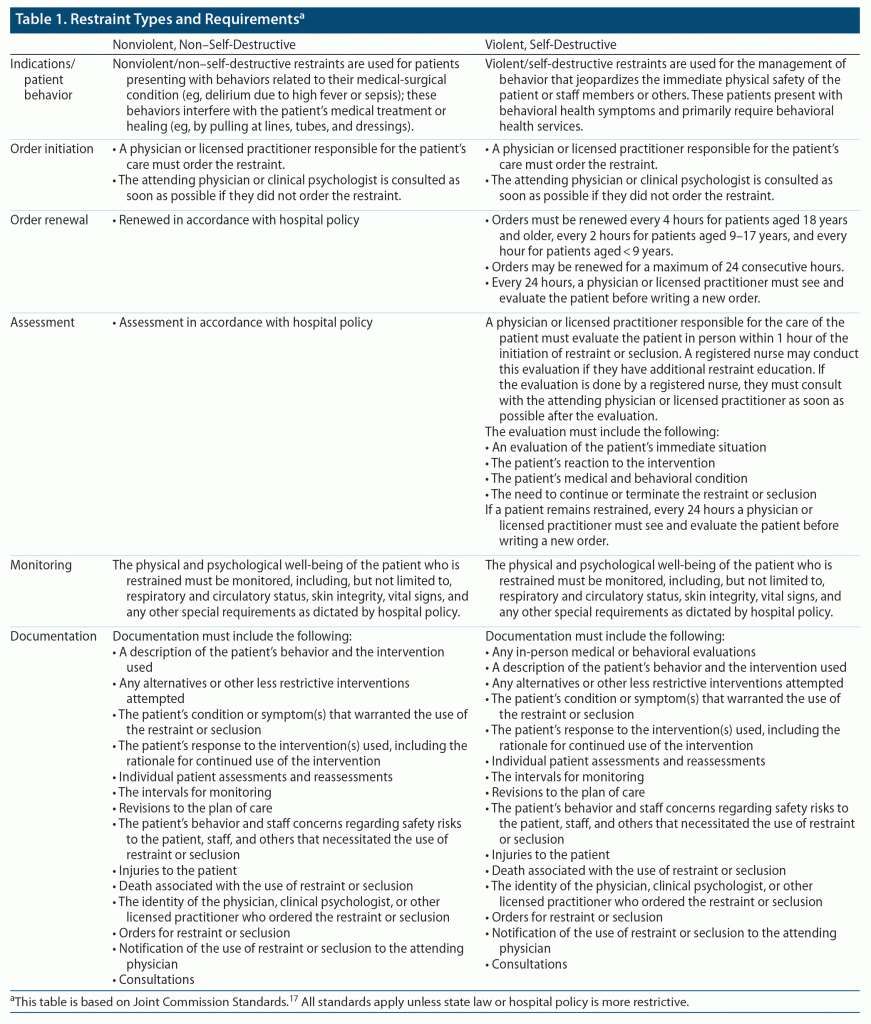
All forms of restraint require an individual medical order. The order must be written by a physician or licensed practitioner.17 The Joint Commission defines a licensed practitioner as “an individual permitted by law and by the organization to provide care, treatment, and services without direction or supervision.”17 Table 1 provides additional details.
How Frequently Must the Patient in Restraints Be Evaluated for the Need for Restraints and for Their Safety?
All patients must be evaluated in person (face-to-face) within 1 hour of restraint initiation for the management of violent and self-destructive behavior.17 The evaluation must be done by a physician or a licensed practitioner. A registered nurse may also conduct this evaluation if they have additional restraint education. If the evaluation is done by a registered nurse, they must consult with the attending physician or licensed practitioner as soon as possible after the evaluation. In addition, if the patient remains in restraints, a physician or licensed practitioner must evaluate the patient every 24 hours before writing a new order for restraints used to manage violent and self-destructive behavior.17 While in restraints, the physical and psychological well-being of the patient, including but not limited to respiratory and circulatory status, skin integrity, and vital signs, must be monitored at a frequency specified by hospital policy.17
How Can Hygiene Be Maintained While in Restraints?
Use of restraints often involves complicated discussions of patient rights and autonomy, as well as concerns about safety, dignity, and privacy. Maintaining personal hygiene in a timely and humane manner can be challenging when a patient is in restraints. Given that patients can be placed in restraints for myriad reasons for varying lengths of time, clinicians who order restraints should think proactively about approaching this intervention in a widely applicable but individualized manner.
Unfortunately, the medical literature about the management of toileting and the maintenance of hygiene while in restraints is limited. Concrete descriptions of effective practices (eg, how to best allow for elimination needs when restraints cannot be safely released in an agitated patient) are few.21,22
For instance, in 2003, the American College of Critical Care Medicine Task Force described recommendations for the promotion of patient safety while restrained in an intensive care unit (ICU).23 The authors23 noted that restrained patients can no longer provide for their basic needs of turning, eating, drinking, and toileting. As such, clinicians who care for these patients must be skilled in providing for these needs.23 Yet, it is unclear exactly what such skill might involve. The group noted that attainment of this goal may come in part through regular assessment of patient needs. They recommended that calm patients be assessed for complications of restraints at least every 4 hours, while agitated patients may require assessment every 15 minutes until they are calm.23 With regard to toileting needs, they recommended that clinicians evaluate agitated patients every 2 hours for potential needs for urination or defecation.23 Alternatively, if a patient is interactive, clinicians may offer an opportunity to toilet. However, these recommendations are unclear about the management of calm patients (eg, Should they be offered opportunities to toilet less frequently?).
Another challenge is determining how toileting should occur. For instance, clinicians will often be hesitant to withhold restraints to allow an agitated or violent patient to use the restroom. Even when a patient is calm, concerns arise when getting out of a hospital bed, and restraints might create fall risks, even with staff in attendance. In these cases, following institutional policies and applying clinical judgment can be conducted in concert. In the agitated and potentially violent patient, clinicians may offer to help the patient use a urinal or with cleaning while maximizing patient privacy, which may involve using restraints in such a way that it is possible for the patient to maneuver and cooperate with the toileting process. If a patient is not considered to be violent and may be moved, with or without support, to a private restroom, this procedure would be preferable. Patient safety, dignity, privacy, and autonomy should be considered throughout the toileting process. At the same time, approaches to toileting for restrained patients should be developed with a realistic view of an institution’s staffing and resources. Institutions should develop a workable approach to this problem, as failures in this regard have caused great discomfort and harm to patients.24
How Often Does the Order for Renewal of Restraints Need to Be Written?
Orders used for restraints for the management of violent or self-destructive behavior are time limited based on the age of the patient. These orders expire after 4 hours for patients aged ≥ 18 years, after 2 hours for patients 9 to 17 years, and after 1 hour for patients < 9 years.17 At the time of their expiration, the orders can be renewed according to these time limits for a maximum of 24 consecutive hours.17
Orders used for the management of nonviolent non–self-destructive behavior expire in accordance with individual hospital policy.17 One strategy frequently used by hospitals in the United States is to require renewal of the nonviolent non–self-destructive restraint order every 24 hours. The renewal of the order is then contingent on an evaluation by the clinical team and documentation that restraints are still required to provide safe and proper care. This strategy is helpful in allowing clinical teams a regular opportunity for reevaluation of the mental status and need for restraints in their patient, as well as in allowing the patient opportunities to be taken out of restraints if feasible. Clinicians should check with their specific institutional policies and legal restrictions to determine when they will need to place a new restraint order.
What Type of Documentation Is Required When a Patient Is in Restraints?
Accurate, timely, descriptive documentation is important to medical care in general and especially to the use of restraints. When ordering, continuing, and discontinuing restraints, clinicians should keep in mind the reasons and protocols associated with this documentation. The Joint Commission includes documentation of restraint use as one of their standards of practice.25 The Joint Commission first requires that clinicians document the specific medical or behavioral restraints used, as well as the behavior leading to the restraint (eg, what necessitated the use of restraints?). Clinicians are also expected to document the specific psychiatric or medical condition, if any, to which these behaviors are attributed. They should also document the restraint alternatives previously used and how or why those strategies were insufficient.
Documentation should also include descriptions of how the patient responded to restraints. Clinicians should indicate how often they reevaluated the patient, what they found on these reevaluations, and how their management changed in accordance with those findings. Any harm or injury caused or made possible by the restraints should also be documented. The restraint orders themselves should be documented, including renewed orders and the names of the ordering clinicians. Finally, it should be documented that the attending clinician was aware of the implementation of restraints, as well any consulting teams participating in the patient’s care while in restraints.25
The nuances of hospital policy pertaining to restraint may differ, as may the exact format of documentation. But, generally, institutions should have the above information written and signed in their electronic medical record should this information ever be requested by the patient, their health proxy, the legal system, or the Joint Commission.
Who Can Write an Order to Discontinue the Use of Restraints?
In general, the physician or licensed practitioner responsible for a patient’s care should be able to both order and discontinue an order for the use of restraints. In a hospital ED or psychiatric unit, this will often be done by the responding practitioner. Specific institutional policies should be referenced.
What Medical Risks Accompany the Use of Physical Restraints?
Decisions about when and how to employ physical restraints can be challenging in a variety of clinical settings (eg, the ED) in part due to the myriad consequences of physical restraints (Table 2). Major medical risks for those being restrained are physical, psychological, and moral/existential injuries. Unfortunately, physical injuries can be commonplace, particularly if the use of restraints is accompanied by inadequate evaluation and monitoring of the patient. Further, death is a rare but known complication of restraining patients.26,27 Strangulation, as well as complications of poor circulation/ischemia, cardiac stress, immobility, muscle weakness, skin injury, infection, incontinence, dehydration, and diminished appetite, are some of the reported physical injuries linked with the use of physical restraints. Major causes of death in those who have been restrained include asphyxia, cardiac arrest, blunt trauma, strangulation, thrombosis, rhabdomyolysis, fire, and drug interactions or overdoses.28,29 Similarly, adverse hospital outcomes of restraint use include functional decline and a longer length of hospital stay.30
Moral and psychological injuries can be debilitating for many individuals who are placed in restraints.31 The consequences of the psychological injury can be limited to the short term, like fear, rage, or isolation, or be long-term sequelae (like depression, anxiety, and posttraumatic stress disorder [PTSD]).26,32,33 Individuals with a history of trauma can experience a reactivation of their trauma response during and after the process of being restrained. Mistrust of health and mental health providers can ensue when physical restraint exacerbates an existing psychiatric condition.34 Low self-esteem and extreme distress have also been reported following use of physical restraints.35
In addition to the medical risks linked with being restrained, there are risks to the health care providers involved in the restraining process, which can be significant. The impact and consequences of restraining patients have been highlighted here, and further investigations are needed.36,37
Which Patients May Be Especially Vulnerable to the Psychological Trauma of Being Restrained?
Psychological trauma due to use of physical restraints is a serious health issue. Anyone who has experienced physical restraint has the potential to develop short- and long-term psychological sequelae. However, those with a history of physical or sexual trauma are especially vulnerable to the psychological trauma precipitated by using restraints.31,38 Treatment in the ED, where physical restraints are frequently applied, can retraumatize individuals with a sexual trauma history and place them at risk for decompensation due to the trauma response.38 Similarly, people have described the experience of being restrained in the ED as like that of being in prison,31 and those who have been held prisoner can be retraumatized by this experience. If someone has a history of PTSD, the risk of developing a variety of trauma responses, including decompensation of the illness, is increased. Others who are vulnerable to the psychological trauma of physical restraint use are the elderly, the undomiciled, those with substance use disorders, and those engaged in military combat.31
Case Vignette: What Happened to Mr A?
During Mr A’s entire psychiatric evaluation, he remained calm with no displays of aggression or overt paranoia. When the consulting psychiatrist described the events leading to his restraint, including his near assault of the attending physician, Mr A felt guilty and ashamed. He articulated that he did not want to injure anyone. After his discussion with the consulting psychiatrist, Mr A willingly participated in voluntary inpatient treatment at the Veterans Affairs hospital to address both his PTSD and substance use.
CONCLUSION
Restraints are the emergency intervention of last resort to manage agitated or aggressive behavior in the ED. Moreover, they should be applied only by hospital staff who are well trained regarding their use. All manner of restraints requires a time-limited medical order written by a physician or licensed practitioner.17
Clinicians must document the specific medical or behavioral restraints used, as well as the behavior leading to the restraint, what alternatives to restraint had been used, and how or why those strategies were insufficient. Unfortunately, physical complications of restraints include strangulation, as well as poor circulation/ischemia, cardiac stress, immobility, muscle weakness, skin injury, infection, incontinence, dehydration, and diminished appetite. The psychological sequelae of being restrained include retraumatization of those with a sexual trauma history, PTSD, and previous military combat.31 Knowledge of the reasons for restraints, the techniques that can minimize associated sequelae, and the process of ordering and monitoring restraints will facilitate effective and safe control of agitated patients.
Submitted: May 12, 2022; accepted August 23, 2022.
Published online: May 4, 2023.
Relevant financial relationships: Dr Vyas has received research salary support from Nestlé Purina PetCare Company. No other authors have disclosures to report.
Funding/support: None.
Clinical Points
- Physical restraints are the emergency intervention of last resort to manage agitated or aggressive behavior in the emergency department (ED); moreover, they should only be applied by hospital staff who are well trained regarding their use.
- Physical restraints can be subdivided into nonviolent or non–self-destructive restraints (used to promote medical healing, such as preventing self-extubation) or violent or self-destructive restraints (used for the management of self-destructive behavior that jeopardizes the immediate physical safety of the patient, staff, or others).
- All forms of physical restraint require an individual medical order, written by a physician or licensed practitioner; orders used for restraints for the management of violent or self-destructive behavior are time limited based on the age of the patient and the severity of the condition.
- Physical complications of physical restraints include strangulation, complications of poor circulation/ischemia, cardiac stress, immobility, muscle weakness, skin injury, infection, incontinence, dehydration, and diminished appetite.
- The psychological sequelae of being physically restrained include retraumatization of those with a sexual trauma history, posttraumatic stress disorder, and those who have served in military combat.
References (38)

- Miner JR, Klein LR, Cole JB, et al. The characteristics and prevalence of agitation in an urban county emergency department. Ann Emerg Med. 2018;72(4):361–370. PubMed CrossRef
- Centers for Medicare and Medicaid Services, Department of Health and Human Services. Condition of participation: patient’s rights. Federal Register 42 CFR §482.13. 2006; 71426–71428.
- Sloane PD, Mathew LJ, Scarborough M, et al. Physical and pharmacologic restraint of nursing home patients with dementia. Impact of specialized units. JAMA. 1991;265(10):1278–1282. PubMed CrossRef
- Knox DK, Holloman GH Jr. Use and avoidance of seclusion and restraint: consensus statement of the American Association for Emergency Psychiatry Project Beta Seclusion and Restraint Workgroup. West J Emerg Med. 2012;13(1):35–40. PubMed CrossRef
- Richmond JS, Berlin JS, Fishkind AB, et al. Verbal de-escalation of the agitated patient: consensus statement of the American Association for Emergency Psychiatry Project Beta De-escalation Workgroup. West J Emerg Med. 2012;13(1):17–25. PubMed CrossRef
- Wilson MP, Pepper D, Currier GW, et al. The psychopharmacology of agitation: consensus statement of the American Association for Emergency Psychiatry Project Beta Psychopharmacology Workgroup. West J Emerg Med. 2012;13(1):26–34. PubMed CrossRef
- Ambrosi E, Debiasi M, Longhini J, et al. Variation of the occurrence of physical restraint use in the long-term care: a scoping review. Int J Environ Res Public Health. 2021;18(22):11918. PubMed CrossRef
- Wong AH, Whitfill T, Ohuabunwa EC, et al. Association of race/ethnicity and other demographic characteristics with use of physical restraints in the emergency department. JAMA Netw Open. 2021;4(1):e2035241. PubMed CrossRef
- Schnitzer K, Merideth F, Macias-Konstantopoulos W, et al. Disparities in care: the role of race on the utilization of physical restraints in the emergency setting. Acad Emerg Med. 2020;27(10):943–950. PubMed CrossRef
- Khalid Z, Fana M, Payea R, et al. Disparities and variables associated with physical restraint for acute agitation in a nonpsychiatric emergency department. Prim Care Companion CNS Disord. 2019;21(6):19m02471. PubMed CrossRef
- Huizing AR, Hamers JP, de Jonge J, et al. Organizational determinants of the use of physical restraints: a multilevel approach. Soc Sci Med. 2007;65(5):924–933. PubMed CrossRef
- De Benedictis L, Dumais A, Sieu N, et al. Staff perceptions and organizational factors as predictors of seclusion and restraint on psychiatric wards. Psychiatr Serv. 2011;62(5):484–491. PubMed CrossRef
- Shields MC, Busch AB. The effect of Centers for Medicare and Medicaid’s inpatient psychiatric facility quality reporting program on the use of restraint and seclusion. Med Care. 2020;58(10):889–894. PubMed CrossRef
- Castle NG, Engberg J. The health consequences of using physical restraints in nursing homes. Med Care. 2009;47(11):1164–1173. PubMed CrossRef
- Agnes JE. Chemical and physical restraint use in the older person. Br J Med Pract. 2010;3(1):302.
- Carreras Tartak JA, Brisbon N, Wilkie S, et al. Racial and ethnic disparities in emergency department restraint use: a multicenter retrospective analysis. Acad Emerg Med. 2021;28(9):957–965. PubMed CrossRef
- The Joint Commission Comprehensive Accreditation and Certification Manual. The Joint Commission E-dition. Joint Commission Resources website. Accessed April 9, 2022. https://e-dition.jcrinc.com/MainContent.aspx
- Booth JS, Schraga ED. Four-point restraint. Medscape website. December 19, 2018. Accessed March 4, 2022. https://emedicine.medscape.com/article/1941454-overview
- Steinberg A. Prone restraint cardiac arrest: a comprehensive review of the scientific literature and an explanation of the physiology. Med Sci Law. 2021;61(3):215–226. PubMed CrossRef
- Coburn VA, Mycyk MB. Physical and chemical restraints. Emerg Med Clin North Am. 2009;27(4):655–667, ix. PubMed CrossRef
- Sharifi A, Arsalani N, Fallahi-Khoshknab M, et al. The principles of physical restraint use for hospitalized elderly people: an integrated literature review. Syst Rev. 2021;10(1):129. PubMed CrossRef
- Kalula SZ, Petros SG. Use of physical restraint in hospital patients: A descriptive study in a tertiary hospital in South Africa. Curationis. 2016;39(1):e1–e8. PubMed CrossRef
- Maccioli GA, Dorman T, Brown BR, et al; American College of Critical Care Medicine, Society of Critical Care Medicine. Clinical practice guidelines for the maintenance of patient physical safety in the intensive care unit: use of restraining therapies–American College of Critical Care Medicine Task Force 2001–2002. Crit Care Med. 2003;31(11):2665–2676. PubMed CrossRef
- Kontio R, Joffe G, Putkonen H, et al. Seclusion and restraint in psychiatry: patients’ experiences and practical suggestions on how to improve practices and use alternatives. Perspect Psychiatr Care. 2012;48(1):16–24. PubMed CrossRef
- Joint Commission International. Joint Commission Standards on Restraint and Seclusion/ Nonviolent Crisis Intervention Training Program. Crisis Prevention Institute; 2009.
- Evans LK, Cotter VT. Avoiding restraints in patients with dementia: understanding, prevention, and management are the keys. Am J Nurs. 2008;108(3):40–49, quiz 50. PubMed CrossRef
- Zusman J. Restraint and Seclusion: Improving Practice and Conquering the JCAHO Standards. Marblehead, MA: Opus Communications; 1997.
- Weiss EM. Deadly restraint: a nationwide pattern of death. The Hartford Courant; October 11–15, 1998.
- Joint Commission on Accreditation of Healthcare Organizations. Preventing restraint deaths. Sentinel Event Alert. 1998;(8):1–3. PubMed
- Chou MY, Hsu YH, Wang YC, et al. The adverse effects of physical restraint use among older adult patients admitted to the internal medicine wards: a hospital-based retrospective cohort study. J Nutr Health Aging. 2020;24(2):160–165. PubMed CrossRef
- Wong AH, Ray JM, Rosenberg A, et al. Experiences of individuals who were physically restrained in the emergency department. JAMA Netw Open. 2020;3(1):e1919381. PubMed CrossRef
- Gallop R, McCay E, Guha M, et al. The experience of hospitalization and restraint of women who have a history of childhood sexual abuse. Health Care Women Int. 1999;20(4):401–416. PubMed CrossRef
- Mohr WK, Pumariega AJ. Post restraint sequelae five years out: concerns and policy implications. Presented at the Annual American Psychiatric Association Meeting. May 9, 2001; New Orleans, Louisiana.
- Mohr WK, Mahon MM, Noone MJ. A restraint on restraints: the need to reconsider the use of restrictive interventions. Arch Psychiatr Nurs. 1998;12(2):95–106. PubMed CrossRef
- Soininen P, Putkonen H, Joffe G, et al. Does experienced seclusion or restraint affect psychiatric patients’ subjective quality of life at discharge? Int J Ment Health Syst. 2013;7(1):28. PubMed CrossRef
- Mohr WK, Petti TA, Mohr BD. Adverse effects associated with physical restraint. Can J Psychiatry. 2003;48(5):330–337. PubMed CrossRef
- Rakhmatullina M, Taub A, Jacob T. Morbidity and mortality associated with the utilization of restraints: a review of literature. Psychiatr Q. 2013;84(4):499–512. PubMed CrossRef
- Wynn R. Psychiatric inpatients’ experiences with restraint. J Forensic Psychiatry Psychol. 2004;15(1):124–144. CrossRef
Please sign in or purchase this PDF for $40.
Save
Cite