Objective: Cannabis withdrawal has not been studied in adults with attention-deficit/hyperactivity disorder (ADHD) who have high rates of cannabis use. We aimed to describe cannabis withdrawal, motivations to quit, and strategies to quit cannabis use in cannabis-dependent adults with ADHD.
Methods: Twenty-three adults with ADHD enrolled in a controlled clinical trial of pharmacotherapy (atomoxetine) for cannabis dependence (DSM-IV criteria) completed the Marijuana Quit Questionnaire (MJQQ) to provide information on their “most serious” quit attempt made without formal treatment. The study was conducted between November 2005 and June 2008.
Results: Participants were predominantly male (82.6%, n = 19), with a mean (SD) age of 27.4 (8.5) years (range, 18-53) at the start of their index quit attempt. The most common motive for quitting cannabis was “to save money” (87%, n = 20); the most common strategy to maintain abstinence was “stopped associating with people who smoke marijuana” (43%, n = 10). Almost all (96%, n = 22) subjects reported ≥ 1 cannabis withdrawal symptom; 7 (30%) met DSM-5 diagnostic criteria for cannabis withdrawal syndrome.
Conclusions: Participants with comorbid ADHD and cannabis dependence reported withdrawal symptoms similar to other samples of non-treatment-seeking cannabis-dependent adults with no psychiatric comorbidity. These findings suggest that ADHD does not influence cannabis withdrawal in the way that it does tobacco (nicotine) withdrawal.
Trial Registration: Data used in this secondary analysis came from ClinicalTrials.gov identifier: NCT00360269
Cannabis Withdrawal in Adults
With Attention-Deficit/Hyperactivity Disorder
ABSTRACT
Objective: Cannabis withdrawal has not been studied in adults with attention-deficit/hyperactivity disorder (ADHD) who have high rates of cannabis use. We aimed to describe cannabis withdrawal, motivations to quit, and strategies to quit cannabis use in cannabis-dependent adults with ADHD.
Methods: Twenty-three adults with ADHD enrolled in a controlled clinical trial of pharmacotherapy (atomoxetine) for cannabis dependence (DSM-IV criteria) completed the Marijuana Quit Questionnaire (MJQQ) to provide information on their “most serious” quit attempt made without formal treatment. The study was conducted between November 2005 and June 2008.
Results: Participants were predominantly male (82.6%, n = 19), with a mean (SD) age of 27.4 (8.5) years (range, 18–53) at the start of their index quit attempt. The most common motive for quitting cannabis was “to save money” (87%, n = 20); the most common strategy to maintain abstinence was “stopped associating with people who smoke marijuana” (43%, n = 10). Almost all (96%, n = 22) subjects reported ≥ 1 cannabis withdrawal symptom; 7 (30%) met DSM-5 diagnostic criteria for cannabis withdrawal syndrome.
Conclusions: Participants with comorbid ADHD and cannabis dependence reported withdrawal symptoms similar to other samples of non–treatment-seeking cannabis-dependent adults with no psychiatric comorbidity. These findings suggest that ADHD does not influence cannabis withdrawal in the way that it does tobacco (nicotine) withdrawal.
Trial Registration: Data used in this secondary analysis came from ClinicalTrials.gov identifier: NCT00360269
Prim Care Companion CNS Disord 2018;20(1):17m02203
To cite: Chauchard E, Hartwell KJ, McRae-Clark AL, et al. Cannabis withdrawal in adults with attention-deficit/hyperactivity disorder. Prim Care Companion CNS Disord. 2018;20(1):17m02203.
To share: https://doi.org/10.4088/PCC.17m02203
© Copyright 2018 Physicians Postgraduate Press, Inc.
aChemistry and Drug Metabolism Section, Intramural Research Program, National Institute on Drug Abuse, Baltimore, Maryland
bFaculté de Psychologie, Laboratoire de Psychologie des Pays de la Loire, Université de Nantes, Chemin de la Censive du Tertre, Nantes, France
cDepartment of Psychiatry and Behavioral Sciences, Medical University of South Carolina, Charleston, South Carolina
dDepartment of Psychiatry, University of Maryland School of Medicine, Baltimore, Maryland
*Corresponding author: David A. Gorelick, MD, PhD, PO Box 21247, MPRC-Tawes Bldg, Baltimore, MD 21228 ([email protected]).
Cannabis is the most commonly used illicit drug, with over 22 million current users aged 12 or older in the United States in 2014.1 The proportion of substance abuse treatment admissions for primary cannabis abuse increased from 12% in 1997 to 16.8% in 2013.2 However, the majority of cannabis users do not seek treatment.3
Considerable overlap exists between substance use disorders (SUDs), including cannabis, and attention-deficit/hyperactivity disorder (ADHD). Adults with alcohol or other SUDs have elevated rates of ADHD.4 Conversely, childhood and untreated adult ADHD are associated with a higher risk for comorbid SUDs.5 Cannabis use disorders are a particular concern. For example, a chart review of children and adolescents receiving psychiatric services in a large university hospital system over the previous decade found that cannabis use disorders were the most prevalent SUD, accounting for over 80% of all SUD diagnoses.6 Cannabis is the most commonly used illicit drug by adults with ADHD.7,8 However, the underlying etiology for elevated rates of cannabis dependence in ADHD is not clear. Adults with cannabis use disorders and ADHD have an earlier age at first use,9 a higher level of consumption,10 and a higher level of cannabis-associated impairment9,10 than cannabis users without ADHD.
To our knowledge, no study has described cannabis withdrawal symptoms in individuals with ADHD. Substance withdrawal symptoms in individuals with ADHD have been studied only for nicotine. Nicotine withdrawal symptoms were more frequent11 and more intense11–14 in those with ADHD than in those without the disorder. Those with ADHD experienced more somatic symptoms, more negative affect, and more intense craving.14
There is limited research on the role that psychiatric comorbidity plays in attempts to quit cannabis use. In non–treatment-seeking populations without psychiatric comorbidity, attempts to quit cannabis use without formal treatment are often motivated by concerns over the negative impact marijuana has on health and social image.15 We are unaware of any studies addressing these issues in treatment-seeking cannabis users with psychiatric comorbidity such as ADHD.
The goal of the present study is to evaluate the experience of cannabis withdrawal, motivations to quit, and strategies used to quit cannabis use in treatment-seeking, cannabis-dependent adults with ADHD.
METHODS
Study Design and Procedures
Individuals between 18 and 65 years of age seeking treatment for cannabis dependence (DSM-IV criteria) were recruited through local flyers and newspaper and internet advertisements to participate in a randomized, double-blind, placebo-controlled outpatient clinical trial investigating atomoxetine for treatment of current comorbid ADHD and cannabis dependence.16 The study was approved by the Medical University of South Carolina Institutional Review Board and registered at ClinicalTrials.gov (identifier NCT00360269). All participants provided written informed consent prior to any study procedures and were paid for their participation.
Exclusion criteria included current dependence on substances other than cannabis or nicotine, lifetime history of schizophrenia or bipolar disorder, significant current suicide risk (based on Structured Clinical Interview for DSM-IV-TR [SCID]), significant cognitive impairment, pregnant or nursing women, current major medical illnesses (eg, unstable angina, chronic obstructive pulmonary disease, renal disease, infectious hepatitis, or HIV), lack of stable housing, or current treatment with benzodiazepines, antidepressants, or antipsychotic medication. The SCID17 was used to assess current cannabis dependence and other substance use and psychiatric disorders. Participants were further assessed using the Conners’ Adult ADHD Diagnostic Interview, with symptoms corroborated by someone who knew the participant well (eg, spouse/partner, parent, sibling, or close friend) completing the Conners’ Adult ADHD Rating Scale-Observer.18 A physical examination was conducted to assess physical health. The Marijuana Quit Questionnaire (MJQQ)19 was administered at the baseline visit after randomization to study medication. The MJQQ is a 176-item semistructured instrument that collects data in 3 domains regarding the individual’s self-defined “most difficult” quit attempt without formal treatment outside a controlled setting: sociodemographic, cannabis use history (including related problems), and withdrawal experience, including withdrawal symptoms, motivation to quit, and strategies to maintain abstinence.
Statistical Analysis
Descriptive statistics are reported using mean (SD) for continuous outcomes and percent (n) for categorical outcomes. Comparisons of subjects who completed the MJQQ versus those who did not were investigated using the χ2 test for categorical data and independent t test for continuous data. Two-tailed α for significance was .05. Statistical tests were conducted with SPSS version 20 (SPSS, Inc, Chicago, Illinois).
RESULTS
Participant Demographics
Forty-two participants were eligible to take the MJQQ, of whom 30 were administered the questionnaire and 23 provided sufficient data for analysis. The majority of participants were single, young-adult, white men who became regular (at least weekly) cannabis users as adolescents (Table 1). The 23 participants included in this analysis do not differ significantly from the 7 participants who did not complete the MJQQ in age, sex, education, age at their first cannabis use, or age at their first weekly use (Table 1). All but 1 participant (96%) met at least 1 criterion for lifetime cannabis dependence; almost two-thirds (65%, n = 15) met at least 3 criteria for lifetime cannabis dependence.
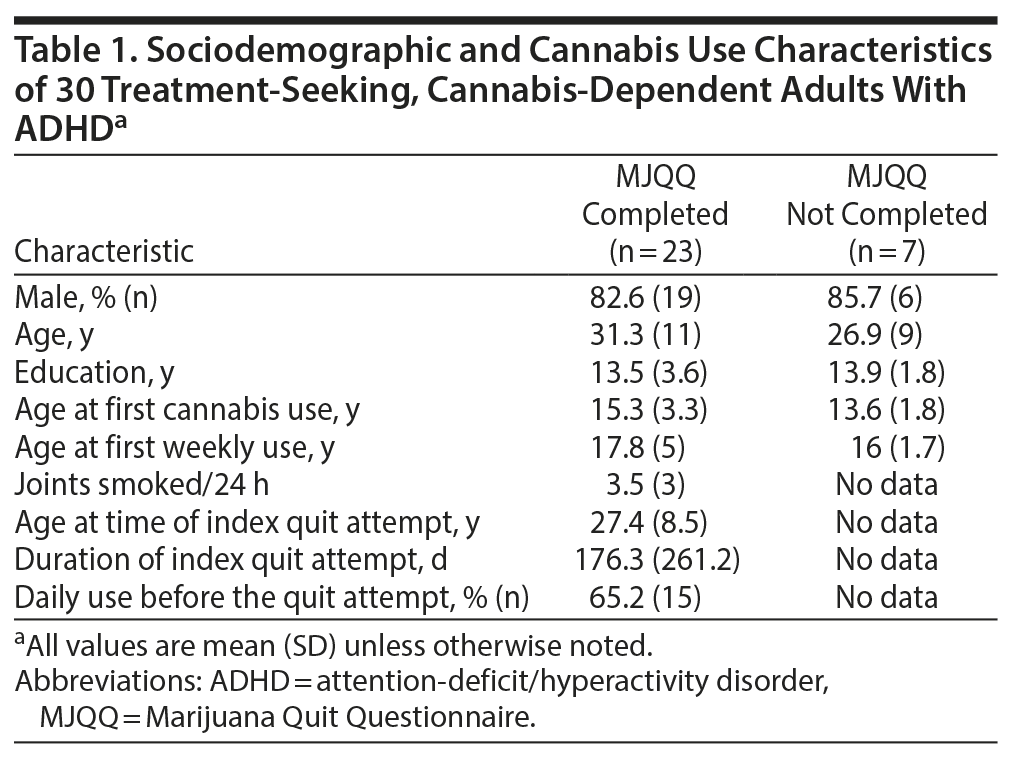
Characteristics of Index Quit Attempt
The index cannabis quit attempt started 5 days to 12 years before the study interview when subjects were 27.4 (8.5) (range, 18–53) years old. During the 6 months prior to the index quit attempt, 65% (n=15) of subjects used cannabis daily and 100% (n=23) at least weekly. Ninety-six percent smoked marijuana, averaging 3.5 (3.0) joints per day (range, 0–12). Use of other psychoactive substances at least weekly was common during the 6 months before the quit attempt, but heavy use (6–7 days per week) was less common: 64% and 30% of subjects used at least weekly or heavily, respectively, for caffeine; 52% and 0% for alcohol; 48% and 30% for tobacco; 48% and 4% for non-narcotic pain medication (eg, aspirin, acetaminophen, ibuprofen); 39% and 0% for stimulants (eg, cocaine and amphetamines); 17% and 0% for hallucinogens (eg, LSD [lysergic acid diethylamide], mescaline); 17% and 0% for sleeping aids (eg, diphenhydramine); 14% and 0% for sedatives (eg, benzodiazepines, barbiturates); and 13% and 0% for narcotic pain medications (eg, codeine, oxycodone).
At least three-quarters of participants, including 94% (n=20) of caffeine users, 84% (n=18) of alcohol users, and 93% (n=20) of tobacco users, reported no decrease in their use of the most commonly reported legal and illegal psychoactive substances during their quit attempt.
Motives for Quitting and Abstinence Strategies
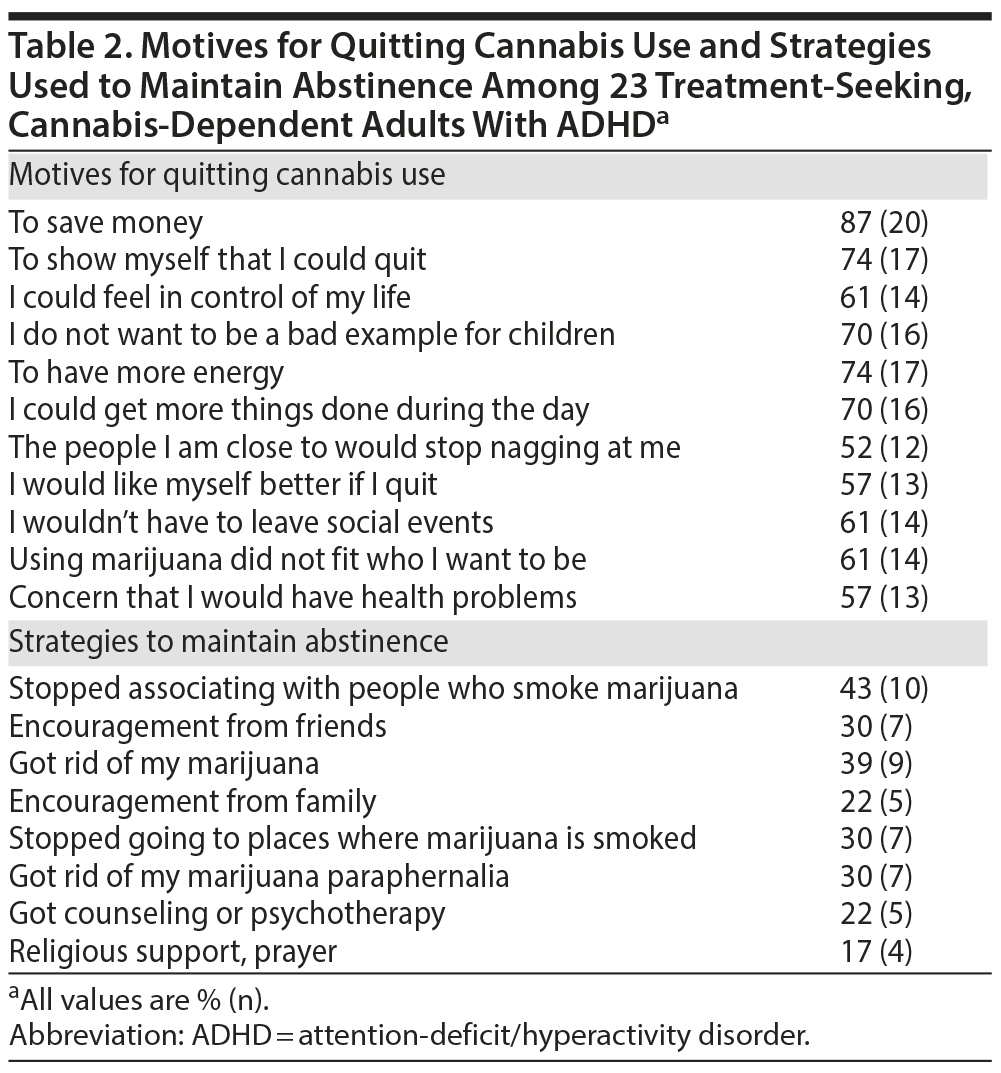
Participants reported a mean of 12.5 (6.1) (range, 0–23) motives to quit cannabis use (Table 2). The most common motive was “to save money” (87%, n = 20, of the sample), followed by “to show myself that I could quit” (74%, n = 17) and “to have more energy” (74%, n = 17). Seventy-eight percent of participants used at least 1 strategy to help maintain abstinence (Table 2), with a mean of 2.7 (2.5) (range, 0–9) such strategies per participant. The most common strategies were “stopped associating with people who smoke marijuana” (43% of the sample, n = 10) and “got rid of my marijuana” (39%, n = 9).
Cannabis Withdrawal Symptoms and Syndrome
Ninety-five percent of participants reported experiencing at least 1 cannabis withdrawal symptom. The most common withdrawal symptoms were craving for marijuana (57%, n = 13), feeling restless (52%, n = 12), trouble falling asleep (52%, n = 12), feeling angry (52%, n = 12), feeling bored (48%, n = 11), feeling irritable/jumpy (48%, n = 11), and feeling anxious/nervous (48%, n = 11) (Table 3). Seven (30%) participants met DSM-520 diagnostic criteria for cannabis withdrawal syndrome. The most common DSM-5 withdrawal symptoms were insomnia (57%, n = 13), irritability/anger/aggression (57%, n = 13), and restlessness (52%, n = 12) (Table 4).


DISCUSSION
To our knowledge, this study is the first to evaluate cannabis withdrawal symptoms in individuals with ADHD. Participants in this study (adults with ADHD) experienced similar cannabis withdrawal symptoms as 385 adult, non–treatment-seeking subjects with no major psychiatric comorbidity in a previous study21 that used the same interview instrument (MJQQ). In both samples, almost all participants met at least 1 lifetime criterion for DMS-IV cannabis dependence (96% in ADHD sample and 99% in the noncomorbid sample), although fewer participants in the ADHD sample met at least 3 criteria for lifetime cannabis dependence (65% vs 91%). In both samples, almost all participants (95%) reported experiencing at least 1 withdrawal symptom during their index quit attempt. The most common withdrawal symptoms were increased craving for marijuana (57% ADHD sample vs 76% in the noncomorbid sample), mood changes (48%–52% vs 34%–50%, respectively), and difficulties falling asleep (52% vs 47%, respectively). There was no significant difference in proportion of participants meeting DSM-5 criteria for cannabis withdrawal syndrome (30% vs 41%, respectively; P = .39 by Fisher exact test).21
These findings suggest that ADHD may not influence cannabis withdrawal in the way that it does tobacco (nicotine) withdrawal. Several studies reported that nicotine withdrawal symptoms were more frequent11 and more intense11–14 in individuals with ADHD than in those without the disorder. Somatic symptoms, negative affect, and increased craving also appear more prominent in those with ADHD.14 The interaction between ADHD and nicotine withdrawal may be related, in part, to their common association with decreased brain dopaminergic function,22 resulting in an additive effect on withdrawal symptoms. This commonality also exists with cannabis withdrawal,23 leaving unclear the mechanism of its differential interaction with ADHD.
This study has several limitations. First, lack of a contemporaneous non-ADHD control group within the study precludes a statistical comparison of the impact of ADHD on cannabis withdrawal in treatment-seeking adult cannabis users, although our historical comparison group was similar in age, degree of cannabis dependence, and interview instrument. Second, the sample was relatively small, limiting the power to detect clinical profiles of withdrawal symptoms. Third, while participants had no other current (within prior 3 months) substance dependence at the time of study interview, we cannot be certain that they were free of any dependence at the time of their index quit attempt. However, we consider this possibility unlikely, as, except for tobacco (30%) and caffeine (30%), almost no subjects were heavy users of noncannabis psychoactive substances during the 6 months before the start of their index quit attempt. Finally, data were obtained by retrospective self-report with no external corroboration. Adult cannabis users not in treatment and without psychiatric comorbidity have been found to give reliable retrospective self-report about their cannabis use history.24,25 However, there is evidence that adolescents with ADHD have difficulty reporting their nicotine withdrawal symptoms.12 The success of the quit attempt could not be used as a dependent variable in statistical analyses because current cannabis dependence was an eligibility criterion for the underlying clinical trial. Future longitudinal studies of cannabis withdrawal with a non-ADHD control group and contemporaneous data collection are needed to better understand the influence of ADHD on cannabis withdrawal.
Submitted: August 4, 2017; accepted December 4, 2017.
Published online: February 22, 2018.
Potential conflicts of interest: None reported.
Funding/support: Intramural Research Program, National Institute on Drug Abuse, NIH (Dr Gorelick); NIH grants R21DA0188221 (Dr McRae-Clark), T32DA007288 (BJS). Dr Chauchard received funding from the Interministerial Mission for the Fight against Drugs and Drug Addiction (MILDT; French Government) and the University of Toulouse II, Le Mirail.
Role of sponsor: The funding sources had no role in the design, analysis, interpretation, or publication of this study.
REFERENCES
1. Center for Behavioral Health Statistics and Quality. Behavioral Health Trends in the United States: Results From the 2014 National Survey on Drug Use and Health. HHS Publication No. SMA 15-4927, NSDUH Series H-50. SAMHSA.gov website. https://www.samhsa.gov/data/sites/default/files/NSDUH-FRR1-2014/NSDUH-FRR1-2014.htm. 2015.
2. Substance Abuse and Mental Health Services Administration, Center for Behavioral Health Statistics and Quality. Treatment Episode Data Set (TEDS): 2003–2013. National Admissions to Substance Abuse Treatment Services. Vol BHSIS Series S-75, HHS Publication No. (SMA) 15-4934. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2014.
3. Stinson FS, Ruan WJ, Pickering R, et al. Cannabis use disorders in the USA: prevalence, correlates and co-morbidity. Psychol Med. 2006;36(10):1447–1460. PubMed CrossRef
4. Wilens TE. Attention-deficit/hyperactivity disorder and the substance use disorders: the nature of the relationship, subtypes at risk, and treatment issues. Psychiatr Clin North Am. 2004;27(2):283–301. PubMed CrossRef
5. Wilens TE, Adamson J, Sgambati S, et al. Do individuals with ADHD self-medicate with cigarettes and substances of abuse? results from a controlled family study of ADHD. Am J Addict. 2007;16(suppl 1):14–21; quiz 22–23. PubMed CrossRef
6. Wu LT, Gersing K, Burchett B, et al. Substance use disorders and comorbid Axis I and II psychiatric disorders among young psychiatric patients: findings from a large electronic health records database. J Psychiatr Res. 2011;45(11):1453–1462. PubMed CrossRef
7. Biederman J, Wilens T, Mick E, et al. Psychoactive substance use disorders in adults with attention deficit hyperactivity disorder (ADHD): effects of ADHD and psychiatric comorbidity. Am J Psychiatry. 1995;152(11):1652–1658. PubMed CrossRef
8. Murphy K, Barkley RA. Attention deficit hyperactivity disorder adults: comorbidities and adaptive impairments. Compr Psychiatry. 1996;37(6):393–401. PubMed CrossRef
9. Rooney M, Chronis-Tuscano A, Yoon Y. Substance use in college students with ADHD. J Atten Disord. 2012;16(3):221–234. PubMed CrossRef
10. Faraone SV, Wilens TE, Petty C, et al. Substance use among ADHD adults: implications of late onset and subthreshold diagnoses. Am J Addict. 2007;16(suppl 1):24–32, quiz 33–34. PubMed CrossRef
11. Pomerleau CS, Downey KK, Snedecor SM, et al. Smoking patterns and abstinence effects in smokers with no ADHD, childhood ADHD, and adult ADHD symptomatology. Addict Behav. 2003;28(6):1149–1157. PubMed CrossRef
12. Gray KM, Baker NL, Carpenter MJ, Lewis AL, et al. Attention-deficit/hyperactivity disorder confounds nicotine withdrawal self-report in adolescent smokers. Am J Addict. 2010;19(4):325–331. PubMed
13. McClernon FJ, Kollins SH, Lutz AM, et al. Effects of smoking abstinence on adult smokers with and without attention deficit hyperactivity disorder: results of a preliminary study. Psychopharmacology (Berl). 2008;197(1):95–105. PubMed CrossRef
14. McClernon FJ, Van Voorhees EE, English J, et al. Smoking withdrawal symptoms are more severe among smokers with ADHD and independent of ADHD symptom change: results from a 12-day contingency-managed abstinence trial. Nicotine Tob Res. 2011;13(9):784–792. PubMed CrossRef
15. Copersino ML, Boyd SJ, Tashkin DP, et al. Quitting among non-treatment-seeking marijuana users: reasons and changes in other substance use. Am J Addict. 2006;15(4):297–302. PubMed CrossRef
16. McRae-Clark AL, Carter RE, Killeen TK, et al. A placebo-controlled trial of atomoxetine in marijuana-dependent individuals with attention deficit hyperactivity disorder. Am J Addict. 2010;19(6):481–489. PubMed CrossRef
17. First MS, Gibbon M, Williams JBW. Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Research version, Patient Edition. SCIP-I/P. New York, NY: Biometrics Research, New York State Psychiatric Institute; 1994.
18. Conners CK, Erhardt D, Sparrow E. Conners’ Adult ADHD Rating Scale (CAARS). North Tonawanda, NY: Multi-Health Systems; 1999.
19. Levin KH, Copersino ML, Heishman SJ, et al. Cannabis withdrawal symptoms in non-treatment-seeking adult cannabis smokers. Drug Alcohol Depend. 2010;111(1–2):120–127. PubMed CrossRef
20. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
21. Gorelick DA, Levin KH, Copersino ML, et al. Diagnostic criteria for cannabis withdrawal syndrome. Drug Alcohol Depend. 2012;123(1–3):141–147. PubMed CrossRef
22. Volkow ND, Wang GJ, Newcorn J, et al. Depressed dopamine activity in caudate and preliminary evidence of limbic involvement in adults with attention-deficit/hyperactivity disorder. Arch Gen Psychiatry. 2007;64(8):932–940. PubMed CrossRef
23. Oleson EB, Cheer JF. A brain on cannabinoids: the role of dopamine release in reward seeking. Cold Spring Harb Perspect Med. 2012;2(8). PubMed CrossRef
24. Ensminger ME, Juon HS, Green KM. Consistency between adolescent reports and adult retrospective reports of adolescent marijuana use: explanations of inconsistent reporting among an African American population. Drug Alcohol Depend. 2007;89(1):13–23. PubMed CrossRef
25. Fendrich M, Mackesy-Amiti ME. Inconsistencies in lifetime cocaine and marijuana use reports: impact on prevalence and incidence. Addiction. 1995;90(1):111–118. PubMed CrossRef
Enjoy free PDF downloads as part of your membership!
Save
Cite
Advertisement
GAM ID: sidebar-top

