ABSTRACT
Objective: As the coronavirus disease (COVID-19) outbreak is the first pandemic to occur in the modern smartphone era, people universally rely on their electronic devices to stay current on the rapidly evolving circumstances. The objective of this study was to examine how daily screen time levels affect the mental health of health care workers attempting to stay up to date on the ever-changing COVID-19–related information available to them.
Methods: Health care workers at an academic teaching hospital were asked to participate in a 12-question online-based survey between the dates of May 30, 2020, and June 3, 2020. The questions included their sex, age range, occupation, department, daily screen time, changes in screen time in the last 4 weeks, and mental health outcomes such as sleep, mood, anxiety, and difficulty controlling worry.
Results: No association was found between age, sex, occupation, and screen time. There was a statistically significant association between the type of department and daily screen time hours (P = .012). A positive trend was noted between screen time and sleep disruption (P = .09). An increase in hours in the last 4 weeks was associated with age (P = .03). A positive trend was also noted for an increase in screen hours and sleep disruption (P = .11) and anxiety (P = .10).
Conclusions: A possible explanation for our finding of screen time not being associated with mental health outcomes could be that the knowledge that information was readily available through technology provided comfort to people as the pandemic evolved and brought changes to their daily lives.
Prim Care Companion CNS Disord 2021;23(5):21m02959
To cite: Le C, Khalid Z, Avramut C, et al. Psychological effects of screen time in health care workers during the COVID-19 pandemic. Prim Care Companion CNS Disord. 2021;23(5):21m02959.
To share: https://doi.org/10.4088/PCC.21m02959
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Central Michigan University, Saginaw, Michigan
bCentral Michigan University, College of Medicine, Mt Pleasant, Michigan
cWestern University of Health Sciences, College of Osteopathic Medicine of the Pacific, Pomona, California
dDivision of Research, Case Western University, Cleveland, Ohio
*Corresponding author: Zaira Khalid, MD, 1000 Houghton Ave, Saginaw, MI 48602 ([email protected]).
Due to the novel coronavirus disease 2019 (COVID-19) outbreak, declared a pandemic on March 11, 2020 by the World Health Organization (WHO), many countries have issued social distancing and quarantine orders in an effort to contain the contagious spread.1 The first case reported in the United States in the same month further highlighted the importance of communication and coordination between clinicians and public health authorities.2 The measures to reduce person-to-person contact and minimize airborne transmission have forced millions of people, including health care workers on the frontline of the pandemic, to remain connected and informed electronically. With forced isolation and uncertainty, mental health challenges arise. However, battling these threats becomes increasingly difficult for health care workers (doctors, nurses, respiratory therapists) who face additional stressors related to direct exposure to the virus and providing care for severely ill patients under adverse circumstances.3,4
Screen time refers to time spent using an electronic device with a screen such as a smartphone, computer, or television.5 Although previous studies6 have shown the detrimental effects of higher levels of exposure on child and adolescent development (including greater obesity and depressive symptoms, less healthy diet, and poorer quality of life), limited data exist surrounding its association with adult mental health and well-being. As the first pandemic in the modern smartphone era, people universally rely on their electronic devices to stay current on the rapidly evolving circumstances. We aim to examine how daily screen time levels affect the mental health of health care workers attempting to stay up to date on the ever-changing COVID-19–related information available to them.
METHODS
This study was conducted at an academic teaching hospital located in Saginaw, Michigan. All health care workers were invited to complete an online survey using SurveyMonkey between the dates of May 30, 2020, and June 3, 2020. By the end of the data collection period (June 3, 2020), the state of Michigan had a cumulative total of 59,666 COVID-19 cases; Saginaw County, where the study was conducted, had a cumulative total of 1,109 cases. This study was approved by the Central Michigan University Institutional Review Board.
The inclusion criteria were health care workers providing direct patient care and able to understand English. The exclusion criteria were limited to non-English speakers and those not providing direct patient care. Eligible health care workers were those who worked solely with inpatients and included physicians, nurses, inpatient pharmacists, occupational and physical therapists, technicians, transcriptionists, respiratory therapists, and phlebotomists. All hospital departments were included (emergency, intensive care unit, inpatient trauma, cardiology, surgery, maternity, pediatrics, neonatal, psychiatric, neurology, oncology, and pharmacy).
Measures
A 12-item anonymous online-based questionnaire was used to obtain participant demographics including sex, age range, occupation, and hospital department in which they worked. Each participant was asked to report his or her current screen time on a daily basis ranging from 1 to 8 hours, with screen time being defined as time spent using a cellphone, a computer, and watching television for work-related or personal use, excluding time spent on these devices for telemedicine or use of an electronic medical record. Next, 1 “yes/no” item asked if the respondent had an increase in screen hours over the last 4 weeks. Those who experienced an increase in screen time were asked to report the amount of increased hours ranging from 1 to ≥ 4.
In the second part of the survey, participants were asked to rank on a scale of 1–6 how often they experienced changes in their mood, anxiety, sleep, and ability to control worry. The scale used the rankings 1 = 0 days, 2 = 1–3 days, 3 = 4–7 days, 4 = 8–11 days, and 5 = ≥ 12 days. The last part of the survey asked participants if they had avoided situations in the past 4 weeks that reminded them of a previous traumatic event using the same rating scale of 1–6.
Sample Size and Statistical Analysis
A sample size of N = 68 was estimated to have 80% power at a 0.05 level of significance to detect medium effect size Spearman correlations. The analyses were computed in 3 stages. In stage 1, frequency distributions were computed for each of the categorical demographic variables to describe the characteristics of the study sample. Given that all study and outcome variables were measured as ordinal categorical variables, stage 2 examined the associations of screen time and the demographic variables with the 4 single-item outcomes of depressed mood, sleep, anxiety, and worry using χ2 statistics and Spearman rank order correlations. These analyses were designed to test the major study hypothesis regarding increased screen time on the mental health outcomes and to identify possible demographic confounders. A follow-up regression analysis would control for any relevant demographic confounders in the final test of the associations between screen time and the mental health outcomes. In the last stage, the Spearman correlation analyses were repeated but only for that segment of the sample that reported an increase in screen time over their normal screen time hours.
RESULTS
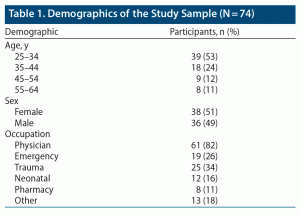
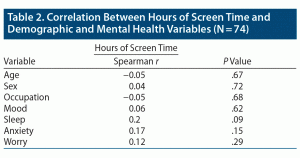
The total number of survey responses received was 74. Forty-nine percent of the respondents were women, and 53% were within the age group 25–34 years, followed by 24% in the age group 35–44 years (Table 1). For the purpose of the study, occupation was grouped into 2 categories: physician and nonphysician—82% of the participants were physicians. There was no statistically significant (P < .05) association between screen time and the demographic variables sex, age, and occupation or outcomes of depression, sleep, anxiety, and worrying (Table 2).
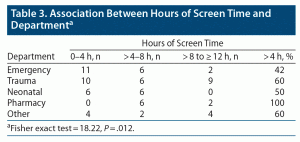
Departments were categorized as emergency, trauma, neonatal, pharmacy, and other. The highest response rate was from trauma (34%), followed by emergency (26%), neonatal (16%), pharmacy (11%), and other (13%). There was a statistically significant association between the type of department and daily screen time hours (P = .012) as seen in Table 3. Trauma reported the highest number of participants in the daily screen time category of 8 to ≥ 12 hours. The percentage of participants reporting daily use > 4 hours was highest in those working in pharmacy (100%), followed by trauma (60%), other (60%), neonatal (50%), and emergency (42%).
We evaluated if daily screen hours of the entire sample size were associated with the 4 mental health outcomes (mood, sleep, anxiety, worry); however, these findings were statistically nonsignificant. Still, as seen in Table 2, a positive trend was noted in the correlation between screen time and sleep (P = .09).
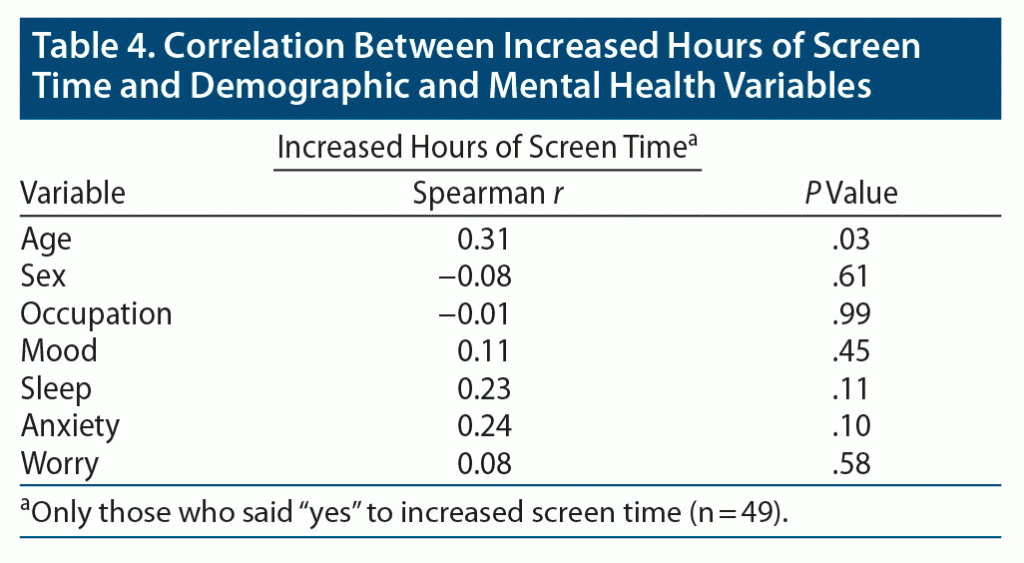
Next, we examined the data of only those participants that reported “yes” to the question: “Was there an increase in the amount of screen time in the last 4 weeks?” (n = 49, 66%). An increase in hours was associated with age (P = .03). Positive trends were noted for screen hours, with increases in sleep disturbances and anxiety days (Table 4).
DISCUSSION
Over the last few decades, screen time has become both a universal and integral part of everyday life. This concept continues to be under significant research in relation to mental health, as it is influenced not only by the content people are exposed to, but also by the amount of time they devote to their devices.7 Our research focused on the effects of screen time specifically during a challenging period in history—the early COVID-19 pandemic—in a notably vulnerable population—health care professionals.
We found no association between our demographics (sex, age, occupation) and mental health outcomes. The type of department that the health care provider worked in did have an association with screen time hours, with 100% of those working in pharmacy reporting use of > 4 hours of screen time daily. This finding could be a result of the ever-changing treatment guidelines and their development during a global pandemic, requiring those in pharmacy to stay updated via their devices such as phones and laptops. The trauma department had the highest number of people who reported > 8 to ≥ 12 daily screen time hours. This finding could also be a result of the ever-changing treatment guidelines and their development during a global pandemic, requiring those in the trauma department to stay up to date electronically. The abundance of new information regarding the pandemic has been recognized by the WHO as an “infodemic,” referring to the abundance of new information, as well as misinformation, disinformation, and rumors regarding provider safety, medications, treatment, and protocols that are ever changing.8
Unlike studies such as that of Wu et al,9 which showed a positive association between high amounts of screen time and anxiety, depression, and poor sleep quality, we found no correlation between total hours of screen time and our 4 chosen mental health outcomes. We did, however, find a positive trend in the correlation between screen time and sleep, which is similar to a study by Christensen et al,10 who also found that exposure to screen time negatively impacted sleep. It is important to note that these studies9,10 were not conducted during a global pandemic. A possible explanation for our findings could be that the knowledge and availability of information through technology were able to provide comfort as the evolving pandemic brought changes to our daily lives.
Interestingly, we also found that health care workers who reported an increase in their screen time over the last 4 weeks also showed a positive trend toward increased anxiety and sleep disturbances. Thus, the deviation from an individual’s baseline screen time is also important to note. Disturbances of sleep can result in mood disturbances, anxiety, and cognitive changes and ultimately can affect health care workers’ performance at work.11
The COVID-19 pandemic is unique in that it is the first to occur during a time of rapidly growing digital technology, the use of which comprises a significant portion of not only the health care workers’ workday but also their personal and free time. The effects of screen time on mental health have been heavily studied; however, the effects during a pandemic have not. Our data raise the question of whether health care workers utilize screen time to alleviate heightened worries during a pandemic or is pure curiosity during uncertain times feeding this deviation from an individual’s daily screen time quota?
Submitted: February 19, 2021; accepted May 19, 2021.
Published online: August 26, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Clinical Points
- In health care workers, an increase in screen time from baseline use can result in sleep disturbances and anxiety.
- Inpatient trauma and pharmacy departments were noted to have the highest hours of screen time during the early stages of the COVID-19 pandemic.
- In health care workers, technology and the ability to access information immediately could help alleviate the anxiety associated with a global pandemic.
References (11)

- World Health Organization. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19 - 11 March 2020. Accessed July 22, 2021. who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020
- Holshue ML, DeBolt C, Lindquist S, et al; Washington State 2019-nCoV Case Investigation Team. First case of 2019 novel coronavirus in the United States. N Engl J Med. 2020;382(10):929–936. PubMed CrossRef
- Huremović D. Social Distancing, Quarantine, and Isolation. In: Psychiatry of Pandemics, by Damir Huremović, Switzerland. Cham, Switzerland: Springer;2019:85–94.
- Huremović D. Quarantine and Isolation: Effects on Healthcare Workers. In: Psychiatry of Pandemics, by Damir Huremović, Switzerland. Cham, Switzerland: Springer;2019:119–125.
- Americans spend nearly half of their waking hours (42 percent) looking at a screen, it’s been revealed by new research. CooperVision. Accessed July 22, 2021. com/our-company/news-center/press-release/americans-spend-nearly-half-their-waking-hours-42-percent
- Stiglic N, Viner RM. Effects of screentime on the health and well-being of children and adolescents: a systematic review of reviews. BMJ Open. 2019;9(1):e023191. PubMed CrossRef
- Jericho M, Elliott A. Youth health in a digital world: approaching screen use in clinical practice. Clin Child Psychol Psychiatry. 2020;25(3):662–671. PubMed CrossRef
- United Nations. UN tackles ‘infodemic’ of misinformation and cybercrime in COVID-19 crisis |United Nations. Accessed July 22, 2021. un.org/en/un-coronavirus-communications-team/un-tackling-%E2%80%98infodemic%E2%80%99-misinformation-and-cybercrime-covid-19
- Wu X, Tao S, Zhang Y, et al. Low physical activity and high screen time can increase the risks of mental health problems and poor sleep quality among Chinese college students. PLoS One. 2015;10(3):e0119607. PubMed CrossRef
- Christensen MA, Bettencourt L, Kaye L, et al. Direct measurements of smartphone screen-time: relationships with demographics and sleep. PLoS One. 2016;11(11):e0165331. PubMed CrossRef
- Howard SK. Sleep deprivation and physician performance: why should I care? Proc Bayl Univ Med Cent. 2005;18(2):108–112, discussion 112–113. PubMed CrossRef
Enjoy free PDF downloads as part of your membership!
Save
Cite
Advertisement
GAM ID: sidebar-top